Maine Critical Access Integrated Paramedics
- Need: With the nearest hospital more than an hour away, the local community health center in rural Jackman, Maine struggled to maintain its ability to offer 24/7 care to due to staffing and budgetary challenges.
- Intervention: Critical Access Integrated Paramedics provide urgent care to patients after hours and on weekends.
- Results: The Jackman Community Health Center has been able to offer round-the-clock care to clinic patients, while also increasing the level of EMS service available to the community.
Description
The Jackman Community Health Center had increasingly struggled to find a sustainable model for offering round-the-clock care to residents of the rural Moose River Valley region, due in part to challenges recruiting and retaining local physicians. To ensure that urgent care would continue to be available to community members 24/7, the health center and its operating organization, Penobscot Community Health Care, partnered with North East Mobile Health Services, Eastern Maine Community College, and St. Joseph Hospital in Bangor to create a new program that allows paramedics to staff the clinic and provide care after-hours and on weekends.
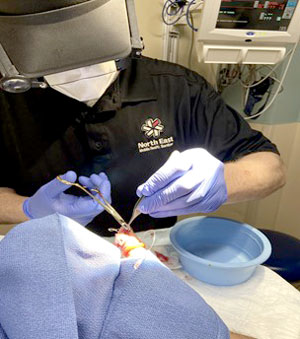
The Critical Access Integrated Paramedics program lets local paramedics broaden their skill set through online courses and laboratory sessions with Eastern Maine Community College and clinical rotations at the emergency department of St. Joseph Hospital. With this expanded training, the paramedics are able to perform services including ultrasounds, splinting, and wound care. The program also utilizes telemedicine technology, allowing the paramedics to communicate with healthcare providers at St. Joseph Hospital while they are with the patient.
The paramedics, most of whom live in other parts of the state, each work a 48-hour shift in Jackman once a week on an eight-week rotation; in the seventh and eighth weeks, they work a 24-hour shift and spend an additional 12 to 24 hours in clinical rotations at St. Joseph's to maintain and sharpen their skill set. While on shift in Jackman, the paramedics stay in apartment housing converted from a former nursing home in town.
The initiative is funded primarily through local property taxes in Jackman and Somerset County. The program also received a four-year, $1.2 million federal grant from the Health Resources and Services Administration in 2020 to help cover costs related to launching the program, such as equipment, training, and education.
Services offered
Paramedics trained through the Critical Access Integrated Paramedics program are available 24/7 to provide services to residents of Jackman and the Moose River Valley. Patients can access care after-hours in several ways:
- Patients requiring after-hours care or assistance can call the clinic's phone number from home. Those in need of services, such as scheduling an appointment to see a primary care physician or getting lab results, are referred to a night nurse triage system, while those who need urgent care treatment are told to come to the clinic.
- Patients who show up to the clinic after hours without calling ahead first can let the paramedic on shift know they are there by using a phone stationed outside the door that rings directly to the on-duty paramedic's phone.
- Patients who call 911 with an urgent care need can also have a Critical Access Integrated Paramedic dispatched and the 911 call may be converted into a telehealth urgent care visit.
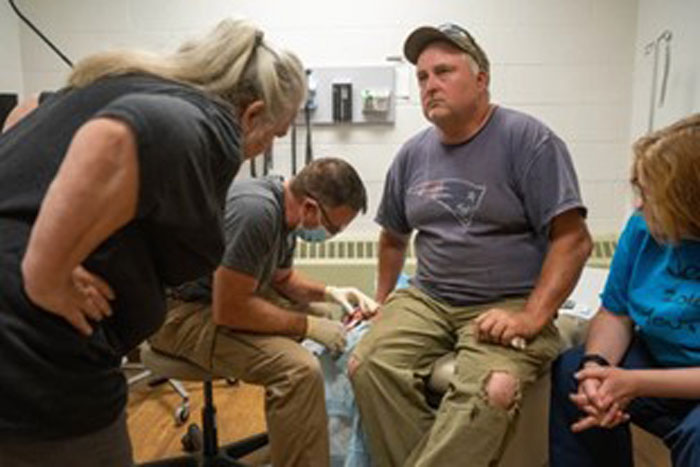
Urgent care procedures that the Critical Access Integrated Paramedics can perform include but are not limited to:
- Wound care
- Local and regional anesthesia
- Soft tissue acute foreign body removal
- Eye, ear, nose and throat procedures
- Ultrasounds
- Non-sedated joint dislocation reduction
- Fiberglass splinting
- Casting
The Critical Access Integrated Paramedics may also be called upon to assist the local ambulance service with 911 calls that require Advanced Life Support (ALS). The local ambulance service, which responds to about 80 calls per year, is volunteer-run and can provide service at the Basic Life Support (BLS) level. If a call that may require Advanced Life Support comes in, the Critical Access Integrated Paramedic on duty can be dispatched along with the volunteer ambulance service. Conversely, the Critical Access Integrated Paramedics may call on volunteers from the ambulance service for assistance if the paramedic needs an extra set of hands to help with an after-hours urgent care procedure at the clinic.
Results
The Critical Access Integrated Paramedics program has allowed Jackman Community Health Center to continue offering round-the-clock care to clinic patients, while also increasing the level of EMS service available to the community.
The program has trained four full-time paramedics and three part-time paramedics so far, and serves an average of three to four patients each week.
Challenges
Paying for the program is an ongoing challenge. The local community has committed to funding the bulk of operational costs through local tax revenues, with the remainder offset by grants and other revenue streams, but there is currently no other mechanism in place to reimburse the paramedics for their work.
There is also currently no way to fulfill medical prescriptions after hours in Jackman, although the Critical Access Integrated Paramedics initiative is now working with a local pharmacy to develop a pilot program for remote dispensing.

Replication
The Critical Access Integrated Paramedics program in Jackman was designed and developed with input from the local community, with multiple community-wide meetings to hear feedback from local residents on potential models and approaches. The leadership team for the program sees this informed community self-determination process as critical to the success of, and ongoing local support for, the initiative, and encourages anyone attempting to implement a similar program to be as transparent as possible in discussions with community members.
Because the initiative is a first-of-its-kind pilot program for the statewide Maine EMS system, the process of designing and developing the program was a relatively long one: 18 months were spent developing the clinical practice structure, and seven months were spent developing the final contracts. Other communities in Maine wishing to implement similar programs in the future may face a less time-consuming process.
In some other states, a program like this may not be legal. In 2020, the Jackman program's leadership team worked with Maine lawmakers to update state statute to ensure that Maine EMS had the authority to oversee this type of program; an earlier version of the statute focused solely on EMS in a transport context.
The physical infrastructure for the Critical Access Integrated Paramedics initiative already existed in Jackman prior to the program's creation: The town already had a clinic, and living quarters available at the former nursing home. But the leadership team believes aspects of the program could be adopted in rural areas that do not have the same infrastructure available – for instance, paramedics could provide urgent care services on a house-call basis.
Contact Information
Rick Petrie, Chief Operations OfficerNorth East Mobile Health Services
Jackman Community Health Center
rpetrie@nemhs.com
Topics
Access
· Emergency department and urgent care services
· Emergency medical technicians and paramedics
· Federally Qualified Health Centers
· Telehealth
States served
Maine
Date added
August 26, 2022
Suggested citation: Rural Health Information Hub, 2022 . Maine Critical Access Integrated Paramedics [online]. Rural Health Information Hub. Available at: https://www.ruralhealthinfo.org/project-examples/1101 [Accessed 4 June 2026]
Please contact the models and innovations contact directly for the most complete and current information about this program. Summaries of models and innovations are provided by RHIhub for your convenience. The programs described are not endorsed by RHIhub or by the Federal Office of Rural Health Policy. Each rural community should consider whether a particular project or approach is a good match for their community’s needs and capacity. While it is sometimes possible to adapt program components to match your resources, keep in mind that changes to the program design may impact results.
