Jul 15, 2020
Advance Care Planning: New Realities in Times of COVID-19
 Leaving
nothing in its path untouched, the COVID-19 public health
emergency has impacted all aspects of health; of
well-being; and, of course, the delivery of rural
healthcare. Many rural experts believe that the epidemic
will help advance needed changes that otherwise might
have taken years to study, like changes being
brought about by current
telehealth waivers.
Leaving
nothing in its path untouched, the COVID-19 public health
emergency has impacted all aspects of health; of
well-being; and, of course, the delivery of rural
healthcare. Many rural experts believe that the epidemic
will help advance needed changes that otherwise might
have taken years to study, like changes being
brought about by current
telehealth waivers.
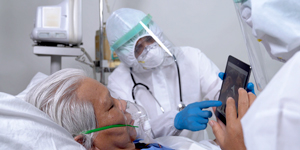
Other experts have focused on changes in patient care: the isolation of patients because of no-visitation policies and clinicians challenged with communication difficulties around this incompletely understood new disease.
And for patients who were stable one hour previous but now need intensive care interventions? For many of those patients and their families, it would have been key to have prior advance care planning (ACP): the process of "making decisions about the healthcare you would want to receive if you're facing a medical crisis," according to the National Hospice and Palliative Care Organization.
Clinicians' ACP Experiences in Times of COVID-19
For rural patients who require transfer to a distant urban center providing critical care, Dr. Lewis Satterwhite, a pulmonologist and critical care physician at the University of Kansas Medical Center, mentioned in an early April COVID-19 video presentation (no longer available online) for rural clinical research networks that it was important to try to have conversations about goals of care.
"One of the things I always worry about with the longer transfers [with regard to travel times from rural areas] are the risks of making that trip," Satterwhite said, pointing out that goals of care discussions are especially important knowing that aggressive care for COVID-19 might result in living with a less-than-desired outcome. "There is a need to be very upfront and honest about the risks."
Other frontline clinicians shared how the novel coronavirus has made the need for ACP very clear and gave examples of how ACP conversations are happening in times of physical distancing.

Dr. Aline Hansen-Guzman is a family physician in a Federally Qualified Health Center in Ft. Morgan, Colorado. With a clinical focus on obstetrics and pediatrics, she said that much of her current energy and activities are geared to isolation issues associated with the COVID-19-positive mothers and their newborns, in addition to the care of rural children. In situations where ACP is more urgent due to COVID-19, one of the early challenges was understanding COVID-19's clinical course in order to apply that knowledge for counseling patients and families.
"Especially early on, not knowing just what to expect about how the infection was going to act, not knowing how severe some of these cases were going to be, made a discussion difficult," she said. Additionally, she said being limited to a phone-only discussion — no video telehealth option available — provided another challenge because body language, which provides important clues for these sensitive discussions, is often more indicative of what's being understood than a verbal response.
Hansen-Guzman said other challenges with ACP discussions are linked with health literacy, primary language differences, and cultural expectations.
"Often our patients don't think of it [ACP] as necessarily an option or they come in with a more paternalistic sense of what medicine should be," she said. "They tell me, 'You just tell me what to do' or 'Whatever you think is best.' That has definitely been a big challenge for me when trying to have those discussions."
Hansen-Guzman's colleague Dr. Tamara Oser, also a family medicine physician and director of Colorado's High Plains Research Network, cares for Ft. Morgan patients of all ages. She echoed Hansen-Guzman's comments about the limitations of a phone conversation as compared to in-person discussions for ACP.

"I don't have a video setup, so my current visits are done over the phone," Oser said. "That means I don't have any visual clues when I'm interacting with patients with language and cultural differences — visual clues that are really important for advance planning discussions. We know these conversations are critical, especially in light of COVID, when we want to have an opportunity for people to share what their wishes would be. In my previous practice, I did a lot of Medicare wellness visits that automatically included advance care planning discussions. Now, there is so much less time since most of the available minutes are spent just trying to determine what medical problems are happening and what's going on in that respect."

Dr. William Vandivier, a pulmonologist and critical care physician at the University of Colorado – Anschutz Medical Campus, shared another element related to ACP: no visitation means family members are unable to take in the whole picture of a critically ill loved one — a gap he sees as not bridged by current video technology.
"I find that time talking with family members, developing a relationship with them, having them be present in the ICU, seeing how their loved one is doing and seeing the progression of their loved one's illness over time — all of these things help immensely when families are making decisions. If they've been able to spend the time at the bedside, I find that there's less of a difference between what I'm seeing and what they see. Now, that's not possible. Intermittent video interaction with limited screen views does not replace that physical presence at the bedside. I think that absence is making it much more difficult for families to make decisions."
When Video Technology Helps
In Lakin, Kansas, family physician Dr. Drew Miller is Chief Medical Officer at Kearny County Hospital. He and his colleagues care for patients in the clinic, their Critical Access Hospital, and long-term care setting. Initially, he said COVID-19 "turned our whole hospital upside down." However, with seven physicians and four physician assistants, they quickly organized for safety and sustainability. He shared that COVID-19 certainly made obvious the value of ACP to both clinicians and families, and their practice has depended on technology in addressing ACP.
"We always tried to have conversations with patients admitted to the hospital," Miller said. "But with COVID, what's changed is that we had to become very intentional about having those conversations."
He shared that early experiences showed just how brief the interval could be between admission at their Critical Access Hospital, followed by rapid deterioration and need for urgent transfer, where there were still unavoidable cases of death at an accepting facility. He said this brevity emphasized the importance of providing a way that patients and their families could engage with each other immediately after admission, an engagement that further promoted ACP discussions.

"This need for engagement impacted our workflow and now, with all our COVID patients, we have a chart order to video-call twice daily with family on an ongoing basis," Miller said. "We are also making more phone calls to families. We're finding out in follow-up clinic appointments just how much those efforts mean to our patients. I've noticed that even in non-COVID patients, our group is increasing their communication with family. Yes, it slows you down a little bit, but that effort to regularly communicate with family while their family member is in the hospital is really meaningful. I think it's just becoming part of our routine."
Miller said that the increased communication is often leading to an improved discharge process and he feels that COVID-19 has certainly highlighted the importance of patients having more prior knowledge of discussions that will arise during serious illness.
Talking ACP with Rural Patients in the Critical Care Unit
Vandivier, the Colorado physician, said that for the most part he doesn't perceive a rural-urban difference in an ICU ACP discussion, with one possible exception.
"Functional status," Vandivier said. "With the conversations I have in the ICU, everyone is usually interested in quality of life and their functional status. But I would also say that I've noticed that people from rural areas maybe stress the importance of function a little bit more because — and I'm guessing here — of their limited resources and rural culture itself that make it really important to function at a level that will allow independence."
Looking at the Future: Rural Options for Putting the "Advance" in Advance Care Planning
Older. Sicker. Poorer. Less access to medical care and often less access to educational opportunities. These are well-known descriptors used repeatedly for rural populations. So how can rural clinicians and healthcare organizations facing these common demographic challenges make sure their patients have access to ACP? These clinicians have been thinking about solutions. Hansen-Guzman envisions ideas like videos with information offered at the appropriate literacy level and using a respectful approach for language- and group-specific attitudes around health. Miller, too, expressed the need for informational videos.
"I'm thinking a video that says, 'Hey, this is what advanced care planning is. This is what you need to be thinking about, this is what to expect during the hospital stay, here are some great questions to ask your doctor during the hospital course,' Miller said. "Patients don't know what questions to ask. Eventually, the patient, the patient's family, and the doctors figure it out as we go along. But understanding of ACP by patients and family members right from the beginning is really important."
PREPARE™: ACP Videos for the General Population
One program offering informational videos meeting the needs outlined by Hansen-Guzman and Miller is PREPARE™ for Your Care, a program created by a coalition led by the University of California. Those associated with the program note that this informational approach is geared to patients and families rather than healthcare providers and organizations. It pairs a video with 5 steps core to ACP planning: 1) choosing a medical decision-maker: a surrogate to represent the person unable to speak for themselves, 2) deciding what matters most in life, 3) choosing flexibility for the surrogate decision-maker, 4) sharing personal wishes with others, and 5) asking doctors the right questions. Completion of an advance directive, also known as a living will, might also be accomplished.
In addition to ideas directly from clinicians, experts
and advocates have several additional suggestions: allow
other healthcare professionals to provide the information
and change healthcare policy in order to accomplish that.
The Department of Veterans Affairs (VA) Office of Rural Health (ORH) also supports an evidence-based rural promising practice using social workers, nurses, psychologists, or chaplains in a group setting and offers this ACP program by telehealth technology, noting that "health care providers often cannot and do not address ACP and advance directives during traditional medical appointments because of time constraints and lack of ACP expertise." [issue brief no longer available online]
In a recent statement that advocates said could also benefit rural populations, the Coalition to Transform Advanced Care suggested several policy changes (no longer available online) to expand the ACP reimbursement policy that includes only nurse practitioners, physician assistants, and physicians to also include social workers and nurses who can also efficiently and effectively facilitate the steps of ACP.
In addition to expanding the field of healthcare professionals assisting with ACP, the academic literature supporting the effectiveness of non-healthcare professionals offering ACP education to the general population is growing. A very recent journal article describes the success of a quality improvement project completed by academic nursing professionals in South Dakota who led a coalition that included 20 different professions and used the evidence-based ACP program Respecting Choices®.
COVID-19's Impact on ACP Legalities
Though often completed as part of formal estate planning, most states require only witnesses and a notary public — not an attorney or a healthcare provider — to complete legal documents required for ACP. Here again, physical distancing associated with COVID-19 impacts completion of these forms. Advocates and experts from across the country are talking about capturing state policymakers' attention in order to enact immediate changes needed to address a variety of legal requirements specific to ACP.
Nikole Nelson, executive director of Alaska's Legal Services Corporation's Anchorage and statewide office, shared in a recent webinar hosted by the National Center for Medical Legal Partnership that, although Alaska's legal system has much built into it to accommodate challenges of geographic distancing in a state that has a larger geographic footprint than California, Montana, and Texas combined, COVID-19 has still impacted medical-legal work.
"We are currently getting lots of questions about decision-making documents, advance directives, and wills," she said to the webinar viewers. "There is a high need for that at this point. Our legislature passed a law that allowed for video-notarizing. We're able to take advantage of that if people have the capacity and videoconferencing with the two witnesses and a notary in order to make a valid will. We're also giving out information about what to do if you have a handwritten will in case you to need to make that happen, [and also if you] don't have the capacity to bring in the normal requirements that you'd have for the formality relating to executing the will."
COVID-19 Global Impact: Are More People Thinking about ACP?
Experts and advocates have long proposed that ACP is important, irrespective of age or health. Dr. Rebecca Sudore, a northern California geriatrician and palliative care physician, is one of the PREPARE™ for Your Care collaborators. In a recent webinar presentation, she shared that there has been a 5-fold spike in access of program information, now reaching 200,000 unique users in over 115 countries. Though it's difficult to pinpoint an exact cause of the spike, it's likely that it's a result of the pandemic and comes from the general population's new desire to understand how they can take control of their future healthcare if they are unable to speak for themselves — conversations that experts and advocates hope are happening now between friends and between family members.
Sudore told the webinar audience that the topic of ACP has taken on new relevance even within her own family. Where previously her work in advance care planning had been understood by her family because of the medical decision-making needs of their mother, it didn't seem a relevant topic that actually applied to them. Sudore said COVID-19 seems to have changed her family's attitude.
"I have had conversations with my siblings that I never thought that I would have," Sudore said. "Though they know about the work that I'm doing and 'yeah, that was for our mom,' it wasn't for them. But now, it's for them."
Additional Resources
- Centers for Disease Control and Prevention
People Who Are at Increased Risk for Severe Illness - Medicare Learning Network
Advance Care Planning - Center for Advancement of Palliative Care
Advance Care Planning in COVID-19: Remote Notarization - The Conversation Project
Being Prepared in the Time of COVID-19 - Respecting Choices® Person-Centered
Care
Help with Breathing Decision Aid
Resources for Having Proactive Planning Conversations in the Context of COVID-19

