Nov 20, 2019
Diagnosing the Rural COPD Patient: Ask About Symptoms, Use Spirometry
Related Article
Office-Based
Spirometry: Key to Diagnosing Rural COPD Patients

In rural America, chronic obstructive pulmonary disease, or COPD, claims a lot of lives. Recent data indicate that not only does COPD have almost double the prevalence rate in rural areas, but almost double the mortality rate when compared with large urban areas. As the third leading cause of death from chronic diseases, COPD has a mortality rate that is steadily rising in comparison to the other top five causes of death, which have stable or decreasing mortality rates. Federal agencies note that 3.5 million people living in rural areas have COPD, a condition which has no cure, but has treatments to improve these people's lives. Experts are also concerned because many rural citizens — maybe hundreds of thousands — have COPD but don't know it. Changing these rural statistics starts with suspecting COPD and getting patients accurately diagnosed.
Which Patients Might Have COPD?
Dr. Barbara Yawn, a rural family medicine physician who is also a clinical researcher, has long championed the issues around the diagnosis and treatment of COPD. Currently the Chief Scientific Officer for the COPD Foundation, she's participated in many national collaborative meetings and specialty gatherings and published extensively on many aspects of the condition. She explained that diagnosing COPD starts with recognizing common symptom patterns associated with COPD.
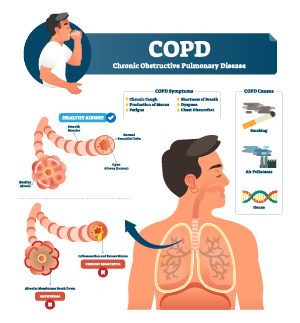
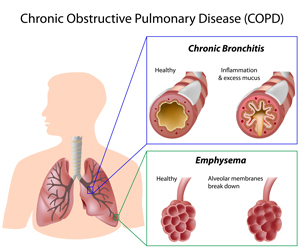
Defining COPD
COPD is an umbrella term for describing chronic respiratory diseases — including emphysema and chronic bronchitis — that are usually progressive and affect the lung's airways and lung tissue.
"When we talk about recognizing people with
COPD, we often don't recognize them until they
are in their 50s and 60s," Yawn said.
"We need to start thinking about patients
having COPD at an earlier age. And though we need to
think about COPD in current and former smokers, in rural
areas there are also several other important exposures
such as grain dust, chemicals used in farming, exposures
from mining, logging, wood fire stoves, and even the
occupational exposures experienced by hair dressers or
bakers."
Workplace Exposures Can Also Lead to COPD
As Yawn indicated, COPD is not just a condition seen in smokers. Twenty-five percent of patients with COPD have never smoked. Environmental exposures such as grain dust, grain molds, and other inhaled particles she referenced can trigger the development of chronic lower respiratory diseases. Learn more about rural occupational lung diseases in the Rural Monitor article Pulmonary Health in Rural America: Cause and Impact of Work-Related Lung Diseases.
"Unlike asthma, many people with COPD may not
have much wheezing, but they'll have recurrent
respiratory illnesses that often get called acute
bronchitis or a 'bad cold,'" Yawn said.
"These are the patients who say, 'Yeah, I've
had this cold for a week or two, and I'm not getting
better.' Or they might tell their family or friends,
'Every year, I get one or two or three of these colds and
they always last longer than anyone else's cold. But the
doctor gives me antibiotics and I'll get better.' These
are the people that we really have to pay attention to
and put COPD in the differential diagnosis."
Yawn said there are other symptoms indicating possible COPD that sometimes go unnoticed, even by patients themselves.

"Another group of people with COPD go unrecognized because they don't have these acute, recurrent respiratory episodes," she said. "Instead, they've just stopped doing things or slowed their normal pace because they're short of breath. It's not that they're withholding information from you, because what's happened is that they've just gotten short of breath so gradually, they've naturally compensated for it."
She said just asking several questions about specific activities can actually help identify this group.
"I often ask them this: 'Do you walk more slowly than other people your age?'" she said. "If they answer yes, the follow-up question comes: 'Is it because of your breathing?' Or another question like 'Can you climb a flight of steps or walk up a small hill without getting short of breath or having to stop?' These more specific questions can help uncover lifestyle limitations. You'll start learning new things about your patients, like they now can only weed part of their garden rather than the whole garden at one time. Or that they've bought a riding lawn mower because they get too short of breath using the push mower."
Sex Differences in COPD

According to the Centers for Disease Control and Prevention, COPD and other chronic lower respiratory diseases were the third leading cause of death in women in 2017. Previously considered a condition mainly seen in men, COPD prevalence and mortality rates are now showing that COPD is more common in women. A 2014 study reviewed several sex-related issues associated with the disease's presentation in women:
- More intense shortness of breath than men
- Diagnosed at a younger age, at a more advanced stage, and having less overall tobacco use
- More likely to be misdiagnosed as asthma instead of COPD
- More likely to have chronic bronchitis versus emphysema in men
- Respond less well to treatments
- Die in higher numbers than men
- Compared to men's declining death rates, have an increasing death rate
Yawn goes on to share information concerning a third
group of patients having symptoms of possible COPD.
"Another group of patients will just blame their shortness of breath on the extra pounds they're carrying around, or that they've let themselves just get out of shape, or think that age has caught up with them," she said. "Even if these issues are present, physicians and other clinicians need to remember that these patients can still have COPD. Their symptoms may be a combination of both deconditioning and COPD."
Yawn said her favorite question to help uncover activity
limitations is a direct question: Do you have to stop
walking when you're on level ground or walk slower than
other people your age? When interviewing a patient, she
also suggested that if the spouse is in attendance, it's
equally important to notice their body language and
perhaps ask if they agree.
"The patient might be answering no to all the questions, and the spouse is sitting next to them vigorously shaking their head yes," she said.
Lastly, Yawn also emphasized that COPD doesn't usually exists as a single condition. Patients with COPD often have heart disease and other conditions that can worsen COPD — or be worsened by it.
"If a patient has worsening of their heart failure, that can cause fluid build-up in their lungs and worsen their COPD," she said. "And if their COPD worsens and oxygen levels drop, that can be a problem for the heart."
COPD Research in Rural Primary Care Practices
Currently, several researchers from around the country and the COPD Foundation are completing an NIH-funded grant that will investigate the ability of a five-question and peak flow tool to identify people with a high likelihood of having COPD. The study, referred to as the CAPTURE Study, will be done in primary care practice sites, including rural. The research focus includes identifying patients who need further spirometry/lung function testing to confirm the diagnosis.
Spirometry: The Diagnostic Test for COPD
"Spirometry is crucial in confirming the COPD diagnosis," Yawn said. "Research has shown that if we diagnose people with COPD based on symptoms alone, we're wrong 20 to 30 percent of the time. That means we may be treating the wrong condition 30 percent of the time and none of us wants to do that. The reverse is also true. Many people, especially current or former smokers, are diagnosed with heart disease. However, it may actually be COPD or they may have COPD in addition to their heart disease. You won't know unless you test lung function."
Understanding More: Lung Function, Spirometry and Diagnosis COPD
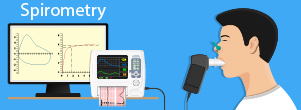 What is
spirometry? It's a test that measures lung capacity.
Learn more about the GOLD criteria, spirometry, lung
capacity testing, and spirometry numbers like FEV1 and
FVC in Office-Based
Spirometry: Key to Diagnosing Rural COPD Patients.
What is
spirometry? It's a test that measures lung capacity.
Learn more about the GOLD criteria, spirometry, lung
capacity testing, and spirometry numbers like FEV1 and
FVC in Office-Based
Spirometry: Key to Diagnosing Rural COPD Patients.
"But, you don't do spirometry on
everyone," she said. "Instead, you do
it on people with the risk factors or a suspicious
clinical presentation. Just like we do EKGs on a patient
who tells us they have chest pain, we should consider
spirometry in a patient who has shortness of breath,
especially if they have risk factors and exposure history
that go with COPD. Both EKGs and spirometry are
disruptive to a busy primary care clinic's work flow. But
these tests provide really important information. In
fact, spirometry may provide more information than the
standard EKG. I think we tend to focus on heart disease
and forget about the lungs."
According to the COPD Foundation's information, spirometry is needed because "leaving symptoms misdiagnosed, untreated, or undertreated may cause them to worsen faster than if they were treated with proper medication and therapy…providing a proper diagnosis means individuals will receive the right treatments and follow-up monitoring."
The Language of COPD Severity
The standardized reference for the severity of COPD is the GOLD criteria. The criteria were developed by an international group of healthcare and public health professionals and define COPD severity based on the amount of airflow obstruction measured by spirometry, a value referred to as the FEV1. Referring to the obstruction level as mild, moderate, severe, or very severe, GOLD criteria are often used to standardize research and by federal agencies to establish disability and pulmonary rehabilitation (PR) conditions for coverage. Patient Kandy Blankartz's airflow obstruction measures made her a candidate for both disability coverage and PR.

Blankartz, age 71, lives in Mobridge, South Dakota, a small rural town in the north central part of the state and located on the Missouri River. She has 5 children. She also has 13 grandchildren. Attending her grandchildren's sporting events, concerts, and even having lunch with them at school is a priority for Blankartz — despite the fact that she has COPD and has been on oxygen for 22 years. A State Captain for the COPD Foundation, Blankartz said her COPD diagnosis is a bit more complex since it is an overlap diagnosis that comes from several lifelong chronic lower respiratory diseases: asthma, bronchiectasis, and emphysema. She now also has pulmonary hypertension, a heart condition often linked to chronic lung diseases.
Blankartz said she's had spirometry testing over the years. Driving anywhere from 2 to 4 to 8 hours round trip to see allergists or lung specialists, she recalls some of her doctors did spirometry regularly, others less often. The results weren't routinely discussed. However, she recalls with clarity the first time her spirometry meant something important.
"I never woke up to the importance of spirometry until I changed doctors in the '90s," she said. "When that doctor did spirometry, he looked at my numbers and then he looked at me and told me they were so bad, I qualified for disability. Now, when my specialist does spirometry, I always ask about my numbers and get a copy of my results. I had PFTs [a pulmonary function test] recently, and I was really happy that my numbers have only gone down 1 point in the past 2 years."
For Blankartz and other patients with COPD, medications, oxygen, and PR are very important treatments. The Centers for Medicare and Medicaid Services (CMS) base conditions of coverage for Medicare PR program enrollment on GOLD criteria. Blankartz's spirometry results met the criteria and she said this program is "a must" for patients with COPD. She's been doing maintenance since completing the program in 2012.
"I do 50 minutes of exercise three times a week and I really believe that it's kept me doing well," she said, explaining that she can do her maintenance program in the rehab facility included in a new addition on the local hospital/clinical facility in Mobridge.
Spirometry: Only One of Several Tools for COPD Whole Patient Care

Experts like Dr. Yawn are quick to point out that although spirometry is necessary to establish a COPD diagnosis — in addition to establishing other diagnoses that cause shortness of breath — it's not used for determining treatment.
"Spirometry is no longer used as the basis for selecting therapy," Yawn said. "The choices for treatment, which include medications, pulmonary rehabilitation, and even oxygen, are all chosen based on symptoms. Of course, oxygen has additional requirements based on laboratory measures."
Along with other experts, the COPD Foundation points out that COPD is not a one-size-fits-all condition and spirometry numbers can't tell the whole story of how COPD impacts a patient's everyday life. Two or three patients with the same measure of airflow obstruction, or FEV1, can have very different levels of symptoms and activity limitations. Both symptoms and activity levels can be assessed by several tools: the COPD Assessment Test, or CAT, and the mMRC Breathlessness Scale. Experts also point out that these COPD-specific tools provide information that might be missed if standard chronic illness assessments are used to assess people with COPD.
COPD Foundation Resources The COPD Foundation endorses the whole patient care approach to COPD. It has a comprehensive set of online resources for Healthcare Professionals and a recently updated online COPD Pocket Guide interactive smartphone app.
In addition to information for clinicians, the Foundation also has released a Patient/Caregiver version that allows patients to become more active participants in their care.
Patient Blankartz said that though the specific numbers
really don't influence how you live with COPD, getting
spirometry done is very important for proper diagnosis.
"If you have shortness of breath, it's simple: You should have spirometry," she said. "It will change your life to have the right diagnosis and get the right treatments."
Resources
Rural-Specific Resources
- National Rural Health Resource Center
The Rural COPD Podcast
A Rural Hospital Guide to Improving Chronic Obstructive Pulmonary Disease
Federal Agencies
- Centers for Disease Control and Prevention
- National Heart, Lung, and Blood Institute
Health Topics: COPD
Learn More Breathe Better® - Veterans Health Administration
COPD Provider Guide
COPD Provider Quick Reference Guide
COPD Patient Guide
Advocacy Groups and Professional Associations
- American Association for Respiratory Care
- American Lung Association
- American Thoracic Society
- COPD Foundation and its 5-Question COPD Population Screener™
- Respiratory Health Association
COPD Caregivers Toolkit
For an overview of the condition in rural areas, listen to advocates, researchers, and others talk about research needs and hope for patients with COPD:

