Community Care Partnership of Maine Accountable Care Organization
- Need: To increase access and quality of care for patients in rural Maine.
- Intervention: Community hospitals and Federally Qualified Health Centers in Maine formed the Community Care Partnership of Maine Accountable Care Organization (CCPM ACO).
- Results: CCPM serves about 250,000 patients in Maine every year. In addition, it has implemented shared savings arrangements/contracts with different Medicare Advantage and other private health payers.
Description
The Community Care Partnership of Maine Accountable Care Organization (CCPM ACO) began in 2015 when a Federally Qualified Health Center (FQHC) and community hospital started to collaborate. Now the CCPM ACO involves 17 FQHCs and five community hospitals that operate as a clinically and financially integrated network and serve 250,000 patients annually. By sharing infrastructure; reducing duplication; and piloting initiatives that improve quality, cost efficiency, access to care, and the patient and care team experience, members of CCPM achieve economies of scale that sustain local care in rural communities.
The CCPM ACO negotiates and manages shared savings across the network. It has earned shared savings for eight consecutive years under Medicare's Shared Savings Program, generating more than $120 million over the last several years. Most of these dollars are reinvested into member organizations, based on patient volume, to support staffing, care delivery improvements, and local sustainability.
Beyond shared saving contracts, the collaborative also centralizes comprehensive pre-visit planning and pharmacy consults that provide comprehensive medication review and recommendations. These workforce extenders add capacity for all member organizations.
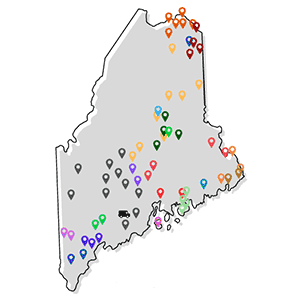
The participating hospitals are:
- Cary Medical Center
- Millinocket Regional Hospital
- Mount Desert Island Hospital
- Penobscot Valley Hospital
- St. Joseph Healthcare
The participating FQHCs are:
- Bucksport Regional Health Center
- Community Clinical Services, Inc.
- Eastport Health Care, Inc.
- Fish River Rural Health
- Greater Portland Health
- Harrington Family Health Center
- Health Access Network
- HealthReach Community Health Centers
- Hometown Health Center
- Islands Community Medical Services, Inc.
- Katahdin Valley Health Center
- Maine Mobile Health Program
- Nasson Health Care
- Pines Health Services
- Regional Medical Center at Lubec
- Sacopee Valley Health Center
- St. Croix Regional Family Health Center
Through one of its member organizations, CCPM was awarded a 2016-2019 Federal Office of Rural Health Policy (FORHP) Small Health Care Provider Quality Improvement grant. In 2025, CCPM secured more than $3.7 million in grant funding to support several of its initiatives, including cancer screening and prevention, virtual curbside consultation services, diabetes and cardiovascular disease prevention, and other primary care and quality improvement innovation strategies.
Services offered
CCPM uses a health information exchange (HIE) called HealthInfoNet to share patient information among the hospitals and FQHCs. This HIE allows the facilities to provide better-coordinated care to their patients and to collect population health data. In addition, the HIE provides real-time predictive analytics in order to predict (and work to prevent) readmissions.
CCPM also allows member organizations to share services in order to reduce costs and duplicated services. Rural organizations do not have to "reinvent the wheel" when they can borrow another organization's expertise or services.
CCPM is a forum for sharing best practices on how to help patients be as healthy as possible and how to help reduce unnecessary emergency department visits or hospitalizations. Rural member organizations report that monthly sharing with their peers reduces rural isolation and provides collegial support.
CCPM hosts a series of recurring meetings where members convene to discuss changes and innovations in patient care, quality, and data analytics. These include Quality & Clinical Integration, Care Management, and Medical Directors meetings.
In 2019, CCPM launched Pharmacy Consults as a benefit of ACO membership. Any patient of its 22 member organizations is eligible to receive this service. CCPM employs a Clinical Pharmacist to support this service line. Upon referral, the Clinical Pharmacist performs a comprehensive medication review and issues recommendations that include:
- Changes in the medication regimen
- Instructions for monitoring for specific desired (or undesired) outcomes
- Suggestions for management of potentially inappropriate medication use
In 2019, CCPM began onboarding and training medical assistants (MAs) to support its member organizations with pre-visit planning. CCPM's centralized MAs are specially trained to provide comprehensive pre-visit planning, reducing administrative burden and freeing up time for both the provider and MA. Over the lifetime of the service, CCPM has completed more than 105,000 pre-visit plans for its members. CCPM's pre-visit planning MAs now serve 10 of the 21 member organizations and are working to operationalize the service with additional organizations.
CCPM offers medication-assisted treatment (MAT) and care management consultation on a contracted basis to interested member organizations. In addition, CCPM offers a free online Continuing Medical Education (CME) Series as a benefit of ACO membership. Any employee of the 22 member organizations is eligible to access the library of AMA-accredited CME modules, many of which are tailored to an FQHC audience.
In 2024, CCPM partnered with a platform to offer virtual curbside specialty consults directly to its members' providers. All CCPM member organizations now have clinicians utilizing the service, with a 99% satisfaction rate. By the end of 2025, the program surpassed 5,000 consults and achieved estimated cost savings of over $1 million. CCPM also secured two grant awards to fully offset member costs for this service in 2026. CCPM continues to explore additional opportunities to engage with the platform.
Results
Over the course of several years, CCPM has implemented a complex LLC legal structure, compliance program, organization, and financial structure. CCPM also covers about 120,000 patients in Maine.
CCPM has earned shared savings for 9 consecutive years under the Medicare Shared Savings Program (MSSP). In addition, CCPM has implemented shared savings arrangements/contracts with different Medicare Advantage and other private health payers.
In 2024, CCPM generated over $18 million in savings under MSSP, resulting in about $7 million in shared savings for CCPM. CCPM is the only ACO in Maine, and one of a handful of ACOs nationwide, to have achieved shared savings for 9 consecutive years (2016-2024). To date, CCPM's work has saved Medicare $98.2 million.
The ACO presents at multiple state and regional committees and organizations focused on rural healthcare and population health, including the Maine Council on Aging and the Maine Public Health Association. CCPM staff provide annual presentations on their work at regional conferences, such as the New England Rural Health Association.
Challenges
While CCPM views its vast geography spread across the state as a strength, it recognizes that the distance poses some logistical barriers. To overcome these barriers, CCPM hosts the majority of its committee meetings virtually to reduce travel time for attendees, a practice that allowed it to continue operations during the COVID-19 pandemic.
CCPM also contends with the use of multiple electronic medical records (EMRs) across its 22 member organizations, which at times poses challenges in starting new initiatives.
Replication
Some member organizations had tried other ACO models but felt that they didn't "fit" into these work cultures. CCPM was a better fit because the member organizations shared similar values, like focusing on their communities' immediate needs.

CCPM also credits its long-standing success to the leanness of its organizational structure. All of CCPM's officers fulfill their role in a part-time capacity while also serving in a separate role at one of its member organizations.
Contact Information
Danielle Brown, Executive AdministratorCommunity Care Partnership of Maine
daniellebrown@ccpmaine.org
Topics
Accountable Care Organizations
· Federally Qualified Health Centers
· Healthcare quality
· Hospitals
· Primary care
States served
Maine
Date added
February 17, 2017
Suggested citation: Rural Health Information Hub, 2026 . Community Care Partnership of Maine Accountable Care Organization [online]. Rural Health Information Hub. Available at: https://www.ruralhealthinfo.org/project-examples/944 [Accessed 13 May 2026]
Please contact the models and innovations contact directly for the most complete and current information about this program. Summaries of models and innovations are provided by RHIhub for your convenience. The programs described are not endorsed by RHIhub or by the Federal Office of Rural Health Policy. Each rural community should consider whether a particular project or approach is a good match for their community’s needs and capacity. While it is sometimes possible to adapt program components to match your resources, keep in mind that changes to the program design may impact results.
