Aug 05, 2015
Technology Stemming from Tragedy
by Kate Menzies
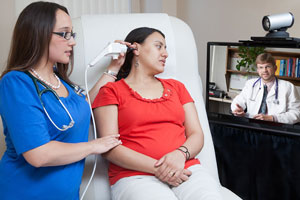
For Finger Lakes Community Health (FLCH), a rural Federally Qualified Health Center, a telehealth program was a solution inspired by tragedy. In 2004, one of FLCH's RNs was traveling to a Migrant Head Start site to provide services to children, when she was fatally struck by another car. Two years later, an FLCH community health worker suffered brain damage from being hit head-on by another vehicle after he had just transported a patient to a specialty care appointment. Both of these incidents occurred when providers were traveling between FLCH sites.
Something had to be done to prevent future fatalities.
"Our workers compensation insurance was one of the higher in the state of New York," said Director of Special Programs at FLCH, Sirene Garcia. "The transportation costs and the liability from going site to site were a huge expense for us."
FLCH decided to make better use of their staff's time and reduce the liability insurance expense of providers by creating the Finger Lakes Telehealth Network (FLTN).
"Telehealth was kind of a no-brainer," said Mary Zelazny, CEO of FLCH. "The return on investment was as great as the reimbursement potential."
In January 2015, the governor of New York signed a bill mandating that telemedicine and telehealth be covered by insurance, with Medicaid also reimbursing for telehealth services beginning in January of 2016.
Reimbursements have become the Holy Grail of telehealth.
"Reimbursements have become the Holy Grail of telehealth," said Zelazny.
FLTN is unique in that it provides an open access network to more than 20 partnering organizations, including several health center sites, giving these establishments the opportunity take advantage of telemedicine, distance learning, and administrative telepresence applications, without having to invest time, money, and effort in infrastructure and network development. Partners are required to pay a small subscription fee to join the network, but are able to receive telehealth broadband services at a 65% discount.
"This enables us to create bridges with other agencies," said Garcia. "It forces us to communicate with each other so providers aren't working in siloed environments."
This enables us to create bridges with other agencies.
For patients, telehealth enables them to choose among a variety of available providers, as well as offering greater access to specialty care. Primary care providers are able to work closely with specialists and hear first-hand recommendations for courses of action. As a result, quality of care for patients increases with the greater availability of shared resources.
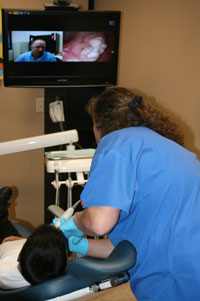
"It's going to transform our health system," said Zelazny. "Telehealth is going to assist us as we shift to a value-based pay system."
For FLCH, this telehealth network represents a step forward in finding ways for patients to receive care, without increasing transportation costs. Telehealth utilizes technology to reduce costs in the healthcare system and improve the quality of care available to patients.
"Better access to care equals better health outcomes, which in turn means less stress on the system," said Zelazny. "That's why we are here."
