Nov 29, 2023
Nursing Students Bring Free Care to Rural Virginia with Student-Run Mobile Health Clinic
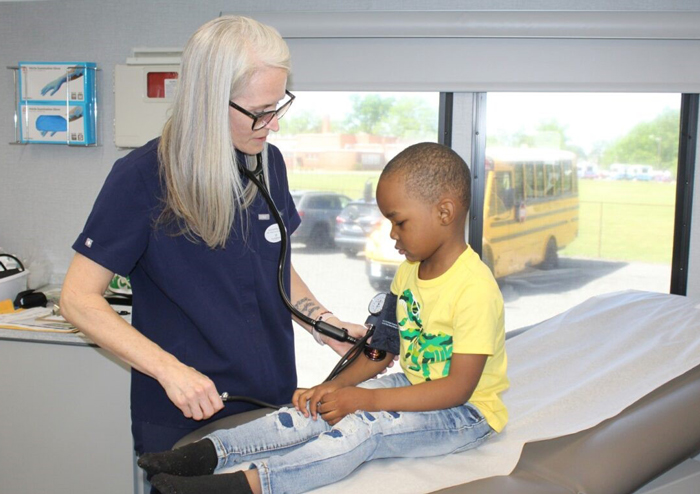
On the first day that the university's mobile health clinic hit the road, Jeffrey "Fritz" Bauman didn't know what to expect.
Bauman, a student in Old Dominion University's (ODU) family nurse practitioner (FNP) program, had never lived in a rural community before, much less worked as a provider in one. But he liked to volunteer. So when he saw an email asking for nurse practitioner students to staff a new student-run mobile health clinic serving rural southeastern Virginia, he signed up right away.
The first day the clinic opened its doors, Bauman and his fellow students only saw two patients. But over the following months, that number grew dramatically. At one event three months later, 74 patients were seen by students and faculty mentors over the course of five hours — with 50 more patients having to be turned away.
"We really had to build the community's trust and let them know what we were about and what we offered," Bauman said. "It's been monumental since then."
The free mobile clinic, which began seeing patients in April, was created with two goals in mind: to bridge gaps in care in the region's rural communities, while simultaneously providing ODU nursing students with clinical placement opportunities. By staffing the clinic with students, from undergraduates up to the doctoral level, the program gives future healthcare professionals hands-on experience in rural care.
"Our hope is that we grow a passion in our nursing students for providing this type of care in rural underserved communities," said Tammy Speerhas, DNP, FNP-C, CEN, who serves as Director of ODU Community Care. "We want to have long-term longitudinal impact, not just a short-term impact."
'A Tiger by the Tail'
In Franklin, Virginia — a city of about 8,000 people in the southeastern part of the state — the need to prioritize healthcare was clear to City Manager Amanda Jarratt. Franklin and its surrounding communities have few primary care physicians, with only two working pediatricians in the region and virtually no specialist providers: Recently, Jarratt recalls, she tried to make an appointment for herself at the local hospital and was met with a six-month wait. In Franklin, where Jarratt describes poverty as a "tremendous issue," these challenges are amplified for people who are uninsured, can't afford regular check-ups, or are unable to travel out of their communities for care.
"The healthier your community is, the healthier your workforce is, and the more productive your citizens are," Jarratt said. "You can't take care of yourself and your family when you're not well. So healthcare is a massive priority, but the importance of it isn't always understood at the community level."
At ODU, Carolyn Rutledge, PhD, FNP-BC, FAAN, Executive Director of Faculty Development, Innovation, and Research and Co-Director of the Center for Telehealth Innovation, Education and Research (C-TIER) in the School of Nursing, knew she wanted to launch a new kind of student-staffed mobile health clinic, ideally one that wouldn't have to travel long distances from the university's campus in Norfolk. She didn't have to look far to find a need in Franklin and neighboring Southampton County, both located within an hour of campus.
"I started exploring the area and realized it was a healthcare desert in a sense," Rutledge said. "Providers would come in, but would not stay. And I knew nurse practitioners tended to stay in these areas for much longer."
A mobile clinic would also bring new hands-on opportunities to the university's nursing students, who often struggled to find clinical placements, Speerhas said.
"If you talk to the nursing students especially, one of their biggest struggles and one of the university's biggest struggles are finding clinical placements for them," Speerhas said. "So we fixed that by creating our own clinical placement. A lot of medical schools have their own practices, but I think at a nursing level, that's not the case."
After receiving a mobile health-focused grant from the Health Resources and Services Administration (HRSA), the team was "off and running," Rutledge said. "And it's been like having a tiger by the tail. We haven't been able to stop."
Getting Community Input
To get a clearer sense of the region's needs, program organizers conducted what Speerhas describes as "reconnaissance missions" in Franklin and surrounding communities.
"We would go out and just start walking the streets, literally, and knocking on doors and talking to people," Speerhas said. "'How can we help? What are your needs?' And quickly my emails and phone started blowing up."

Rutledge credits the team's decision to bring community leaders into the conversation early on, and to ask communities what kinds of services would be most helpful to them, as crucial to the clinic's success.
"We didn't go in saying, 'I am delivering this to you,' because we didn't know what the communities needed," Rutledge said. "It was important to really engage them and make it a collaboration, not something that is separate from the community."
When Rutledge and her team approached Jarratt about opening a mobile health clinic and asked if the city of Franklin would be interested in partnering with the program, "I said, 'Yes, please! Absolutely!'" Jarratt recalled. "When they told me they had a grant and a bus and they were going to bring nurses, I was like, 'Oh my goodness. I'm all in on this. What can we do?'"
By working with community leaders and other stakeholders, the ODU team has built a wide range of partnerships across the region. Partners include local social services organizations; a locally owned pharmacy that has agreed to provide prescriptions when needed; K-12 schools; a community college in Franklin, which leases a townhouse to the university for faculty and students to stay in while working at the clinic; a regional healthcare system with a mobile mammogram van, brought out once a month for a day dedicated to women's health; and the city of Franklin itself, which built a charging station for the mobile clinic and made all city properties available for the clinic to use.
A Unique Model
The mobile clinic — housed in a two-room, 38-foot RV — currently offers free care three days a week at a variety of stops around Southampton County and the Franklin area. Locations include community gathering places, local fire stations, and schools.
On a typical day, the clinic is staffed by a range of ODU nursing students, from Bachelor of Science in Nursing (BSN) students to those in the Doctor of Nursing Practice (DNP) program, with a faculty nurse practitioner overseeing things. Students earning their Associate Degree in Nursing (ADN) at Paul D. Camp Community College, a two-year school in Franklin, have also begun working at the clinic.
Some patients might come to the clinic with acute issues, such as infections or injuries, while others need general wellness exams, high school sports physicals, or assistance in managing chronic conditions. Program organizers note that the clinic is not intended to be a substitute for primary care; if a patient has fallen out of care and needs help getting back on track, clinic workers can help them to enroll in insurance or work with local healthcare providers to refer a patient to them.
The clinic's university home lends itself to an interprofessional approach: On days the clinic dedicates to specialty areas such as dental care, mental health counseling, physical and occupational therapy, and speech language pathology, students from these specialty programs are brought in to work as needed; on days dedicated to high school sports physicals, students from the athletic training program join the team. Students in other departments have been recruited to work with the clinic, too: Human services students take regular shifts, students from the Spanish department provide interpreter services, and marketing students help with outreach and publicity.
All of our students have built this program.
"We are nurse-led and student-run," Speerhas said. "All of our students have built this program. What makes it really special is that students have had input at every level, from grant writing on."
As an FNP student, Bauman said that working with students in other degree programs has given him some useful perspective, in part from being able to ask DNP students about their experience in the program.
"It's kind of nice because it's like you can see your past and you can see your future," Bauman said. "You can talk to one another, and they can ask you questions, and you can ask them questions. And in the downtime, you're still learning things."

Unexpected Impacts
Initially, Rutledge had envisioned the mobile clinic serving mostly older patients. But soon after the clinic opened its doors, it became clear that the greatest immediate demand for care lay elsewhere: in pediatrics. Days spent with the clinic parked at schools brought to light some of the common challenges faced by children in the area.
"There were so many kids that were not getting their physicals and even some kids that were getting ready to be kicked out of school because their shots weren't up to date," Rutledge recalled. "We had kids that had had major surgery that had been lost to the process and kids with asthma without treatment plans who were really suffering. And it really amazed us, the need right there.
"And so instead of jumping in with an adult population, we started with a population of children within the schools," she continued. "And from there, the adults said, 'Well, can you see me also?' And so it has been built a little bit differently than I expected, but it has really flourished."
From May through November, the clinic saw more than 500 children for back-to-school and sports physicals.
"Even the most diligent of parents might not get an appointment [with a pediatrician for a physical] for six months or more," Bauman said. "If a kid misses a physical, they might not be able to start school. And they might rely on school for the only food they get during the day. They might rely on school for their only education or their only time out of the house if they live in an unsafe household. So it really delays their care and their needs."
You don't know what you don't know until you're confronted with it.
Working in the clinic and getting to know rural communities firsthand have given Bauman a new perspective in his work: "The biggest eye-opening thing has been what we take for granted not living in a rural area, with access to healthcare," he said. "You don't know what you don't know until you're confronted with it."
After he graduates, regardless of where he ends up practicing, Bauman plans to seek out underserved rural areas nearby and spend at least one weekend a month providing physicals or other needed services to residents there. Already, three other students who volunteered in the mobile clinic have graduated and have come back to work for the university — and in the mobile clinic — in a clinical capacity.
"A win for us is to show [the students] this area of healthcare and have them fall in love with it and have them want to be a part of it," Speerhas said. "And we've already had that."

