Feb 12, 2014
Technology Widens Care Options for Rural Hospitals

Rapidly advancing technological developments are helping rural hospitals save patients—and themselves. Throughout the country, hospital leaders are looking at ways they can strengthen their bottom line using technologies that better serve their communities and keep patients closer to home.
In Michigan, urban surgeons perform complex procedures at small Critical Access Hospitals (CAHs). Robotic surgery expands physician and hospital capabilities in Minnesota. And in Washington, medical robots place remote physician specialists at the bedside of critically ill patients.
"Ten years ago, what we're doing wouldn't have been possible," asserts Michigan Rural Healthcare Preservation (MRHP) CEO Ethan Lipkind. "There have been astronomical strides in medical technology that have improved engineering, and advancements that have made it possible to provide sophisticated procedures in settings that were previously impossible. And we can do all of it in an exceptionally safe environment that benefits both patient and hospital."
Today's patients are smart and savvy, and they request best practice options such as robotic surgery, according to Joy Johnson, chief operating officer at Sanford Bemidji Medical Center (SBMC) in Bemidji, Minn. Patients want to stay close to home for care but they will travel long distances for best practice surgical options, Johnson said, adding that rural hospitals must be proactive technologically to maintain a solid bottom line.
"The old paradigm was that a hospital's purpose was to aggregate all the professionals in one place and bring patients there," says Tom Martin, CEO at Lincoln Hospital in Davenport, Wash. "Now that ability is changing to us bringing the professionals to where the patients are."
Increasing Treatment Access
Lipkind knows of no organization similar to MRHP, a nonprofit network created in 2010 to help remote rural hospitals remain operational by developing environments that offer patients the advantages of the latest technologies. MRHP collaborates with CAHs in Deckerville and West Branch to operate a surgical program where four urban surgeons travel to the CAHs to do neurosurgery, complex urology, spine and orthopedic surgeries, fusion procedures and advanced pain care management.
"The traveling surgeons are the lifeline of this arrangement," Lipkind commented. "Patient outcomes have been stellar. In these small rural hospitals, the focus is on one individual patient at a time. So these patients get more individualized care."
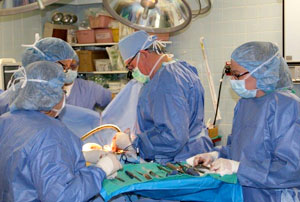
Mary Ann*, a patient with a lumbar disk injury, terms her surgical experience "fantastic." Dr. Gerald Schell, a board certified neurosurgeon with Michigan Clinic Neurosurgery in Saginaw, performed Mary Ann's multilevel spinal fusion in the Operating Room of the 15-bed Deckerville Community Hospital (DCH).
"I was treated like family from walking in the door until being discharged," Mary Ann said. "The staff went above and beyond the call of duty."
According to DCH Chief Financial Officer Valerie Bryant, the surgical program has stabilized DCH financially, improved employee morale and been embraced by patients. DCH's upfront investments included equipment upgrades and staff training.
"It takes additional nursing and clinical staff because we need all hands on deck the days these surgeons come in," Bryant said. "We have to take care of our patients in the hospital and put more staff in the OR. But the benefit has definitely outweighed our additional expenses."
MRHP is expanding surgical options at these network hospitals and has begun working with two more rural hospitals to develop programs specific to their needs. Lipkind said MRHP is also affiliated with physician offices, the Field Neurosciences Institute and Central Michigan University College of Medicine.
Robotic Surgery Offers New Options for Rural Patients
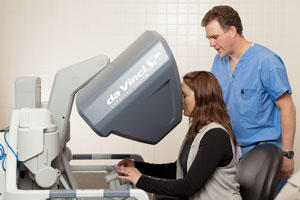
Sanford Bemidji Medical Center in Bemidji and Essentia Health-St. Joseph's Medical Center in Brainerd are two rural Minnesota hospitals that have installed the da Vinci Surgical System, the first robotic surgical system approved in 2000 by the FDA. The system has a camera that provides a multi-dimensional view inside the patient's body and a minimally invasive robotic arm with a pivoting wrist that can manipulate microscopic instruments in tiny areas inside the body. The surgeon navigates all aspects of the surgery from an exterior panel.
Currently, both hospitals are offering robotic procedures in the areas of general surgery, urology and gynecology. Difficult surgeries that couldn't have been done in the past at Essentia Health have become common procedures because of the minimally invasive technology using the robot, according to Essentia Health Urologist Dr. Scott Wheeler.
"Robotics take the minimally invasive world one step further," commented Dr. Hal Leland, an Essentia Health obstetrician/gynecologist who performs robotic surgery.
"Robotic surgery is significantly less invasive with less trauma to the body than there is even with minimally invasive surgeries," Johnson concurred. "Patients want robotic surgery because it means shorter hospital stays and faster recoveries for them. New physician surgical grads are trained in robotic surgery and they want to use those skills. If patient retention and physician recruitment are negatively impacted, that can impact a hospital's bottom line."
SBMC, which has 90 acute care beds, is at least 150 miles from the nearest tertiary centers so patients were traveling or being transferred long distances for critical services. Four years ago the board of directors adopted a strategic plan to improve patient care and safety by developing SBMC as a regional referral center. In addition to the robotic program, other high-tech improvements since then include a new cardiac program with 24-hour STEMI service, and a cardiac catheterization laboratory and a chronic wound program that includes hyperbaric oxygen therapy and advanced wound care.
"Hawkeye" the Robot Brings Specialty Care to Local Hospitals
According to the Washington State Hospital Association, the state's 38 CAHs are the healthcare cornerstone in rural communities, and their viability is threatened. Among the CAHs implementing innovative approaches to stabilize their operations is Lincoln Hospital, the first Washington CAH to use a robot to manage care for patients who have had strokes. Lincoln soon extended the program to include hospitalist management for all complex care patients. Within the first year of Lincoln Hospital adding the robot (which they call "Hawkeye") to its staff in 2010, patient transfers decreased by 24 percent and admissions increased by 21 percent, representing a $1 million increase in revenue. Martin said other benefits include shorter patient hospital stays, fewer patient hospital readmissions and improved post-discharge patient management.
Contrary to the administration's fears that patients and staff might react negatively to a robot, Hawkeye was an immediate hit. "It's really amazing to watch Hawkeye at work," Martin commented. "These remote specialists basically see everything in the patient that a doctor in our hospital does. And the stethoscope quality is so good that there isn't any deterioration transmitting heart and lung sounds."
A 25-bed critical access hospital in a CMS-designated frontier location, Lincoln Hospital simply didn't have high enough patient volumes to justify hiring a full-time critical care specialist. But an outside review indicated that 38 percent of patients transferred to Spokane over a six-month period could have remained at Lincoln if critical care management was available.
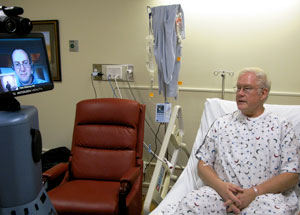
"Our doctors are very competent but they weren't getting that inpatient exposure and skills usage that urban specialty doctors do, so they didn't always feel comfortable keeping complex patients here," Martin explained. "As they started using Hawkeye, they agreed it was extremely beneficial to have another set of eyes on their patients. With this additional clinical support, they have the ability to care for more patients here."
Currently, 14 rural hospitals in Washington state use TeleStroke, and three are developing TeleHospitalist. Critical care specialists or hospitalists at Providence Health Care (PHC) in Spokane provide 24-hour support to the rural physicians and hospitals. According to PHC Telehealth Program Coordinator Denny Lordan, PHC is developing TelePediatrics, TeleMental Health and TeleCritical Care. PHC also assists the rural hospitals with implementation to assure adherence to standard practice guidelines.
"Having subspecialists that we can make available to partner hospitals in the region elevates the level of care that rural patients receive in their own communities and helps to keep care local," Lordan said. "When we keep appropriate patients in their own communities, we also free up higher acuity beds at Providence for patients that need that level of care."
While these administrators are enthusiastic about high-tech solutions, they also agree that success won't happen without community education and support, a financial investment, and willingness to partner or network with other healthcare providers.
"I think as rural hospitals we have to realize if we are going to grow and use our facilities to the fullest extent, it's essential that we bring specialists into that mix," Martin said. "Newer technologies offer opportunities that rural hospitals should be evaluating. Clearly, we have to be willing to become part of a system of care where integrating clinically with large systems using this technology affords us the ability to remain independent. Technology affords us a new perspective. We've stopped looking at our feet and started looking at the sky."
* To ensure patient privacy, the Rural Monitor only uses patients' first names.
Back to: Winter 2014 Issue
