Win With Wellness
- Need: To reduce risk of obesity and chronic disease in rural northwest Illinois.
- Intervention: Win With Wellness (WWW) collaborated with community organizations and worksites to improve physical activity and eating behaviors and reduce weight among adults using a multi-component approach.
- Results: From 2015 to 2018, the two participating counties initiated 28 Take Off Pounds Sensibly (TOPS) groups with 367 participants. In the second round of funding, WWW recruited 183 participants for 9 TOPS groups and 8 community Heart-to-Heart sites.
Description
 Residents in northwest Illinois faced increased
risks of obesity and chronic disease due to unhealthy
behaviors and limited access to physical activity
opportunities and healthy foods.
Residents in northwest Illinois faced increased
risks of obesity and chronic disease due to unhealthy
behaviors and limited access to physical activity
opportunities and healthy foods.
In 2014, researchers at the University of Illinois College of Medicine Rockford compared county data to overall state data from the Illinois Behavioral Risk Factor Surveillance System and found that residents of Stephenson County and Carroll County showed higher rates of diabetes, heart disease, and current smoking than the state average. The premature age-adjusted mortality rate was markedly higher in both counties, especially Carroll.
In addition, these researchers found that a significant proportion of the population in both counties was overweight or obese. In Stephenson County, 73.5% of adults were obese or overweight in 2014; in Carroll County, the percentage was 72.6%.
Through a 2015-2018 Federal Office of Rural Health Policy (FORHP) Rural Health Care Services Outreach grant, the Win With Wellness (WWW) collaborative was initiated to reduce obesity and chronic disease risk for adults in Stephenson and Carroll counties using a multi-component, community-based approach to promote healthy eating and physical activity behaviors. Interventions supported with initial funding included:
- Take Off Pounds Sensibly (TOPS), a weight-loss support group for adults
- Heart-to-Heart (HH) health promotion sessions for worksites and community groups
- Media campaign, including billboards, social media, and radio interviews
In 2018, WWW received a 2018-2021 FORHP Rural Health Outreach grant and enhanced programming focused on reducing the burden of cardiovascular disease (CVD) in adults in Stephenson and Carroll counties by addressing modifiable risk factors.
Interventions focused on improving health behaviors to reduce CVD risk and assessing and addressing environmental barriers to engaging in physical activity and healthy eating behaviors. During the three-year project, WWW targeted a cohort of eligible adults aged 30-74 to engage in community or worksite-based interventions to address their personal CVD risk factors identified during enrollment screenings. By leveraging additional funding, WWW was also able to serve adults who did not meet eligibility criteria, including those over age 74. With the new funding and focus, the following interventions were added to the initial TOPS and HH groups:
- Text-4-Wellness, a texting program in which participants can receive information and motivational messages
- Step-4-Wellness, a physical activity monitor program in which participants can track their daily steps
- HH online sessions
- Referrals to primary care and the Illinois Tobacco Quitline
In addition, physical activity and nutrition environment assessments were conducted and information about existing resources were provided to residents, both in online format and through flyers posted in the community.
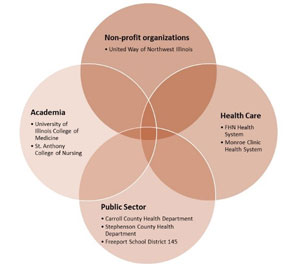
The 2018 WWW partnership included county health departments, clinics and healthcare systems, colleges of medicine and nursing, a United Way branch, and a school district. Medical and nursing students gained experience in community-based research, and WWW benefited from their volunteer work. During this partnership, three medical students helped with the WWW Facebook page and two nursing students helped with the environmental assessments.
WWW is not currently active.
Services offered
Participants received TOPS membership through the FORHP grant. TOPS is a weight-loss support group for adults that focuses on small changes participants can make to their diets and activity levels. Weekly group sessions held in community settings included private weigh-ins and professionally prepared, informational programs featuring up-to-date information on nutrition, exercise, and healthy lifestyles. The program provided positive reinforcement and motivation to adhere to food and exercise programs.
HH presentations are health education sessions led by health educators for worksites and community groups. These presentations emphasize small, practical changes that attendees can make to reduce CVD risk. In December 2019, online HH curriculum modules were launched.
Text-4-Wellness Text Messaging Program: Participants had the option of enrolling in this program. Enrolled participants received three text messages per week for 16 weeks and had the option to re-enroll to receive additional messages at the end of each 16-week period. Messages provided tips and motivation to encourage healthy eating and physical activity.
Step-4-Wellness (S4W) physical activity monitor program: Participants had the option of enrolling in this program. Enrolled participants received a physical activity tracker (if they needed one) and agreed to sync their daily physical activity with both the tracker's app and an online platform that allowed for activity tracking and the creation of physical activity challenges. Participants were placed in three-week "challenges" in which they received a daily step goal. After each three-week challenge, participants engaged in a one-week group challenge to reach larger step goals as a group.
Community-wide physical activity assessments were completed for four communities using the Town-Wide Assessment (TWA), Program and Policy Assessment (PPA), and Street Segment Assessment (SSA) components of the Rural Active Living Assessment (RALA). Physical activity maps were created for each town. Food environment assessments in the same communities using the Nutritional Environment Measures Survey in stores (NEMS-S) were initiated.
Results
Results from the 2015-2018 FORHP grant
WWW enrolled a total of 367 participants, 92% female and 8% male. Participants who completed one year of the program saw significant reductions in weight (a mean weight loss of 8.8 pounds), which translates to a 1.5-point average reduction in body mass index (BMI). In addition, 42% of participants lost 5% of their body weight or more.
Thirty-nine HH sessions were conducted, with 348 participants (79% female, 21% male): 72% of respondents reported planning to make one or more changes in physical activity, and 83% of respondents reported planning to make one or more changes in eating habits as a result of attending a Heart-to-Heart session.
Results from the 2018-2021 FORHP grant
Overall, 183 participants were recruited for the cohort study. Since this program was a continuation of the previous funding, participants from the 2015-2018 program were brought into the new program.
WWW had 9 TOPS groups and 11 HH sites. A total of 109 participants signed up for the optional Step-4-Wellness program and 86 participants signed up for the Text-4-Wellness program.
The Town-Wide Assessment (TWA) and Program and Policy Assessment (PPA) were completed for the rural communities of Freeport, Lena, Mount Carroll, and Savanna. The TWA assessed 18 town characteristics including topography, schools, and recreational amenities. The PPA assessed 11 town-level policy and program items that supported physical activity. These two assessments enabled the development of a comprehensive database of the amenities and policies that promoted or limited physical activity within each town. The information was used to create online community asset maps.
Challenges
Recruitment Challenges
Recruitment took more time and effort than anticipated, particularly due to the difficulty in engaging local worksites to participate. Moving from discussions about worksite wellness to actual implementation required more extensive planning and ongoing relationship-building than anticipated. Barriers included scheduling meetings with appropriate worksite contacts; conflicting work schedules among employees within a worksite, which created challenges in finding a time when a group could meet; busy schedules among worksite employees, which reduced their ability to participate in the group; and competition with other worksite wellness initiatives, such as those offered by health insurance companies.
Because of recruitment challenges, WWW pursued partnerships with community-based organizations, such as churches, and introduced the online version of HH to reduce participation barriers.
Implementation Challenges
-
Physical Activity Tracker Program (S4W): The
implementation of S4W introduced a number of challenges
including participants' lack of familiarity with
physical activity trackers, teaching participants how
to pair their trackers with their phones, participants'
lack of access to technology to sync their trackers,
and smart phone issues such as compatibility with
trackers and apps. This required additional staff time
to provide one-on-one support for the participants
until they were comfortable with the technology.
WWW also created a visual guide with screenshots to provide participants with simple instructions for syncing and troubleshooting. For participants who did not have a smart phone or other device for syncing, or for those with persistent challenges with syncing, paper tracking was offered to ensure no one would be excluded from the program. - Participant Tracking to Maintain the Cohort: Due to the complexity of the intervention and multiple components, participant tracking was complex and labor-intensive. For example, participants could join existing TOPS and HH groups at any time, so follow-up data collection did not necessarily occur at the same time for all participants. Additionally, while TOPS is a participant-led program, group leaders did not want to manage group activities and preferred WWW staff to fulfill that role. Participants could also engage in any one of the optional programs, which added another layer of tracking that was required.
- Participant engagement in HH-Online: WWW assessed the usefulness of implementing online HH modules. Early challenges identified include internet accessibility issues as well as resistance in older adults to familiarizing themselves and becoming comfortable with using the technology.
- Partner Engagement: Almost all the WWW partners were actively engaged in the network: They participated in monthly meetings in-person or by phone, provided input and resources in support of WWW, and participated in decision-making related to the WWW activities. The local school district was invited to the partnership at the start of the current grant period. However, due to staff turnover and internal challenges, they remained disengaged in WWW.
- COVID-19: COVID-19 provided unexpected challenges to the WWW program. Both TOPS and HH are in-person programs. Health educators came up with creative ways of staying in touch with program participants by using online conferencing platforms, online HH modules, and one-on-one health coaching phone calls.
Replication
A key factor to successful replication of community-based partnerships and health programs is to involve people/organizations from multiple sectors during the planning and development stages. Incorporating individuals from sectors not directly related to health can bring a new perspective to the group.
WWW held annual meetings with all participants to provide them feedback on the data and to celebrate their successes. It was also an opportunity to hear participant perspectives on the current program as well as get their ideas for future efforts.
Contact Information
Manorama M. Khare, PhD, Director of the Division of Health Research and EvaluationUniversity of Illinois College of Medicine at Rockford
815.395.5762
mkhare1@uic.edu
Topics
Community engagement and volunteerism
· Food security and nutrition
· Obesity and weight control
· Physical activity
· Wellness, health promotion, and disease prevention
States served
Illinois
Date added
February 27, 2017
Suggested citation: Rural Health Information Hub, 2025 . Win With Wellness [online]. Rural Health Information Hub. Available at: https://www.ruralhealthinfo.org/project-examples/946 [Accessed 21 May 2026]
Please contact the models and innovations contact directly for the most complete and current information about this program. Summaries of models and innovations are provided by RHIhub for your convenience. The programs described are not endorsed by RHIhub or by the Federal Office of Rural Health Policy. Each rural community should consider whether a particular project or approach is a good match for their community’s needs and capacity. While it is sometimes possible to adapt program components to match your resources, keep in mind that changes to the program design may impact results.
