Frontier Community Health Integration Project (FCHIP)
Demonstration ended July 2019. Five-year extension period began July 1, 2021.
The Need for an Integrated Model in Frontier
Frontier areas are sparsely populated rural areas that are isolated from population centers and services and therefore face challenges in providing access to health services. Many frontier counties lack a hospital and frontier counties without healthcare professionals or hospitals are often clustered together which compounds the distance residents must travel to reach a hospital. Those frontier counties that do have hospitals may face higher costs than non-frontier hospitals, due to the lower volume of patients served. Because of these challenges, there is a need for integrating frontier systems of care in order to increase efficiencies and better coordinate patient care.
Project Purpose
The purpose of the demonstration was to develop and test new models for the delivery of healthcare services in frontier areas through improving access to, and better integration of, the delivery of healthcare to Medicare beneficiaries. The primary focus areas of the demonstration were to:
- explore ways to increase access to, and improve the adequacy of, payments for acute care, extended care, and other essential healthcare services provided under the Medicare and Medicaid programs in frontier areas; and
- evaluate regulatory challenges facing frontier providers and the communities they serve
Legislation Authorizing the FCHIP Demonstration
The Frontier Community Health Integration Project (FCHIP) demonstration was authorized under Section 123 of P.L. 110-275, the Medicare Improvements to Patients and Provider's Act of 2008 (MIPPA), and amended by Section 3126 of P.L. 111-148, the Patient Protection and Affordable Care Act (PPACA). The 5-year extension of FCHIP was authorized by Section 129 of P.L. 116-260, Consolidated Appropriations Act, 2021.
FCHIP Demonstration Participants
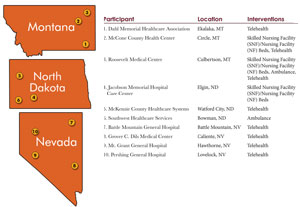
The Centers for Medicare & Medicaid Services (CMS) announced participants in the Frontier Community Health Integration Project Demonstration in August 2016. The 10 participating Critical Access Hospitals and the interventions they focused on:
| Participants | Interventions |
|---|---|
| Dahl Memorial Healthcare Association* Ekalaka, MT |
Telehealth |
| McCone County Health Center Circle, MT |
Skilled Nursing Facility (SNF)/Nursing Facility (NF) Beds Telehealth |
| Roosevelt Medical Center* Culbertson, MT |
Skilled Nursing Facility (SNF)/Nursing Facility (NF) Beds Ambulance Telehealth |
| Jacobson Memorial Hospital Care Center* Elgin, ND |
Skilled Nursing Facility (SNF)/Nursing Facility (NF) Beds |
| McKenzie County Healthcare Systems* Watford City, ND |
Telehealth |
| Southwest Healthcare Services* Bowman, ND |
Skilled Nursing Facility (SNF)/Nursing Facility (NF) Beds Ambulance Telehealth |
| Battle Mountain General Hospital Battle Mountain, NV |
Telehealth |
| Grover C. Dils Medical Center Caliente, NV |
Telehealth |
| Mt. Grant General Hospital Hawthorne, NV |
Telehealth |
| Pershing General Hospital Lovelock, NV |
Telehealth |
| *Participating in the five-year extension. Southwest Healthcare Services added telehealth intervention to its participation agreement in January 2024. Source: Frontier Community Health Integration Project (FCHIP) Demonstration Extension Fact Sheet | |
Eligibility to participate in the demonstration project was defined in the authorizing legislation and limited to “eligible entities”. CMS interpreted the eligible entity definition as meaning Critical Access Hospitals (CAHs) that receive funding through the Medicare Rural Hospital Flexibility Program. The statute limited the demonstration to no more than four States and restricted eligibility to CAHs in States in which at least 65 percent of the counties had six or fewer residents per square mile. CMS selected participants from Montana, Nevada, and North Dakota (though eligible to apply, CAHs in Alaska and Wyoming did not apply).
Partners
In fiscal year 2010, Congress appropriated funds to the Federal Office of Rural Health Policy (FORHP) for the FCHIP demonstration. FORHP funded an 18-month cooperative agreement award to the Montana Health Research & Education Foundation (MHREF) to provide information and data to CMS as they develop this demonstration. In order to identify and communicate the challenges and solutions MHREF hoped to convey to CMS, a Framework Document and subsequent topical white papers were prepared.
FORHP also provided funding to the Medicare Rural Hospital Flexibility Program in North Dakota, Alaska and Wyoming to respond to the framework document and white papers produced by MHREF and provide CMS any additional regulatory proposals not addressed in the original framework or white papers.
More Information on the FCHIP Demonstration
- Frontier Community Health Integration Project (FCHIP) Demonstration Extension Fact Sheet
- Report to Congress: Demonstration Project on Community Health Integration Models in Certain Rural Counties - Final Report
- Frontier Community Health Integration Project Demonstration: Final Evaluation Report
- Report to Congress: Demonstration Project on Community Health Integration Models in Certain Rural Counties, Interim Report 2018
- FCHIP Frequently Asked Questions
- Framework for a New Frontier Health System Model
- Frontier Referral, Admission and Readmission Patterns
- Case Study on Frontier Telehealth
- Frontier Quality Measures and Payment for Performance
- Frontier Care Coordination & Long-Term Care
- Frontier Healthcare Workforce
- Frontier Health System Reimbursement
- Frontier Community Health Integration Demonstration Program: Alaska White Paper
FCHIP Program Contact:
Sarah Heppner, Federal Office of Rural Health
Policy
sheppner@hrsa.gov
301.443.5982