Aug 20, 2014
Telehealth Invigorating and Innovating Diabetes Care
Dr. Hilary Canipe used to wish she had a way to look into her diabetic patients' day-to-day lives rather than only seeing them in her office. Now she does. “Telehealth home monitoring is a powerful tool that has given me a window into patients' homes to understand what is happening with them,” said Canipe, a primary care physician with Roanoke Chowan Community Health Center (RCCHC) in Murfreesboro, North Carolina.
Telehealth for diabetes provides for tighter glucose control, improved clinical outcomes, reduced hospitalizations, and closer screening that prevents or arrests development of serious complications, according to Dr. Kamal Jethwani, Corporate Manager for Research and Innovation at the Boston-based Center for Connected Health (CCH).
“Remote monitoring is changing the epicenter of the delivery system by decentralizing decision-making and empowering patients to take better care of themselves,” Jethwani said. “Patients with chronic illness used to end up in the hospital and go back home with some guidance but little education on what might happen to them or how they needed to care for themselves. Usually, they defaulted on the instruction they got and ended up back in the hospital.” Now, he said, the data that was being collected in clinics or hospitals is something they can do at home. And qualified nurses and professionals monitor them and respond quickly, when needed. “One study even showed a 50 percent drop in mortality with telehealth intervention,” he said.
In nine western New York counties, diabetes is among the top five diagnoses for patients served by the Visiting Nursing Association (VNA) of Western New York. To improve reimbursements for diabetes care, VNA demonstrated that, in the last year, 80 percent of diabetic telehealth patients reduced their A1C levels, some by as much as 6.9 points.
“Some of our patients were at 13 or higher and have come down to almost normal ranges,” said Lisa Greisler, Vice President and Chief Operating Officer. “Diabetes has a lot of complications. Every individual reacts differently. With telehealth, we are able to help them on a daily basis. Once patients realize what a difference they can make in their health, they become committed to managing their disease. It's been amazing to watch the changes.”
VNA, a home health agency which has used telehealth for chronic disease monitoring since 2005, averages about 400 to 600 telehealth patients and 420,000 home visits per year. In North Carolina, Canipe's patients are enrolled in RCCHC's Patient Provider Telehealth Network (PPTN). RCCHC initiated PPTN in 2008 as a three-year feasibility study. Of the 198 patients in the study, data revealed decreases of 92 percent in hospitalizations, 89 percent in length of stays and 67 percent in emergency visits. RCCHC, a Federally Qualified Health Center (FQHC) with locations in Ahoskie, Colerain and Murfreesboro, currently serves approximately 275 diabetic patients living in 28 counties in the state.
Monitoring at Home

“Having this technology in the home has been such an advantage for my patients,” Canipe said. “I can talk with them more accurately about their problems because I have this additional information. They feel more connected and have more control of their disease.”
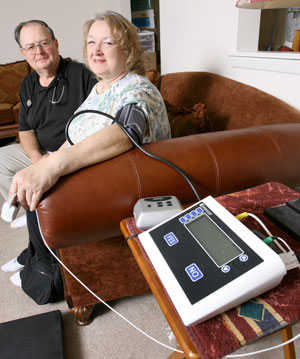
Each morning, patients weigh themselves and check blood pressure, pulse, blood sugar levels and oxygen saturation. They also answer a series of varying questions relative to possible diabetes complications on an easy-to-use, small store-and-record unit in their home, which securely transmits the data to nurses at a central location. If indicators are outside normal parameters, nurses intervene with a follow-up telephone consultation and/or a home visit. The primary care provider is also notified, either through the patient's electronic health record (EHR) or by direct contact if the issue deserves more immediate attention.
Patients are referred for telehealth by their primary care physicians, who can customize monitoring and reporting to the individual patient's needs. Prior to beginning home monitoring, patients receive instruction in performing the daily assessments and must demonstrate competency. Telehealth does not replace doctors' appointments or home visits. It extends rural providers' capabilities, Greisler said, because one centralized nurse can observe and respond to numerous patients in a timely manner. Patients fare better because their physicians can adjust medications and diet regimens based on daily data.
“The nurses do such a good job that it reduces the need for office visits because problems that could have festered and been big issues by the time I saw the patient don't get that far,” Canipe said. “The diabetes education has improved patients' self-management skills too.”
Expanding Telehealth
CCH has been involved in several technology-centered programs for improving chronic disease management. Currently, Jethwani said, a diabetes management pilot using text messaging looks very promising. CCH has been testing the product with an underserved urban population. Within six months, it should be widely available.
“Traditionally, we see only about 15 percent of patients consistently increasing their physical activity, which is one of the American Diabetes Association recommendations and seems to be one of the hardest things for people with diabetes to incorporate into their lifestyle,” he said. “Our patients are using trackers to encourage consistent physical activity.”
The trackers connect directly to patients' EHRs and analyze their activity levels and frequency. Patients receive daily behavioral instruction text messages personalized to their individual patterns. Although study data has not yet been released, Jethwani said patients have experienced better clinical improvement as measured by A1C changes than what an approved oral medication can achieve in six months.
“These patients are beating medication usage or increase by increasing their activity,” he said. “The patients are really engaged because the system is very personalized and interactive. We are hoping to build on this engagement with the next version we've begun.”
For chronic disease management to become more universally available, proponents say reimbursements must improve. VNA hopes to prove the value of diabetes telehealth and contribute to reimbursement reforms with its four-year telehealth study begun in 2013 with a $1 million grant from the Health Resources and Services Administration (HRSA) Telehealth Network Grant Program. VNA has partnered with three physician groups to provide telehealth for 75 diabetic patients living in Chautauqua and Genesee counties, which are heavily rural with large underserved populations and diabetes rates above the national average.
“If we can prove that using telehealth for diabetes improves patient health while reducing costs, that will have a big impact on how telehealth is reimbursed,” Greisler said. “In the United States, people with diabetes incur average medical expenditures of $13,700 annually with $7,900 attributed specifically to diabetes.”
VNA has successfully demonstrated the effectiveness of telehealth in reducing acute care hospitalizations through at-risk pilot programs with local payers and participation in a New York State demonstration project for telehealth. Greisler said the pilot programs' success led to negotiations with local payers that now cover telehealth services. She noted that this type of reimbursement is still “very rare throughout the country.” RCCHC's program is funded by multiple state grants, federal and private grants, and partnerships with other organizations such as Community Care of North Carolina.
As reimbursement improves, and with increasing numbers of the population becoming more tech savvy, personalized health care using phone, web-based and other types of telehealth applications will continue to increase, Jethwani said. “More than 80 percent of our patients go online now. Even in underserved areas, many more people have cell phones. Our analytics are getting smarter and programs are getting better. All of this results in more direct access to people. Across the country we are going to see much higher adoption of programs that provide a lot of health care services through self service.”
Back to: Summer 2014 Issue
