Health Extension Regional Offices (HEROs)
- Need: People in rural New Mexico often found it difficult to find and utilize needed resources from the University of New Mexico Health Sciences Center (UNMHSC).
- Intervention: UNMHSC created Health Extension Regional Offices (HEROs), in which HERO agents live in the communities they serve, help identify health and social needs, and link them with UNMHSC and other university resources.
- Results: In their regions, HERO agents' activities have been wide-ranging, including recruiting physicians, mobilizing research funds to address local priorities, working on economic development, training laypeople in Mental Health First Aid, and helping local institutions access UNMHSC resources.
Evidence-level
Promising (About evidence-level criteria)Description
New Mexico has the third highest rate of poverty among the 50 states, and has been ranked at or near the bottom for child well-being, education, and family and community health. It also ranks among the top 10 states for number of uninsured people, and nearly 50% of its population lives in a Health Professional Shortage Area. Given these challenges, getting healthcare information and services to residents, especially those in remote and rural areas, is essential.

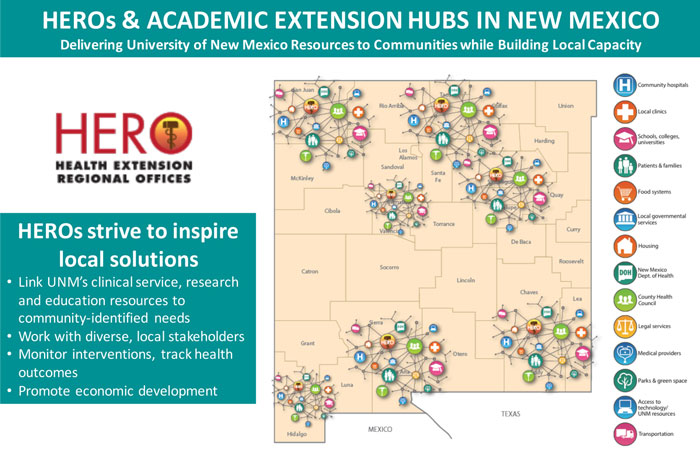
Toward this goal, the University of New Mexico Health Sciences Center (UNMHSC) sought better ways to engage with residents across the state. A survey of rural New Mexicans had criticized UNMHSC for its lack of long-term commitment and attention to their needs, and compared UNMHSC's outreach unfavorably to that of New Mexico State University's agricultural cooperative extension work in their communities. Inspired by the cooperative extension model, which links the expertise of the agricultural college to the work and lives of farm families and communities, UNMHSC developed Health Extension Regional Offices (HEROs). HEROs recruits and locates HERO agents in different regions across the state.

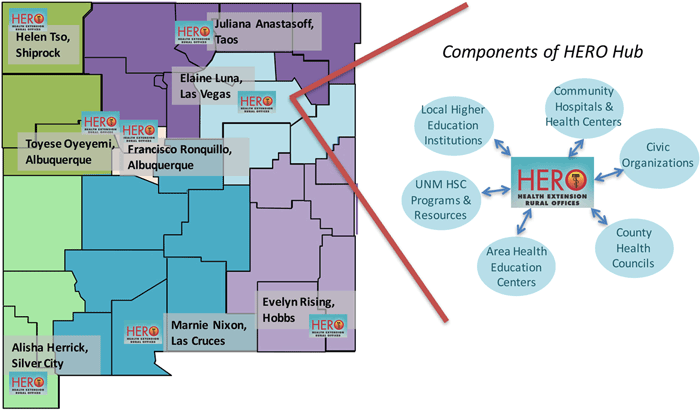
HERO agents work much like Agricultural Extension agents, linking communities with available UNM resources while, at the same time, informing the university about community needs. The agents live in the communities they serve, working to improve local health services and systems. As part of this effort, they work with different sectors and stakeholders in their communities, including health, education, business, agriculture, government and non-profits. They help recruit the appropriate health workforce, mobilize researchers to bring grants to the community and address local health needs, and create local pipelines into health careers. HEROs also meet regularly with one another, sharing ideas on what is working in their efforts to connect with people in their communities.
The overall goal of HEROs is to strengthen community capacity to address local health and social needs. The UNMHSC Office for Community Health (OCH) coordinates the HEROs program and serves as its central point of contact.
The program works with strong, community-based allies such as the Center for Health Innovation (CHI), the state's Area Health Education Centers (AHECs), and community colleges and universities, including the New Mexico State University Cooperative Extension Service.
An example of this collaboration involves the Health Insurance Exchange. UNMHSC was contracted to educate young adults on the value of enrolling in Medicaid or the Exchange. The vehicle for information dissemination included HERO agents and Cooperative Extension agents, the latter being much more knowledgeable of the state's rural counties. In addition, local extension offices have provided resources such as dietitians and nutritionists in areas where obesity and diabetes rates were high, after HERO agents identified the need for them.
Funding for HEROs comes from multiple sources—university, county, endowment, contracts, and federal and other grants. Initial grant funding for HEROs came from the AHRQ IMPaCT (Infrastructure for Maintaining Primary Care Transformation) grant, which supported HERO agents helping small primary care practices become patient-centered medical homes.
AHRQ continued its support through HERO TRalLS (Translating Research Into Localities), which funded the training of primary care practitioners on safe, effective prescribing of opioids. In addition, support from the Commonwealth Fund helped launch the Health Extension Toolkit and funded a conference. UNMHSC also is partnering with the University of Colorado in a $15 million five-year grant from AHRQ called EvidenceNOW that deploys the health extension practice facilitation to help practices adopt evidence-based guidelines in cardiovascular disease prevention.
HERO agents are paid, full-time employees. Their payment source is a mix of university, endowment, and county funds, and research, education and service contracts and grants.
Services offered
- Healthcare workforce development
- Pipeline development to encourage local youth to pursue healthcare degrees
- Telehealth services for training, service, and communications
- Research on community priorities
- Community-based health professions education, clinical service, and program evaluation
- Technical assistance on capacity building, recruitment and retention of workforce, grant writing and evaluation, and health-related community planning
Results
Each HERO agent works independently to focus on priority health needs defined by his or her region. For that reason, outcomes relate to local more than statewide needs. The success of HERO agents depends on their partnering with local stakeholders and mobilizing local and university resources. Therefore, outcomes are a result of HERO agents partnering with local stakeholders. These outcomes have included:
Workforce:
Helped bring 5 new family physicians to rural Lea County and UNM Family Medicine resident rotations every month to frontier Guadalupe County.
Behavioral health:
HERO agents brought Mental Health First Aid to the state. Each agent has become a regional trainer for local laypersons, and thousands have been trained.
Access to care:
A HERO agent wrote the grant for a rural county to be designated as an FQHC site.
Social Determinants of Health:
Each HERO agent has convened stakeholders from different local community sectors to contribute to reducing adverse social determinants. This has included increasing school graduation rates, increased parent involvement in schools, increased rural and inner city enrollment in Medicaid, and reduction in use of opioids in rural primary care practices.
Publications:
Kaufman, A., Dickinson, P.W., Fagnan, L.J. & et al. (2019). The Role of Health Extension in Practice Transformation and Community Health Improvement: Lessons From 5 Case Studies. Annals of Family Medicine, 17 (Suppl 1), S67-S72.
HEROs in Rural Health: Q&A with Art Kaufman. Rural Monitor, 2018.
Kaufman, A., Boren, J., Koukel, S. & et al. (2017). Agriculture and Health Sectors Collaborate in Addressing Population Health. Annals of Family Medicine, 15(5), 475-480.
HERO: New Mexico's Health Extension as a Model for Primary Care Transformation. Content last reviewed April 2015. Agency for Healthcare Research and Quality, Rockville, MD.
TEDxABQ (TED Talk): Art Kaufman - Health Extension: Learning from Farmers How to Improve Community Health. (Published on YouTube, November 3, 2011).
Challenges
In the beginning, some organizations in the state, such as AHECs and Agricultural Cooperative Extension, feared that HEROs would encroach on their turf and their funding. But HEROs has overcome that resistance through collaboration. It now shares complementary strengths with Cooperative Extension and has incorporated AHEC in its office — HERO agents and AHEC coordinators now each wear both hats, extending the range of each program. A remaining challenge is encouraging UNM to listen more to the community via the HERO agents and to respond to their needs more than its own.
Replication
UNMHSC has taken part in creating a Health Extension Toolkit, which shares information from states that have or are implementing health extension. The toolkit explains how health extension works and how it can be used in public health and primary care settings. Its audience includes states, academic health centers, professional societies, and Tribal Nations.
Topics
Access
· Health disparities
· Health workforce
· Physicians
· Wellness, health promotion, and disease prevention
States served
New Mexico
Date added
October 12, 2017
Suggested citation: Rural Health Information Hub, 2024 . Health Extension Regional Offices (HEROs) [online]. Rural Health Information Hub. Available at: https://www.ruralhealthinfo.org/project-examples/981 [Accessed 6 June 2026]
Please contact the models and innovations contact directly for the most complete and current information about this program. Summaries of models and innovations are provided by RHIhub for your convenience. The programs described are not endorsed by RHIhub or by the Federal Office of Rural Health Policy. Each rural community should consider whether a particular project or approach is a good match for their community’s needs and capacity. While it is sometimes possible to adapt program components to match your resources, keep in mind that changes to the program design may impact results.