Outer Cape Health Services Community Resource Navigator Program
- Need: Improving outcomes for Outer and Lower Cape Cod residents in need of social, behavioral health, and substance use disorder services while reducing the burden and costs to town agencies and hospital emergency rooms.
- Intervention: The Community Resource Navigator Program works with local social services, town agencies, faith-based institutions, hospitals, the criminal justice system, and others to identify and connect clients to needed services.
- Results: Clients are gaining access to the care they were once lacking, as measured by improvements in self-sufficiency. The program also helps community partners and stakeholders work together to reduce the impact of risks associated with behavioral health symptoms, substance use disorder, and social determinants of health.
Description
The Outer and Lower Cape communities comprise the outermost 10 towns of Cape Cod, Massachusetts. Though the area is a vacation destination for thousands every year, many residents struggle to make a living. Opioid addiction, alcohol abuse, behavioral health challenges, isolation, expensive housing, high cost of living, and limited transportation impose a disproportionate impact on low-income, elderly, and other populations. Homelessness and housing insecurity have also become more common.
These and other risks related to social determinants of health are just some of the factors that have contributed to the high rates of social, behavioral health, and substance abuse issues of the area's most at-risk residents.
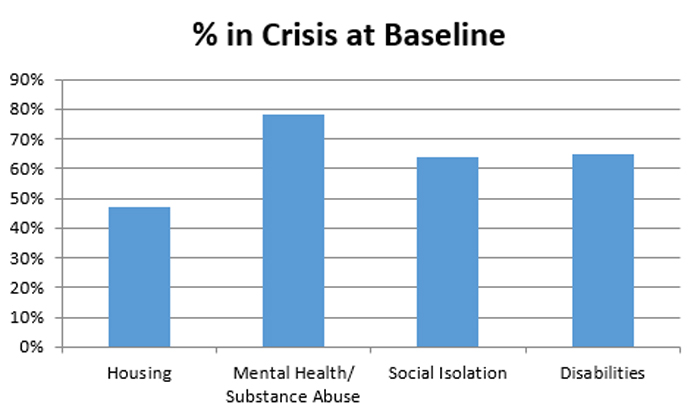
Launched in April of 2016, the Community Navigator program was designed to serve those in need who have been unable to connect with local social, behavioral, and substance abuse agencies. Following the success of the initial pilot in Provincetown, the OCHS Community Navigator program added additional Navigators covering surrounding areas, expanding to 6 Navigators serving 10 towns in the Outer Cape Health Services service area by 2022.
 The
Community Navigator program uses the Community Health
Worker model to train and deploy Navigators who seek out
referrals of potential clients through local service
agencies. The Navigators meet with willing clients in the
community and initiate a conversation in order to connect
them to the appropriate services and treatments. Their
emphasis is on facilitation and coordination of services
rather than a deep case management relationship, pointing
clients to existing service providers and programs. A
Master's level social worker located in an OCHS health
center assists clients and coordinates treatment plans
alongside the Navigator.
The
Community Navigator program uses the Community Health
Worker model to train and deploy Navigators who seek out
referrals of potential clients through local service
agencies. The Navigators meet with willing clients in the
community and initiate a conversation in order to connect
them to the appropriate services and treatments. Their
emphasis is on facilitation and coordination of services
rather than a deep case management relationship, pointing
clients to existing service providers and programs. A
Master's level social worker located in an OCHS health
center assists clients and coordinates treatment plans
alongside the Navigator.
The Community Navigator program acts as the "glue" that helps clients access services in a coordinated fashion. Regular roundtable discussions connect area services that share the common goal of helping those who have fallen through the cracks. This program partners with numerous agencies to point clients to specific services. Below are just a few of them:
- Outer Cape Community Solutions Network
- Nauset Interfaith Association
- Homeless Prevention Council
- Helping Our Women
- Sustainable CAPE
- Lower Cape Outreach
- Housing Assistance Corporation
- Cape Cod Community College
Funds for the Community Navigator program have come from town and institutional grants awarded from the following organizations:
- Town of Truro
- Town of Wellfleet
- Town of Eastham
- Cape Cod Healthcare
- Outer Cape Health Services
- Massachusetts League of Community Health Centers
- Health Resources & Service Administration Access (HRSA) Increases in Mental Health and Substance Abuse Services (AIMS) grant
Services offered
The Navigator's function is the central part of the Community Navigator program. Below are the ways the Navigator assists clients:
- Builds a trusting relationship with the client in a community setting.
- Collects data on services the client needs. Connects client to those services or advocates for particular services if they do not already exist.
- Seeks out clients who need urgent mental healthcare and provides quick access to providers.
- Collaborates with the social worker to build a coordinated treatment plan for each client.
- Helps the client keep medical appointments and secure transportation.
- Maintains regular communication with clients and agencies to track progress.
- Facilitates communication with the client's social and professional networks.
- Finds funding for the clients to improve their health and quality of life for things like home repair, dental work, nutrition counseling, and primary and mental healthcare.
- Tracks each client's progress towards personally defined goals by administering a self-sufficiency matrix questionnaire every 3 months for the first year of participation.
Results
Through the Community Navigator program, patients seeking treatment have been referred to Outer Cape Health Services for office-based opioid treatment and to providers on and off the Cape for outpatient substance abuse treatment and detox programs.
The chart below shows the breakdown of outgoing referrals made by Community Navigators.
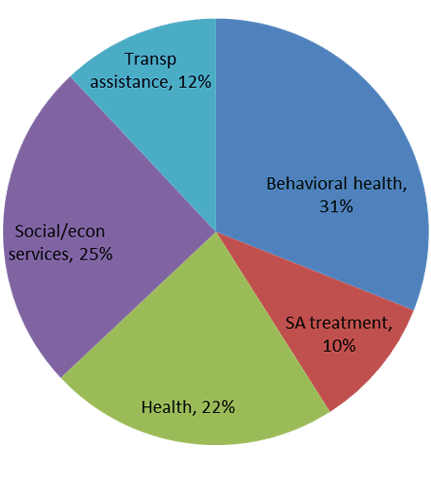
The Community Navigator program has become so successful that other towns and agencies have been quick to replicate and expand the program. The towns of Truro, Wellfleet, and Eastham have joined together to fund their own Navigator, and Cape Cod Healthcare has helped fund another new Navigator position on the Lower Cape. Funding from other towns and HRSA have enabled expansion to the towns of Orleans, Brewster, Chatham, Harwich, Dennis, and Yarmouth via 4 Navigators.
Challenges
Since its start, the Community Navigator program has experienced some difficulties, including:

- Clients' suspicion or immediate distrust of any service provider can cause difficulty getting their information and connecting them to needed services.
- Identifying potential clients takes a lot of time and collaborative efforts. While partnerships with area services have been helpful, there have still been people left unnoticed.
- Working with other agencies can generate concerns around potential duplication of efforts. In light of this, the Community Navigator program has made an increased effort to establish themselves, not as an end-all, but as a resource for already-existing agencies.
Replication
Important concepts for anyone considering a Community Navigator program:
- Take appropriate time to foster relationships with clients to build trust.
- Listen to your client's needs and go at a comfortable pace for them using a client-directed approach.
- Meet with residents who are well-established in the community to point you to those who could best benefit from your services.
- Clarify the role clearly and intentionally to other agencies. Develop resources that explain your purpose and list committed partners.
- Offer to facilitate regular roundtable discussions with other service agencies as a way to get everyone on the same page and provide the best care coordination for clients.
- Integrate navigation services within an established community health center.
One of the key tenets of the Community Navigator Program is the use of assessment instruments to determine needs related to social determinants of health (SDOH) such as housing, nutrition, criminal justice involvement, and employment.
The Navigators administer tools including a modified Self-Sufficiency Matrix and the PRAPARE Implementation and Action Toolkit to assess the needs related to SDOH. OCHS has built a significant database around SDOH scores and is beginning to do predictive modeling using this data to inform service plans and risk tiers.
Contact Information
Leo Blandford Outer Cape Health Services508.905.2800
gblandford@outercape.org
Topics
Behavioral health
· Care coordination
· Human services
· Social determinants of health
States served
Massachusetts
Date added
June 24, 2016
Suggested citation: Rural Health Information Hub, 2023 . Outer Cape Health Services Community Resource Navigator Program [online]. Rural Health Information Hub. Available at: https://www.ruralhealthinfo.org/project-examples/911 [Accessed 8 June 2026]
Please contact the models and innovations contact directly for the most complete and current information about this program. Summaries of models and innovations are provided by RHIhub for your convenience. The programs described are not endorsed by RHIhub or by the Federal Office of Rural Health Policy. Each rural community should consider whether a particular project or approach is a good match for their community’s needs and capacity. While it is sometimes possible to adapt program components to match your resources, keep in mind that changes to the program design may impact results.
