Fostering Futures in Menominee Nation
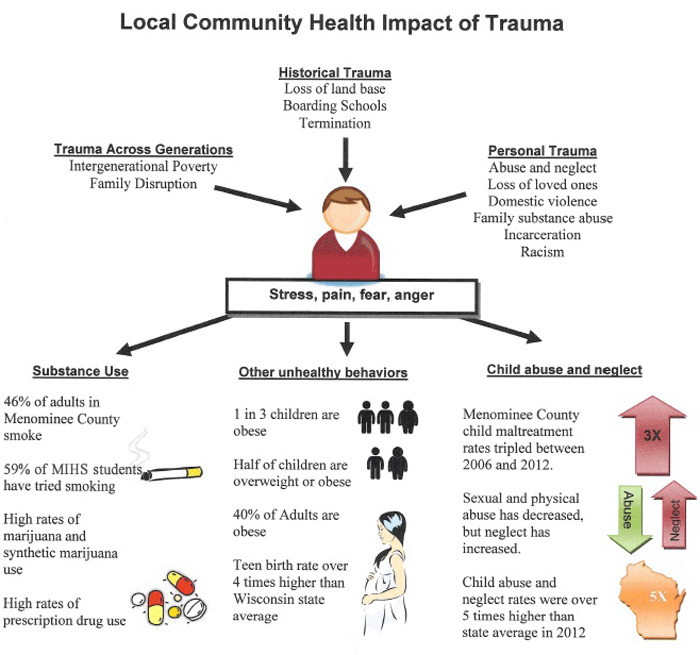
- Need: Since the late 1800s, trauma caused by historic events have greatly affected the way of life for Menominee Indians living on the Menominee Reservation. Economic, socioeconomic, behavioral health, and physical health issues have risen and are causing direct implications for Menominee youth.
- Intervention: Through Fostering Futures, clinic, school, and Head Start/Early Head Start staff are trained in administering trauma-informed care and building resilience among children.
- Results: Behavioral health visits at the Menominee Tribal Clinic have increased, school suspension rates have decreased, and graduation rates have improved from 60% to 94% since 2008.
Description

The Menominee Indian Reservation is home to 4,000 of the 9,000 members of the Menominee Tribe. Trauma has deep roots in the tribe because of significant past events. Beginning in 1860, children were forcibly removed from their homes and sent to boarding schools to learn Western culture. In the 1950's, the tribe's federal recognition was terminated and many Menominee between the ages of 18 and 54 had to leave the reservation in search of employment. The loss of the generation responsible for the development of the emotional and intellectual capacity of children was devastating.
Menominee's economic and socioeconomic decline and rise in poverty and health disparities are just some factors Menominee County's health outcomes ranking has been 72 out of 72 Wisconsin counties since 2007. According to research from the Robert Wood Johnson Foundation and a University of Wisconsin Population Health Institute epidemiologist, the reasons behind the following statistics can be traced back to trying times in Menominee Nation's history:
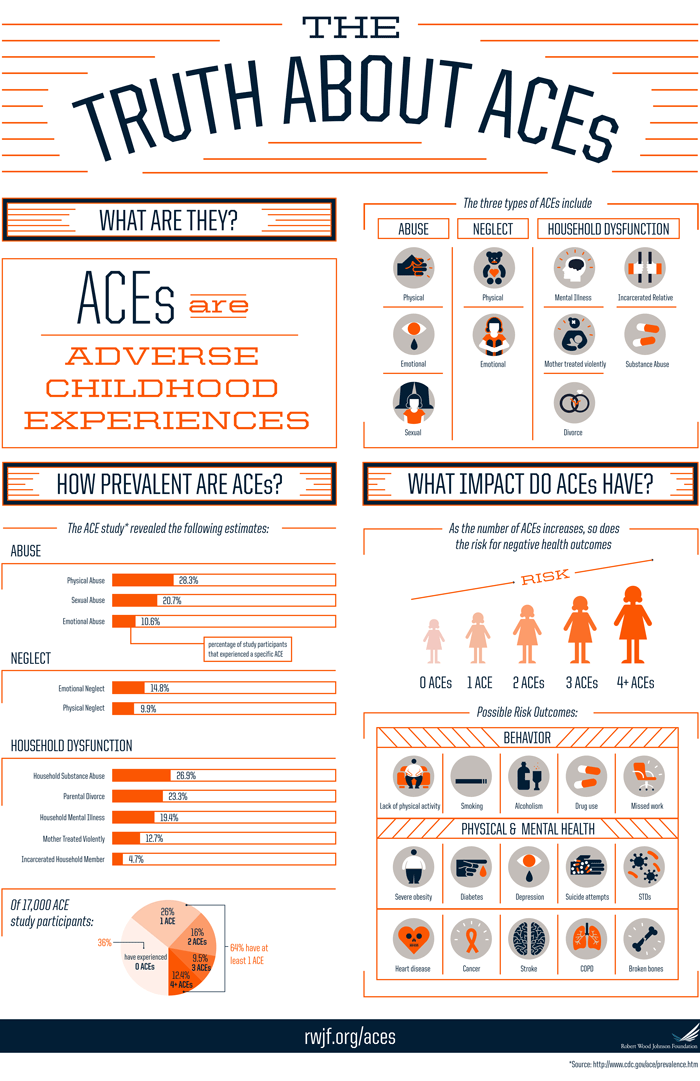
In 2010, leaders of the Menominee Tribal Clinic and the Menominee Indian School District developed the Community Engagement Workgroup. The group is made up of multiple community representatives who seek out solutions for these trauma-induced realities. In 2011, the Tribe volunteered to be a part of a state-wide pilot project called Fostering Futures. Through this project, the workgroup can offer trainings and other initiatives to help staff administer trauma-informed care (TIC) to reverse negative effects of adverse childhood experiences (ACEs) and build resiliency among children.
The Community Engagement Workgroup includes all 41 departments of tribal government, county human services, the school district, and college. A core and advisory team representing these local agencies assists with the implementation of Fostering Future's practices across the community:
- Menominee Tribal Clinic
- Menominee Indian School District
- Menominee Indian Tribe of Wisconsin
- Menominee County Board of Supervisors
- Menominee Tribal Family Services
- College of Menominee Nation
- University of Wisconsin
- Great Lakes Inter-Tribal Epidemiology Center (GLITEC)
- Menominee County Human Services
- Maehnowesekiyah Wellness Center
Fostering Futures continues to receive financial support from the Menominee Indian Tribe of Wisconsin, Menominee County Board of Supervisors, Menominee Indian School District, and the State of Wisconsin Department of Children and Families.
Services offered
This collaborative effort has spurred a cultural shift through trauma-informed care services in the schools, clinic, and community.
Clinical Services:
The Menominee Tribal Clinic created a trauma-informed care team made up of clinical staff who meet regularly with a trauma informed care coordinator to formulate strategies and conduct trainings. This team includes a Wisconsin ACE Interface Master Trainer who is available for community trainings.Menominee Tribal Clinic's Behavioral Health Department consists of:
- 11 full-time staff members
- 3 Licensed Professional Counselors
- 1 Licensed Professional Counselor In-Training
- 2 Licensed Clinical Social Workers
- 1 Advanced Practice Social Worker
- 1 case manager
- 1 Registered Nurse
- 2 support staff
The department contracts:
- 1 psychiatrist
- 2 psychiatric advanced practice nurse practitioners

The clinic also started the Pediatric Integrated Care Collaborative (PICC) to integrate the medical and behavioral health departments for better patient care coordination. Through PICC, children and their families are screened for trauma and receive support to build resiliency and prevent future exposure to trauma. The Menominee Tribal Clinic was 1 of 6 sites in their cohort across the nation that has implemented PICC, a project supported by the Substance Abuse and Mental Health Services Administration (SAMHSA) and Johns Hopkins University.
School-Based Services:
Through a Safe Schools/Healthy Students grant, Menominee Indian School District set up a Student Health Center that offers behavioral health services. A trained trauma coach is also available to work individually with students. The Student Health Center is staffed with a counselor and social worker. Screening, Brief Intervention, and Referral to Treatment (SBIRT) are available if there are concerns of substance use.
Each classroom at Keshena Primary School starts the day with meditation and mood check-ins so that teachers are aware of their students' emotional state. "Safe zones" allow the children a place in the classroom to visit whenever they need space and regulation. The "Sakom Room" (Menominee word for "peace") is a calm setting outside of the classroom where the student can get further help from a trained trauma coach who helps the student through the emotions so he or she is ready to learn again.
Teaching high schoolers Menominee culture and values has been reestablished at Menominee Indian High School. Menominee Grandfather Teachings such as wisdom, respect, honesty, and truth back up additional teachings of culturally-relevant reproductive health and support services for girls. The Maehnow Pematesan coalition also puts on drug-free cultural events to promote sobriety.
Through Head Start/Early Head Start's Trauma Start program, the Crittenton Children's Center offers monthly trainings and events for all professionals, staff, and parents who interact with Head Start, Pre-K, and Kindergarten students.
Community Services:
Two community campaigns were created by Fostering Futures to spread awareness of ACEs, TIC, and resilience through cultural principles. "Ketapanen" (Menominee for "I love you") encourages positive parenting, and "Think" encourages strength-based language and kindness. Trauma training is offered quarterly at the Community Resource Center and is open to everyone.As the Community Engagement Workgroup started working more closely with families through Fostering Futures, they discovered an urgent need for parent and family education trauma. Fostering Futures developed a video series of TIC modules used for training and community/family awareness. Monthly newsletters are distributed throughout the tribe that include TIC information.
Results
In the Clinic:
In 2021, 7,034 appointments were made with the Menominee Tribal Clinic's Behavioral Health Services, an increase compared to 3,145 appointments in 2014.The clinic staff completed a year-long curriculum on the principles of trauma informed care that included the topics: Applying TIC, Historical Trauma, ACEs, Brain Development, Epigenetics, Resilience, De-escalation, Self-Care and Health and Trauma. Pre- and post-test scores showed staff developed a much better understanding of the topics.
Two staff members of the clinic (the clinic administrator and the care coordinator) have joined Johns Hopkins University as faculty members. Two recent cohorts of the PICC project are made up of Indian Health Service (IHS) clinics. Through this project, 16 IHS clinics were informed about trauma informed practices and learned from the Menominee Model.
A care coordinator has been added to the staff in the medical department. This position acts as a liaison between the medical and behavioral health departments and also delivers brief intervention behavioral health services to medical patients.
In the Schools:
- Since 2008, high school graduation rates in Menominee County have increased from 60% to 94%.
- Annual birth rate to girls ages 15-17 have dropped from 20 in 2008 to 5 in 2015 and 3 in 2021.
- Over the past decade, substance use rates have decreased, including use of marijuana (by 30%), cigarettes (by 49%), and alcohol (by 64%).
- An increased number of students have entered post-secondary education.
- School suspension and expulsion rates have decreased.
- Restorative practices are taking effect as there has been a visible change in students' resiliency and health.
In the Community:
The number of people who have participated in the Community Engagement Workgroup has grown from 40 to 100 since its founding.This video, derived from the Menominee Nation, Wisconsin RWJF Culture of Health Prize project, depicts more initiatives and results from the Menominee Tribe (Copyright 2015. Courtesy of the Robert Wood Johnson Foundation).
Below are some recognitions of the Fostering Futures program and Menominee Nation's implementation of it:
- Fostering Futures has been one of several trauma-confronting initiatives across the nation that have spurred conversations among U.S. senators on the issue.
- In 2015, the Menominee Tribe was a Robert Wood Johnson Foundation Culture of Health Prize Winner.
- Menominee's trauma prevention efforts were presented during a 2014 U.S. Senate Committee on Indian Affairs Round Table. Menominee Nation continues working with Mr. Daniel Press, a lawyer in Washington DC, to further trauma-informed care in Indian Country.
- American Public Health Association published an overview of Menominee's trauma-informed framework in a publication entitled Harnessing the Power of Cross-Sector Collaboration.
- Congressional Resolution H. Res 443 – Recognizes the importance and effectiveness of trauma informed care while specifically naming the Menominee Tribe.
The following communities are adopting trauma-informed care principles from Menominee's Fostering Futures program:
- Eastside Native American Education Program in Redmond, WA (Okanagan Nation)
- Paschal Sherman Indian School in Omak, WA (Colville Band of Confederated Tribes)
Challenges
- The stigma of behavioral health often makes patients hesitant to receive behavioral health services.
- Treating patients' trauma when they are already in crisis mode is always more difficult than if catching it in the early stages.
- Since there is a high prevalence of trauma in patients at the Menominee Tribal Clinic, healing takes time. Establishing change happens slowly.
Replication
- Getting support and champions from tribal or community leaders, stakeholders, and federal and state programs is key to building a sustainable model.
- Establishing champions from the medical and behavioral health departments is vital to the success of delivering trauma-informed care.
- Be transparent with your patients, community, and other programs. Transparency helps to build accountability for the goals you set.
- Before initiating trauma-informed care, establish care coordination between medical and behavioral health departments within your clinic while keeping a patient-centered approach.
- Use data collection methods to determine your community's needs and evaluate the effectiveness of your initiative. Develop a 90-day plan, hire staff, and then take action. Stick to your plan and use business strategies like SWOT Analyses to evaluate progress.
- Developing a good model does not guarantee funding. Look for unconventional sources of income from multiple avenues to support your project.
- Before confronting the issue of trauma, the Community Engagement Workgroup addressed more tangible issues such as obesity and dental care. Since the start of the initial conversations, implementing Fostering Futures took nearly a decade, but resiliency and persistence paid off.
- Behavioral changes may take years before results are evident. Be realistic with your expectations while working to improve your community.
The following resources are used by the Fostering Futures initiative to help educate organizations and individuals that work with trauma victims:
- Resiliency/Stress Questionnaire published by the Wisconsin Coalition Against Sexual Assault
-
Finding
your ACE Score published by the ACEs Too High
- Parenting a Child Who Has Experienced Trauma published by the Child Welfare Information Gateway
- Stress and Early Brain Growth, Understanding Adverse Childhood Experiences (ACEs) published by the Community & Family Services Division at the Spokane Regional Health District
- Logic Model in partnership with the University of Wisconsin-Extension and the Great Lakes Inter-Tribal Epidemiology Center (GLITEC)
- Learning Collaborative Toolkit: Improving the Capacity of Primary Care to Serve Children and Families Experiencing Trauma and Chronic Stress
The Menominee Nation Fostering Futures program was inspired by several key sources:
- Bridges out of Poverty strategies - Jodi Pfarr, facilitator
- Teri Berila and Jim Sporleder in Walla Walla, WA
- Heather Forbes from the Beyond Consequences Institute
- Avis Smith from the Trauma Smart preschool program
Contact Information
Jerry Waukau, Tribal Health AdministratorMenominee Tribal Clinic
715.799.5482
jerryw@mtclinic.net
Topics
American Indian or Alaska Native
Behavioral health
Behavioral health workforce
Care coordination
Child welfare
Children and youth
Community and economic development
Culture and cultural competency
Home and community-based services
Integrated service delivery
Networking and collaboration
Schools
Trauma-informed care
States served
Wisconsin
Date added
August 18, 2016
Date updated or reviewed
August 24, 2022
Suggested citation: Rural Health Information Hub, 2022. Fostering Futures in Menominee Nation [online]. Rural Health Information Hub. Available at: https://www.ruralhealthinfo.org/project-examples/924 [Accessed 11 December 2024]
Please contact the models and innovations contact directly for the most complete and current information about this program. Summaries of models and innovations are provided by RHIhub for your convenience. The programs described are not endorsed by RHIhub or by the Federal Office of Rural Health Policy. Each rural community should consider whether a particular project or approach is a good match for their community’s needs and capacity. While it is sometimes possible to adapt program components to match your resources, keep in mind that changes to the program design may impact results.