Avita Health System Comprehensive Cardiology Program
- Need: Population health approach to decrease cardiovascular disease deaths in a rural Ohio healthcare delivery system's service area.
- Intervention: A rural health system's investment in level II cardiac catheterization services and the required specialized cardiology workforce.
- Results: In August 2018, Avita Health System started their cardiovascular service offerings in rural north central Ohio. Early results included decreased tertiary care hospital transfers. Building on the success of their increased ability to provide acute care, care coordination for patients with significant cardiovascular risks, preventive education with risk factor identification and modification, the health system continues to expand its local cardiovascular care.
Description
In the mid-2010s, state-level statistics from the Ohio Department of Health identified Crawford County as having a higher tier of cardiovascular disease death rates compared to other Ohio counties. This data — combined with the fact that cardiovascular disease remains the leading cause of death in Ohio and in the country's rural and urban areas as a whole — prompted the rural Avita Health System (AHS) to analyze its patients' cardiovascular needs.
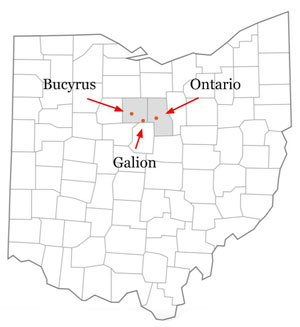
In its original analysis, AHS, a 3-hospital system — including two Critical Access Hospitals (CAHs) — found that about 300 patients per year were requiring transfer from its local rural system to surrounding tertiary medical centers. Two patient groups emerged from this data review: patients experiencing an acute ST-elevation myocardial infarction (STEMIs) and patients with significant cardiovascular risks who were experiencing chest pain of cardiac origin but without evidence of an acute heart attack. For these two groups, research demonstrates that immediate interventional cardiology procedures improve outcomes and lower death rates. Also with the original analysis, a side-by-side review focused on potential cardiovascular services that AHS could support that might offer the greatest impact on their patients' cardiovascular health.
With the comprehensive analysis concluded, discussions began around the potential implementation of level II cardiac catheterization services, understanding that a considerable financial investment would be required to construct and maintain catheterization suites. Also acknowledging the challenges around recruiting and retaining a specialized workforce to perform these services, the AHS board made a commitment to offer these services to nearly 42,000 residents in their Crawford County service area, inclusive of those receiving care at their Galion and Ontario CAH hospital locations. In 2018, the 24/7 interventional cardiology department began offering not only immediate impactful interventional cardiac procedures, but many other non-procedural cardiology services.
With implementation, the presence of local cardiovascular care was found to have additional impacts outside of acute procedural interventions, starting with patient care coordination with other medical specialties. For example, because the region's population has significant issues with cardiovascular surgical risk factors, such as hypertension, hypercholesterolemia, obesity, and inactivity, patients with these cardiovascular risks who might otherwise be referred to a larger facility for surgery were able to receive procedures locally as cardiologists were now available to manage any post-operative cardiovascular needs.
Less frequently referenced as connected to the presence of AHS cardiovascular specialty care are other benefits linked to keeping patients local. Research repeatedly finds that care availability in rural patients' home communities positively impacts outcomes — along with decreasing families' transportation costs and lost work hours linked to the need for family members to be present when care is provided at a distant facility.
Another program goal was preventive education, initially limited in early months of implementation due to the COVID-19 pandemic. Now the organization has been able to strategically add not only prevention activities through community seminar offerings and health fair cardiovascular risk assessments, but also by expanding risk factor testing. Because prevention also depends on risk factor identification and modification, additional offerings range from heart artery calcium testing to genetic testing that identifies conditions like high lipoprotein (a) levels, often referred to as LP(a), a protein linked to stroke and heart attack risks in otherwise healthy people with normal cholesterol profiles. Of note, there are mandatory education components in the cardiac rehabilitation programs now offered in all three hospitals.
To assure quality in its cardiovascular service offerings, the organization participates in the American College of Cardiology's National Cardiovascular Data Registry (NCDR) in order to measure outcomes, analyze quality of care, and allow comparison to national benchmarks. Routine internal workflows include peer review of all heart attack cases and cardiovascular quality measures review.

Services offered
Unique rural cardiovascular services:
- Emergency heart attack care 24 hours a day, 7 days
per week, 365 days a year
- Call rotation includes both a general and interventional cardiologist 24/7/365
- On-site, on-call cardiologist at each hospital of the system's hospitals weekdays from 8:00am – 4:00pm.
- Pulmonary Embolism Response Team
- Inpatient cardiovascular consultations
- Same day/next day cardiology office appointments
- Accredited cardiac rehabilitation programs in all three hospitals
Several additional services from the organization's comprehensive list of cardiovascular services include:
- Cloud-based notification system allowing field paramedics to provide hospital care teams with pre-arrival critical patient data that decreases time so critical for STEMI treatment
- Noninvasive cardiology testing including stress test, echocardiography and vascular testing
- Pacemaker placement and monitoring
- Remote intrapulmonary monitoring for congestive heart failure patients
- Deep venous thrombosis (DVT) clinic
- Vein ablation
- Other cardiovascular health assessment tests and procedures:
-
Cardiovascular genetic testing
- For example: Lipoprotein (a) or LP(a)
- Coronary calcium scoring
- Cardiac Computed Tomography Angiography (CCTA)
Results
Initial August 2019 implementation results:
- Over 1,000 procedures performed
- Over 300 pacemakers and implantable loop recorders placed with ongoing monitoring
- Transfers for acute myocardial infarctions ceased
- Transfers for conditions with a differential diagnosis that includes potential for an acute cardiac issue ceased
Post-implementation 2020 quality metrics included:
- Acute myocardial infarction door-to-treatment AHS
time at 51 minutes
- Compared to the national benchmark of 90 minutes
- Favorable rating on all NCDR quality metrics
More recent years' results:
- A 95% decrease in transfers
- Transfers still occurring are those requiring a higher level of care, like heart bypass surgery
- Cardiac rehab programs experienced a double-digit growth since about 2020
- Although difficult to determine AHS's cardiovascular services as having a direct causal link, recent changes in Crawford County deaths are notable: In 2020, cardiovascular deaths numbered 204; and in 2024 numbered 128, a 40% decrease.
Regarding the financial risks associated with new cardiovascular services start-up in a rural setting, health system administrators believe the services, in part, are responsible for strengthening the healthcare delivery system's financial foundation and adds to the needed stability to ensure its future existence.
In 2019, the health system was recognized as the first Critical Access Hospital in the U.S. to use supersaturated oxygen therapy for acute heart attacks and to implant remote monitoring devices in order to better care for advanced heart failure patients.
This video shares a local patient's perspective of his care from the Avita heart program:
Challenges
Initial implementation challenges:
- Multi-million dollar initial investment in equipment, training, and workforce.
- Altering EMS field transfer patterns with well-established programs even after becoming the closest level II cath lab.
Ongoing challenges related to interventional cardiologist-linked workforce recruitment/retention:
- Cardiology workforce is experiencing a growing shortage due to retirements and fewer physicians entering the specialty, amplified by the needs linked to the aging of America — especially rural America, where there exists a high prevalence of cardiovascular risk factors linked to diabetes, hypertension, and obesity
- Employee migration due to hiring bonuses
Replication
Although large urban healthcare systems that acquire smaller rural systems promote "hub-and-spoke" models, AHS leadership recognized this strategy has also led to closure of rural hospitals.
- Investing in its own cardiovascular services allowed AHS to remain a community health system independent of a larger metropolitan health system and its governance system allows decision-making to focus on prevention and care needs of its local service area, as evidenced by the Avita Heart Program.
- Employment of a cardiology director with cath lab start-up experience and workforce recruitment duties was key in the start-up.
Keeping these factors in mind — in addition to a recent increase in cardiovascular deaths found in younger rural adults — other rural community hospitals wanting to impact the health and well-being of their population by targeting cardiovascular disease might want to consider implementing a comprehensive cardiology program with a level II cardiovascular lab to provide local life-saving care and services that can decrease transfers and keep care local. In the long-term, the financial status of the organization may also see positive results and influence the stability of their existence.
Contact Information
Michael Davis MD MBA, MPH, FACHE, Medical DirectorCardiac Catheterization Services, Avita Health System
614.886.5744
mpdavis@avitahs.org
Topics
Access
· Cardiovascular disease
· Care coordination
· Chronic disease management
· Critical Access Hospitals
· Governance of healthcare organizations
· Health conditions
· Health disparities
· Healthcare networks
· Hospitals
· Inpatient care
· Outpatient care
· Population health
States served
Ohio
Date added
April 19, 2021
Suggested citation: Rural Health Information Hub, 2026 . Avita Health System Comprehensive Cardiology Program [online]. Rural Health Information Hub. Available at: https://www.ruralhealthinfo.org/project-examples/1088 [Accessed 5 June 2026]
Please contact the models and innovations contact directly for the most complete and current information about this program. Summaries of models and innovations are provided by RHIhub for your convenience. The programs described are not endorsed by RHIhub or by the Federal Office of Rural Health Policy. Each rural community should consider whether a particular project or approach is a good match for their community’s needs and capacity. While it is sometimes possible to adapt program components to match your resources, keep in mind that changes to the program design may impact results.
