The Pacific Care Model: Charting the Course for Non-communicable Disease Prevention and Management
- Need: The U.S. Associated Pacific Islands (USAPI) needed an efficient, effective, integrated method to improve primary care services that addressed the increased rates of non-communicable disease (NCD), the regional-specific phrase designating chronic disease.
- Intervention: Through specialized training, multidisciplinary teams from five of the region's health systems implemented the Chronic Care Model (CCM), an approach that targets healthcare system improvements, uses information technology, incorporates evidence-based disease management, and includes self-management support strengthened by community resources.
- Results: Aimed at diabetes management, teams developed a regional, culturally-relevant Non-Communicable Disease Collaborative Initiative that addresses chronic disease management challenges and strengthens healthcare quality and outcomes.
Evidence-level
Effective (About evidence-level criteria)Description
According to a 2023 Health and Human Services evaluation website post, the populations of the U.S. Territories totaled 474,000: the flag territories of the American Samoa and Guam with populations of 55,000 and 169,000, respectively; the Commonwealth of the Northern Mariana Islands 58,000, the freely associated jurisdictions of the Federated States of Micronesia with 115,000; and the Republic of the Marshall Islands 59,000, and the Republic of Palau 18,000.
The region spans across twice the geographic size of the continental U.S. and islands collectively cross not only five time zones, but also the International Date Line.
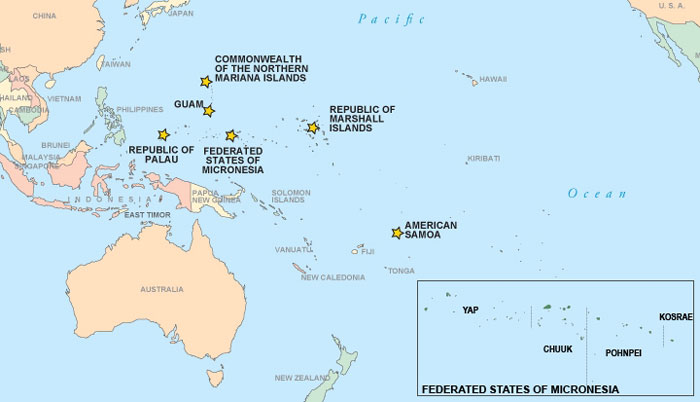
Included are the flag territories of American Samoa and Guam; the Commonwealth of the Northern Mariana Islands; the freely associated jurisdictions of the Federated States of Micronesia (FSM); the Republic of Palau; and the Republic of the Marshall Islands (RMI).
According to the International Diabetes Federation, the prevalence of diabetes within the USAPI is among the highest in the world. In 2008, prevalence estimates ranged from 15% to nearly 27%, compared to that in the U.S. of slightly above 8%.
In 2009, a public health organization created a specific Pacific Chronic Disease Council (PCDC) to address escalating healthcare needs caused by non-communicable chronic diseases (NCD), the regional-specific phrase designating chronic diseases. By 2010, a state of emergency was declared by the Pacific Island Health Officers due to epidemic rates of NCD, stepping up the region's work to manage NCD morbidity and mortality. Also in response to NCD rates, the PCDC created the Pacific NCD Collaborative, a participatory process that promotes co-learning; facilitates collaborative partnerships; and builds skills and strengths of local leadership responsible for health. In addition to implementing the NCD Collaborative, the PCDC also collaborated with CDC and international partners to establish and refine the Pacific Standards for TB and Diabetes Management.
The PCDC initiated the collaborative as a pilot project based on a regional needs assessment that revealed fragmented services, inadequate continuity of care, and limited data for change decision-making. This collaborative effort included public health trainers working with teams formed by members from Community Health Centers (CHCs) and hospital-based systems in the four states of FSM (Chuuk, Kosrae, Pohnpei, and Yap) and also including Majuro, RMI.
Using the chronic care model as a strategy for quality improvement, the project targeted diabetes preventive care. It included plans for future scale-up and program sustainability.
An implementation evaluation tool, the Consolidated Framework for Implementation Research (CFIR), helped identify factors influencing complex healthcare interventions. The Chronic Disease Electronic Management System (CDEMS), a public-domain data management software application with technology support provided by West Virginia University, was adopted by each site to track outcome measures. Three-day learning sessions included The Deming Institute's continuous quality improvement process, followed by field implementation of four to six months intervals to monitor needed health system change. In addition to integrating the "plan, do, study, act" process, sessions also included team training, progress reviews, problem solving, and creating diffusion plans. Local health professional trainers familiar with Health and Human Services agency's disparities collaboratives resources provided assistance.
Two year's work culminated in 2015 with the creation of the Pacific Care Model (PCM). The model is rooted in the local transportation heritage, the traditional outrigger canoe and star navigation. Most recently, the work's logic model has been established.
The work continued with formal meetings where insights, gains, and improvements are shared, the last gathering in 2019.

This model used the canoe to represent effective communication between patients, families, and the healthcare teams; and the stars to represent six PCM elements. Building on this central theme, collaboration is required to reach an intended destination by canoe, and to reach a destination of improved health services and outcomes.

Partial funding for pilot activities was provided by the Centers for Disease Control and Prevention, and the U.S. Department of the Interior, Office of Insular Affairs. Additional support was provided by the Pacific Islands Health Officers Association (PIHOA), Pacific Basin Medical Association, West Virginia University' Office of Health Services Research,and the National Center for Chronic Disease Prevention and Health Promotion, Division of Diabetes Translation.
Services offered
Services offered:
- Diabetes clinical performance measures, such as yearly foot exams, dental exams, blood pressure control monitoring
- "One-stop shop" care and other clinic redesigns
- Increased access to care, and increased quality of care
- Increased diabetes self-management support
- Nutrition counseling
- Universal gestational diabetes screening
Results
Clinical results from the initial 16-month pilot include:
- Median drop of A1C by 1.4 percentage points at three sites.
- Increased diabetes self-management goal-setting at all sites, a key element of diabetes care to decrease diabetes-related complications and improve quality of life
- Improved clinical performance measures at some sites, such as blood pressure control and screening exams
- CDEMS adaptation for the Pacific region's unique screening needs for diabetic comorbid issues, for example betel nut use in addition to tobacco use, and tuberculosis
- Educational materials/resources updates including culturally-relevant information for diabetics and their families
In January 2018, a learning session was held. Additional accomplishments and innovations noted by the teams are:
- Tracking of patients lost to follow-up
- Update of clinical indicators by endocrinology specialists
- Progress in one-stop clinics and other redesigns
In 2019, 11 multidisciplinary teams, representing the region's USAPI health care systems, participated in the Pacific NCD Collaborative. Teams reporting at the bi-annual Collaborative Learning Sessions demonstrated continued diabetes registry database improvements that allows individual patient and physician tracking of preventive care practices, benchmarking, and population management across the participating healthcare teams. These registries expanded to also include individuals previously lost to follow-up as well as the newly diagnosed.
Teams continued to use Plan-Do-Study-Act cycles for the upcoming year and aim for continued improvement in aggregate A1C average, diabetic foot screening, depression screening, self-care goal documentation and blood pressure control.
Teams also demonstrated improvements from using evidence-based preventive practices. Several examples were:
- A median drop of A1C of almost 1 percent in Pohnpei, and FSM.
- Improvements in documentation of:
- Blood pressure control (<140/90) (Palau])
- Depression screening (Kosrae, FSM, Palau)
- Foot exams (Ebeye, Majuro, RMI, Palau)
- Self-care goal (Majuro, Pohnpei, Yap, FSM, Palau)
- Dental exams (Palau)
An increased number of partnerships continue to share the care model by outreach and expansion. For example, in partnership with the Health Resources and Services Administration (HRSA) National Hansen's Disease Program, a train-the-trainer model addressed lower extremity amputation prevention skills for 12 healthcare professionals working in the region.
Another example is the development of culturally relevant diabetes self-management education (DSME) resources, such as the Navigating the Course of Diabetes Self-Care Guidebook, which increases access to DSME and encourages individuals living with diabetes and their families to work with their healthcare teams to prevent complications and promote health.
As of 2020, regional healthcare system involvement increased from eleven to twelve multidisciplinary teams. Diabetes patient registries continue to expand to include those lost to follow-up or previously undiagnosed. Established evidence-based practices that prevent or delay diabetes-related complications and promote health have continued in their use.
Due to the COVID-19 Public Health Emergence (PHE), mid-year 2020 virtual sessions have increased local NCD team member participation. Feedback demonstrated that virtual venues have strengthened collaboration.
For more detailed program results:
Hawley, N.L., Suss, R., Cash, H.L., Aitaota, N., Ayers, B., McElfish, P.. (2019). Diabetes Prevention and Care Programs in the US-Affiliated Pacific Islands: Challenges, Innovation, and Recommendations for Effective Scale-Up. Current Diabetes Reports, 19 (5) 24.
Hosey, G. M., Rengiil, A., Maddison, R., Agapito, A. U., Lippwe, K., Wally, O. D.,... Satterfield, D. (2016). U.S. Associated Pacific Islands Health Care Teams Chart a Course for Improved Health Systems: Implementation and Evaluation of a Non-communicable Disease Collaborative Model. Journal of Health Care for the Poor and Underserved, 27(4A), 19-38.
Hosey, G., Ichiho, H., Satterfield, D., Dankwa-Mullan, I., Kuartei, S., Rhee, K., Belyeu-Camacho, T., deBrum, I., Demei, Y., Lippwe, K., Luces, P. S., & Roby, F. (2011). Chronic disease surveillance systems within the US Associated Pacific Island jurisdictions. Preventing chronic disease, 8(4), A86.
Hosey, G., Aitaoto, N., Satterfield, D., Kelly, J., Apaisam, C. J., Belyeu-Camacho, T., deBrum, I., Luces, P. S., Rengiil, A., & Turituri, P. (2009). The local community attitude towards — and science of — type 2 diabetes prevention in the US Associated Pacific Islands. Preventing chronic disease, 6(3), A104.
Challenges
- Extended time for multiple summit meetings and training sessions
- Skill-building and training to assure quality of clinical data entry, organization, analysis and reporting CDEMS
- Challenges in sustaining consistent regional collaborative team learning sessions
- New member orientation
- Clarity around team member roles and responsibilities
- Development and expansion of standard operating procedures within healthcare systems
Replication
Lessons learned using the CFIR organizing framework for scale up and sustainability:
- Healthcare transformation needs high level administrative support and endorsement
- Reaching consensus for best practices and evidence-based care standards requires facilitation by experts familiar with NCD prevention and management in low-resource settings
- Maximizing the reach of the NCD Collaborative requires alignment and support of international, federal, regional, as well as community partners
- Low resource healthcare environments benefit from the availability of public domain software like CDEMS that allows team members to establish diabetes registries, input data, and generate clinical reports to monitor trends (individual and aggregate), guide management decisions, and develop change strategies
- Creating the PCM to fold in the traditional Pacific Island cultural practices and local knowledge is key for program sustainability and diffusion
Low-resource healthcare systems have unique needs. The collaborative's initial efforts accounted for scale-up and the replication needs outside the original five pilot areas. Essential for replication:
- Garner and maintain senior health officials support
- Engage experienced public health experts for training needs
- Reach quick consensus on policies and guidelines
- Ensure team membership consists of a physician, nurse, data staff, and senior administrator

Topics
Chronic disease management
· Culture
· Diabetes
· Wellness, health promotion, and disease prevention
States served
American Samoa, Commonwealth of the Northern Mariana Islands, Federated States of Micronesia, Guam, Republic of Palau, Republic of the Marshall Islands
Date added
May 1, 2017
Suggested citation: Rural Health Information Hub, 2025 . The Pacific Care Model: Charting the Course for Non-communicable Disease Prevention and Management [online]. Rural Health Information Hub. Available at: https://www.ruralhealthinfo.org/project-examples/952 [Accessed 5 June 2026]
Please contact the models and innovations contact directly for the most complete and current information about this program. Summaries of models and innovations are provided by RHIhub for your convenience. The programs described are not endorsed by RHIhub or by the Federal Office of Rural Health Policy. Each rural community should consider whether a particular project or approach is a good match for their community’s needs and capacity. While it is sometimes possible to adapt program components to match your resources, keep in mind that changes to the program design may impact results.
