Structured Training for Rural Enhancement of Community Health in Obstetrics (STRETCH-OB)
- Need: To improve maternal and birth outcomes in rural and underserved areas by increasing the number of family medicine physicians in these areas who have high-quality, evidence-based obstetrical care skills.
- Intervention: The STRETCH-OB program trains a select number of family medicine residents at the University of Illinois College of Medicine Rockford each year to provide high-quality maternity care, including surgical obstetrical care.
- Results: Four STRETCH-OB residents have graduated as of June 2025 and all have cesarean section privileges in their practice.
Description
To provide family medicine residents interested in practicing in rural areas with enhanced obstetrics and surgical skills – with the ultimate goal of improving maternal and birth outcomes in underserved communities – the University of Illinois College of Medicine Rockford (UICOMR) created the Structured Training for Rural Enhancement of Community Health in Obstetrics (STRETCH-OB) program. The program is designed to broaden the training and scope of practice of a select number of residents in UICOMR's Family Medicine Residency (FMR) program, with two to three residents chosen as STRETCH-OB participants each year. STRETCH-OB applicants indicate their interest in the program while applying to the broader FMR program and undergo an additional interview process if selected.
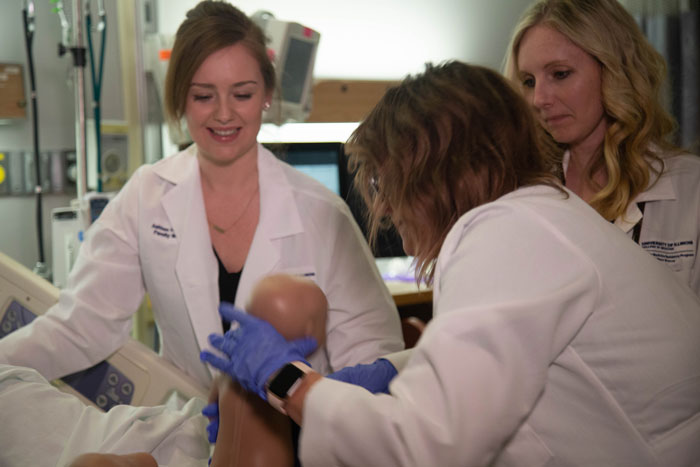
While UICOMR's FMR program already had an obstetrics curriculum that exceeded the Accreditation Council for Graduate Medical Education (ACGME) requirements for maternity care, the STRETCH-OB program builds on this foundation to provide additional training in the comprehensive management of high-risk obstetrics care and the surgical management of obstetrical patients. STRETCH-OB residents complete additional curriculum and training requirements along with the regular FMR program requirements, including rotations in rural settings.
The STRETCH-OB program launched in 2021 with federal funding from the Health Resources and Services Administration's Bureau of Health Workforce Primary Care Training and Enhancement – Community Prevention and Maternal Health program. STRETCH-OB partners include:
- UW Health SwedishAmerican Hospital in Rockford
- UI Health Mile Square Health Center – L.P. Johnson Rockford, a Federally Qualified Health Center
- Six rural healthcare systems:
- FHN in Freeport, Illinois
- OSF Saint Katherine Medical Center in Dixon, Illinois
- Gibson Area Hospital and Health Services in Gibson, Illinois
- OSF St. Mary Medical Center in Galesburg, Illinois
- HSHS St. Francis Hospital in Litchfield, Illinois
- Regional Medical Center in Manchester, Iowa
Services offered
Residents participating in the STRETCH-OB program complete all the standard requirements for board certification in family medicine, as well as additional obstetrics and gynecology rotations during the three-year Family Medicine Residency program. Additional curriculum components for STRETCH-OB residents include:
- Additional didactics for higher risk and surgical obstetrics
- Increased inpatient and outpatient OB rotations and coverage
- Two one-month rural rotations – one during Postgraduate Year 2 (PGY2) and another during PGY3 – in a primary care setting that provides OB care and with a rural hospital that performs deliveries
STRETCH-OB residents are also trained in procedures including colposcopies, bedside ultrasounds, fetal monitoring strip review, and the repair of obstetrical lacerations, and must perform a minimum of 50 Cesarean sections as a primary surgeon and act as first assist at a minimum of 50 cumulative Cesarean sections.
Results
As of July 2025, four STRETCH-OB residents have graduated and are practicing full-spectrum family medicine. All graduates have c-section privileges and work in medically underserved and/or rural areas.
Challenges
Identifying and recruiting motivated, qualified participants for the STRETCH-OB program has been one challenge of implementing the program, organizers said. The first two STRETCH-OB residents were recruited from existing PGY2 family medicine residents; in subsequent years, STRETCH-OB residents have been selected from the pool of applicants to the family medicine residency program. The STRETCH-OB program has also employed other recruitment strategies, such as creating a video specific to the program, specifically targeting medical students enrolled in rural programs, having current STRETCH-OB residents reach out to speak with STRETCH-OB applicants about the program, and having alumni of UICOMR and UICOMR's Rural Medical Education Program serve as preceptors at rural rotation sites.
Integrating the STRETCH-OB curriculum into the existing Family Medicine Residency program was also an initial challenge when launching the program. Navigating the intricacies of scheduling additional obstetrics coverage, obstetrics calls, away rotations, and obstetrics didactics took time and effort in the STRETCH-OB program's first year.
You can read more about the process of implementing the program in the article below:
- Khare, M., Zimmermann, K., Weidenbacher-Hoper, V., Ling Liao, T., Pluta, D., Garry, J. (2024). Lessons Learned in Building a Primary Care Training Program in Advanced Surgical Obstetrics: Implementation of STRETCH-OB. American Journal of Public Health, 114, S312-S313.
Replication
STRETCH-OB leaders believe their program is reproducible and offer the following advice to other institutions interested in implementing a similar program:
- It is important for residency programs to have a strong and well-developed relationship with their department of obstetrics and gynecology, as this department has been a critical partner for the UICOMR STRETCH-OB program.
- It is also important to be able to provide a component of rural training, as any exposure to rural medicine increases the likelihood that a resident physician will go on to practice in a rural site.
- Utilize community-based healthcare organizations as educational and training sites for your residents and develop relationships with rural health care partners to provide clinical rotations for residents.
- Keep in mind that opportunities created through the STRETCH-OB program are mutually beneficial for residents, who are able to receive training in real-world, medically underserved community settings; for the local and rural partners involved in teaching; and for healthcare organizations, who have an opportunity to invest in and potentially recruit STRETCH-OB residents as future physicians in the community.
Contact Information
Manorama M. Khare, Director, Division of Health Research and EvaluationUniversity of Illinois College of Medicine Rockford
STRETCH-OB
815.395.5762
mkhare1@uic.edu
Topics
Graduate medical education
· Health workforce education and training
· Maternal health and prenatal care
· Maternal health workforce
· Women
States served
Illinois
Date added
June 23, 2023
Suggested citation: Rural Health Information Hub, 2025 . Structured Training for Rural Enhancement of Community Health in Obstetrics (STRETCH-OB) [online]. Rural Health Information Hub. Available at: https://www.ruralhealthinfo.org/project-examples/1114 [Accessed 8 June 2026]
Please contact the models and innovations contact directly for the most complete and current information about this program. Summaries of models and innovations are provided by RHIhub for your convenience. The programs described are not endorsed by RHIhub or by the Federal Office of Rural Health Policy. Each rural community should consider whether a particular project or approach is a good match for their community’s needs and capacity. While it is sometimes possible to adapt program components to match your resources, keep in mind that changes to the program design may impact results.
