Feb 12, 2014
Patient Simulators Sharpen Skills of Rural Practitioners
The clock is ticking. On a cold winter morning in rural South Dakota, Joseph, 53, wakes up with crippling chest pain. Because permanent damage or death from heart attack generally occurs in the first hour after blood flow to the heart is blocked, timely treatment is critical for positive patient outcomes. However, in rural areas, timeliness and provider proficiency can be compromised by long distances to the nearest hospital and low patient volumes that result in emergency responders not getting enough practice. Fortunately, Joseph has been created for this purpose. He is a human simulator used by South Dakota Simulation in Motion (SIM-SD) for healthcare simulation training.
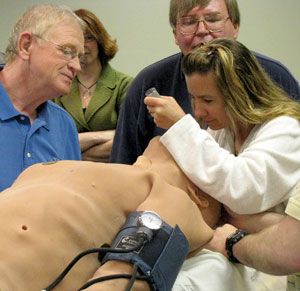
Simulation training using computerized patient manikins has become one of the most promising innovations in healthcare education, according to Dr. Paul Phrampus, Immediate Past President of the Society for Simulation in Healthcare (SSH). This rapidly growing field of medical education enhances professionals' competency by giving them practice in critically important but often little-used skills. The greatest benefit, Phrampus said, is the improved patient safety that results from practitioners' increased efficiency and reduction of errors.
"In our small communities, most of our ambulance services are volunteers that may have no more than 15 to 20 calls a year," said Clara Johnson, a SIM-SD site coordinator. "They might only see one or two heart attacks a year. It's hard to maintain expertise and feel comfortable when your exposure is so limited. With simulation education, we replicate actual situations in a realistic environment like the one where they work."
Mobile simulation decreases participation barriers. The emergency medical technicians (EMTs) caring for Joseph were actually working in the back of the SIM-SD custom-built mobile learning lab equipped as a facsimile of an ambulance. The front section of the 44-foot truck houses a realistic hospital emergency bay.
SIM-SD annually provides training for 124 ambulance services and 50 hospitals throughout the state. In Missouri, the 30-foot Mobile Sim, equipped with more than 110 medical scenarios, travels to rural communities for training re-enactments. Offering mobile simulation improves the likelihood that low-volume areas will receive the training they need, Johnson said. Volunteer ambulance crews already take time away from their income-producing jobs to respond to ambulance calls, and rural hospitals struggle with understaffed departments. Sending rural staff outside the community for professional education is expensive and less likely to happen.
Simulation opens new educational opportunities, according to Halley Lee, Director of the South Dakota Office of Rural Health (SDORH). "We couldn't replicate these situations using a live patient without risking harm to the individual. These scenarios and simulators become very real, very quickly for our participants. The simulators are so lifelike that it's hard to imagine unless you've seen them in action. They talk, they cry, they breathe, they pulsate, they respond to medication. They can die— and be brought back to life."
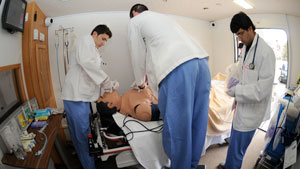
Simulation effectiveness is evident in the immediate feedback that practitioners receive when they realize how their actions might have affected a live human patient, said Dena Higbee, director of the University of Missouri Shelden Clinical Simulation Center (SCSC) in Columbia. "If they give a wrong drug dosage, the simulator's heart rate and respiration goes up accordingly with how that specific drug interacts with the body. We see our people come out fully realizing what might happen to a real patient if they make a mistake like that. It's very effective."
Training scenarios vary widely among locations, often being tailored to specific needs and sometimes starting outside the trucks so practitioners can utilize skills such as stabilizing and moving patients into the ambulance. Emergency responders may have specific requests; for instance, rural Missouri EMTs requested more practice in delivering babies. Although the intent is that ambulance crews don't deliver babies, Higbee said rural crews may be so far away from definitive care when they respond to an OB call that sometimes they have no choice but to deliver the baby.
Both mom and baby are simulators. South Dakota and Missouri trainers use simulators of various sizes, sexes and ages depending on the scenario. "The pediatric manikins offer valuable hands-on experience because EMTs aren't likely to see a lot of children," Higbee said. "Children's anatomy and their reactions differ from adults."
Instructors that create and implement the controlled scenarios observe scenarios from behind a one-way mirror. Virtual reality devices record the sessions for later review and assessment with participants.
Simulation learning also improves behaviors such as effective communication, teamwork and decision-making, Phrampus said. "In traditional curriculums, these kinds of skills are only addressed in a cursory fashion. They are critical to effective patient care. We can create team environments that demonstrate proper communication and teamwork and how they actually impact patient care."
By practicing communication and teamwork interactions, medical personnel are better prepared to make sound decisions, respond quickly and be prepared for the unexpected, Higbee said. Planned scenarios include teamwork and communication components; for instance, human actors may play roles such as distraught family members.

Substantive data qualifying simulation's effectiveness is difficult to develop given the wide range of simulation practices and the low frequency of occurrences, according to Phrampus. The University of Pittsburgh's Peter M. Winter Institute for Simulation, Education and Research (WISER), where Phrampus is an emergency physician and director, has documented simulated training that demonstrates significant reductions in specific situations. Reduced complications related to airway management is one example where results were so convincing that the University of Pittsburgh Medical Center requires medical staff to annually participate in airway management simulation education.
"Unanticipated difficulties in airway management are relatively uncommon so practitioners don't get a lot of exposure," Phrampus said. "But when it happens, it can put patients at risk for brain damage and death if not rectified quickly. When you look at rural areas where there are low volumes and limited diversity in cases, it means those folks may not be getting what they need to maintain skills. Simulation gives them a structured practice ground that allows skills refreshment of varying depth and variety."
Simulation complements traditional learning, he stressed. Traditional learning is based on cognitive knowledge relying on written testing. Simulation enacts performance assessments that test how the individual utilizes that cognitive knowledge.
"The importance of simulation to health care is just blossoming and we are going to see its practice and educational opportunities continue to dramatically grow," Phrampus asserted. "SSH is encouraging collection of data that demonstrates specific value in simulation. That body of science will eventually reach the tipping point where it will achieve the relevance that payers and regulators need to feel comfortable to then require simulation for continuing practice."
The 10,000 square-foot Shelden Clinical Simulation Center offers simulation education for all interested practitioners whether or not they are affiliated with the University of Missouri. A wide variety of medical, pharmacy and nurse practitioner students, respiratory therapists, helicopter flight crews, practicing nurses and physicians train at the facility. Mobile Sim, which went on the road in spring 2011, is supported by a $288,133 grant from the Health Resources and Services Administration (HRSA).
SIM-SD, which began operation in 2010, uses a nationally standardized training curriculum throughout the state. SIM-SD added a North Dakota counterpart last year and is sponsoring school-based scenarios known as Scrub Camps to foster student interest in healthcare careers. The Leona M. and Harry B. Helmsley Charitable Trust funds SIM-SD through the SDORH.
Back to: Winter 2014 Issue
