Regional Initiatives in Dental Education (RIDE)
- Need: Address oral health disparities in Washington's rural and underserved communities.
- Intervention: The University of Washington School of Dentistry developed the Regional Initiatives in Dental Education (RIDE) program preparing dentists for practice in rural and underserved areas.
- Results: As of 2019, 77% of all RIDE graduates are practicing in Washington state. Of those, 82% are practicing in rural and underserved communities.
Description
 Rural and underserved populations have
higher rates of dental caries and permanent tooth loss,
often due to economic disparities and distances from
dental providers. Many of these areas are
federally designated as dental health professional
shortage areas. A
2017 report by the University of Washington's Center
for Health Workforce Studies corroborates the lack of
dentists in rural areas.
Rural and underserved populations have
higher rates of dental caries and permanent tooth loss,
often due to economic disparities and distances from
dental providers. Many of these areas are
federally designated as dental health professional
shortage areas. A
2017 report by the University of Washington's Center
for Health Workforce Studies corroborates the lack of
dentists in rural areas.
To meet these dental care needs – with initial funding from Washington's state legislature in 2007 – the University of Washington's School of Dentistry (UWSOD) created the Regional Initiatives In Dental Education (RIDE) program. RIDE's 4 year curriculum focuses on training a "super-generalist" able to meet the challenges of an oral health practice in rural and underserved areas. Modeled after the University of Washington School of Medicine's WWAMI program (Washington, Wyoming, Alaska, Montana and Idaho), the young RIDE program is already experiencing early success placing dentists in rural/underserved areas in Washington and beyond.
The RIDE "hub" is in Spokane, and like WWAMI, similarly leverages regional university infrastructure for biomedical science instruction, and community practitioners for instruction on clinical rotations.

The RIDE dental students take first year courses with WWAMI medical students and will spend over 40% of their educational time in Washington's rural and remote areas. Distance learning also augments both biomedical and dental science instruction to ensure equivalency with UWSOD Seattle curriculum.
Dental science courses are taught by the faculty from Eastern Washington University's (EWU) Dental Hygiene program. These experienced senior faculty members are passionate about participating in RIDE's mission-based effort addressing oral health disparities. Classes with both dental and hygiene students lend to a valuable shared academic atmosphere.
The RIDE program also introduces dental students to teamwork concepts and holistic patient care models. Training occurs in an interprofessional setting with medical, dental, and dental hygiene students working alongside hygienists, nurse practitioners, physician assistants, physicians, pharmacists, nurses, behavioral health practitioners, and social workers.
RIDE's unique approach includes 5-6 months of extended intensive clinical training in Eastern Washington's Federally Qualified Health Centers (FQHCs). This includes experiences in oral medicine, oral surgery, periodontics, and pediatric dentistry designed to equip dental students with the additional skills often required in rural areas.
Multiple organizations recognize the public health and economic benefits resulting from RIDE's implementation. Support of the program comes from:
- University of Washington School of Medicine
- Eastern Washington University
- Federally Qualified Health Centers in Eastern and Central Washington
- Spokane District Dental Society
- Spokane Chamber of Commerce (Greater Spokane, Inc.)
- Washington State Dental Association
- Washington Dental Service Foundation
- State Legislators
- Washington State Board of Health
In 2017, the program was the recipient of the American Dental Education Association/Gies Foundation (ADEA Gies Foundation) Award for Vision, the highest national award based on "outstanding contributions to oral health and dental education."
Support and financial assistance came from multiple sources: HRSA ARRA grant, the Washington State Department of Health, the Washington state legislature, the American Dental Education Association, in addition to in-kind resources from the other institutions and organizations.
Services offered
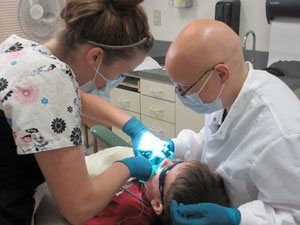 During community clinic
rotations, students see six to eight or more patients
daily, compared with two to three patients in the
standard dental curriculum. In addition to addressing
capacity needs, students also help provide much-needed
emergency care, including extractions and reduced
response time for patients with critical needs.
During community clinic
rotations, students see six to eight or more patients
daily, compared with two to three patients in the
standard dental curriculum. In addition to addressing
capacity needs, students also help provide much-needed
emergency care, including extractions and reduced
response time for patients with critical needs.
RIDE Curriculum Overview:
Year 1
- Spokane-based classes: The Spokane EWU Health Sciences campus site hosts most of the RIDE activities in the first year, with distance-learning technologies linking to Seattle.
- Small group learning: RIDE and Seattle-based students experience curriculum that minimizes lecture-based content, but instead requires student participation in small groups to promote critical thinking and development of self-assessment skills. The RIDE small group faculty to student ratio is 1:8.
Year 2 Summer
- First community rotation: All RIDE students participate in a 4-week rotation at a Community Health Center in Central or Eastern Washington (RUOP—Rural/Underserved Opportunities Program) to provide early exposure to the practice possibilities available in rural and underserved areas.
Years 2 and 3
- Seattle-based clinical training: These two years include preclinical dental courses and in-depth exposure to these specific dental specialties: oral surgery, endodontics, pediatric dentistry, orthodontics, oral medicine, periodontics, prosthodontics, and restorative and operative dentistry. Third year instruction is based on a "clerkship" model, with further intensive exposure to each subspecialty.
Year 4 Summer/Fall Quarters
- General Practice Clinic: Similar to their peers, RIDE students participate in the general practice clinic in Seattle and rotate through other specialized services such as Hospital Dentistry, Geriatric Dentistry, and Urgent Care.
- Winter/Spring's extended clinical rotations: Under supervision of community preceptors, these extended 4 to 5 month clinical rotations occur in Eastern and Central Washington's rural and remote FQHCs.
Additional RIDE-specific program features:
-
Mentoring: These EWU faculty and
community practitioners with careers dedicated to
dental care for the underserved mentor students:
- Spokane District Dental Society members
- CHC preceptors working one-on-one with students for 5-6 months
- UW Seattle and Eastern Washington University faculty with direct RIDE student oversight throughout the 4-year training
-
Small Group Interactions: These groups
provide:
- An environment for creating study groups, close relationships, peer support, social activity engagement, all beneficial for participating in the intensive RIDE curriculum track
- Formal faculty-facilitated online course for self-reflection activities which are further leveraged as a method of sharing clinical experiences
- This successful small group model has been adapted for the Seattle campus, for example small group instruction during Seattle clerkship rotations
Results
-
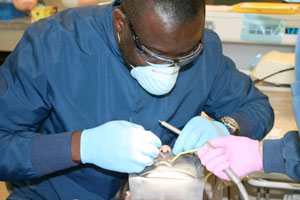 As of 2019, 77% of all RIDE
students are practicing in Washington state. Of those,
82% are in rural and underserved communities.
As of 2019, 77% of all RIDE
students are practicing in Washington state. Of those,
82% are in rural and underserved communities.
- Provision of 44,000 patient care hours in rural and underserved communities through the intensive community rotations in central and eastern Washington.
- Proven educational equivalency between RIDE and Seattle-based UWSOD curriculum
- High community preceptor satisfaction
- High student satisfaction rates
- Successful Commission on Dental Accreditation (CODA) site visits in 2012 and 2016.
- Local and state dental association support
- Positive community response
- Increased visibility for RIDE program itself as well as the School of Dentistry due to alignment with University's mission
-
Loan repayment opportunities:
- Graduates who work in Washington's FQHCs qualify for loan repayment programs through the National Health Service Corps.
- Washington's State Loan Repayment Program
- Other federal and state loan repayment opportunities are available for loan repayment for students with commitment to the military, Indian Health Service, and National Public Health Service (Commissioned Corps), as collated by the American Dental Association.
Challenges
 Major challenges
included:
Major challenges
included:
- Prolonged time interval to foster strong internal and external stakeholder support
- Meeting CODA standards at all program sites
- Engaging all community preceptors and regional faculty for CODA site visits
- Calibrating community faculty by university-based faculty
- Monitoring student data ensuring completion of all required curriculum and competencies prior to starting extended rotations and clerkships
- Creating win-win arrangements with community dentists and clinics for optimal clinical experiences
- Ensuring faculty-student oversight during community rotations
- Academic inter-institutional coordination for:
- Space, faculty and other resources
- Shared curricula schedule, timing and content
- Student housing
Replication
First envisioned in 2003, the RIDE program now has both deep and broad experiences translating to key elements for program replication.
First steps would include feasibility assessments in the following areas:
- Rural and underserved communities' unmet needs using workforce studies, population-based oral health surveys, and reports
- Degree of administrative support from key administrators within the dental school and the university
- Stakeholder support:
- Determine if degree of alignment with school mission/vision matches the endeavor of training professionals to deliver care to rural underserved populations
- Identify opposition as well as support among professional groups such as state and component dental associations, local communities, regional schools, community health centers, dental insurers, commissioner(s) of higher education, dental/dental hygiene and other health professional schools
- Dedicated faculty numbers – preferably from a variety of departments – committed to the mission of delivering dental care to underserved populations
- Resource availability:
- Faculty support, staff, distance learning, and other local considerations.
- Regional educational and clinical infrastructure
- Funding avenues: state funds for launch, with additional essential smaller commitments
- Create an ideal student persona
interested in providing care to underserved populations
which includes:
- Increased academic work
- Independent learning skills
- Logistical challenges associated with location changes
With feasibility determined, second comes development of a clear budget and project plan, followed by taking the program through required academic internal approval before ultimately presenting program to the state legislature. These steps may require two years or more.
This video provides a visual overview of UWSOD's innovative RIDE program:
Contact Information
Jennifer Grant, Director of Operations, Office of Regional Affairs & RIDEUniversity of Washington School of Dentistry
206.543.0903
jengrant@uw.edu
Topics
Dental workforce
Health workforce education and training
Oral health
States served
Washington
Date added
August 2, 2017
Date updated or reviewed
February 14, 2020
Suggested citation: Rural Health Information Hub, 2020. Regional Initiatives in Dental Education (RIDE) [online]. Rural Health Information Hub. Available at: https://www.ruralhealthinfo.org/project-examples/970 [Accessed 19 April 2024]
Please contact the models and innovations contact directly for the most complete and current information about this program. Summaries of models and innovations are provided by RHIhub for your convenience. The programs described are not endorsed by RHIhub or by the Federal Office of Rural Health Policy. Each rural community should consider whether a particular project or approach is a good match for their community’s needs and capacity. While it is sometimes possible to adapt program components to match your resources, keep in mind that changes to the program design may impact results.
