Aug 17, 2022
Breaking the Cycle: Missouri Community Paramedicine Program Brings Primary Care to High-Risk Patients
 After 28 years as a paramedic in
Washington County, Missouri, Bryan Buckley had grown
accustomed to seeing familiar faces.
After 28 years as a paramedic in
Washington County, Missouri, Bryan Buckley had grown
accustomed to seeing familiar faces.
Some familiar faces lived in remote corners of the rural county, too far from the central town of Potosi to visit the doctor as often as needed; for others, financial difficulties or anxiety prevented them from scheduling regular check-ups to monitor their chronic conditions. One woman, a diabetic with no other means of transportation, was taken to the hospital in an ambulance at least 44 times over the course of two years. While the specific barriers to receiving preventive care differed from patient to patient, the 911 calls that inevitably followed tended to fit a similar pattern.
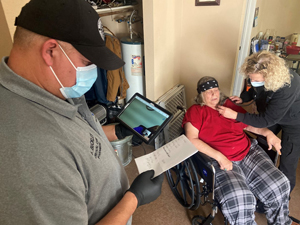
"We'd take them to the hospital, and they would typically end up in the ICU," Buckley recalled. "And then after they got to a place where they could be discharged, the whole cycle started all over again and it just kept going."
Buckley still regularly sees these patients and others with similar stories — but these days, it's typically before they call 911. A partnership between the local health center, the county's ambulance district, and a nearby community college lets community paramedics and community health workers make regular house-call visits to high-risk and chronically ill patients lacking access to reliable primary care. There, from the comfort of the patients' own homes, the paramedics can perform basic preventive care measures, conduct home assessments, serve as liaisons for writing or updating prescriptions, and facilitate telehealth visits with the health center's providers.
"Now I can actually intervene and say, okay, we've got these resources to help break that perpetual cycle," Buckley said.
By proactively bringing care to some of the community's most at-risk residents through a uniquely collaborative process, Washington County's Mobile Integrated Healthcare Network (MIHN) is catching patients who had previously fallen through the primary care cracks before they reach the point of medical crisis — while bringing down costly and avoidable hospital visits and freeing up limited emergency resources. The initiative's leadership team sees the MIHN as a model for other rural communities with similar challenges in Missouri and beyond; already, they're working to make the program replicable across the state.
"It's about changing that mentality of, 'We've always done it this way,'" said Washington County Ambulance District Chief Justin Duncan. "We're breaking down silos — not only at the provider level or the individual community level, but at the state level and hopefully at the national level as well."
An Unusual Partnership
The Washington County program is the first initiative of its kind in Missouri — and, to the leadership team's knowledge, the first of its kind in the country — to center on a partnership between a Federally Qualified Health Center (FQHC) and an ambulance district, making it unusual among Mobile Integrated Healthcare (MIH) programs.
The concept for Washington County's MIHN model emerged from conversations in 2020 between the regional FQHC — Great Mines Health Center, located in the county seat of Potosi — and the Washington County Ambulance District. Circumstances brought about by the COVID-19 pandemic, including an increase in downtime for EMS and clinic staff and changes to telehealth reimbursement rates, had opened up new possibilities for addressing a longstanding challenge: reaching chronically ill patients who, for a variety of reasons, weren't able to access regular primary and preventive care, relying instead on 911 calls and emergency care. In Washington County, a federally designated Medically Underserved Area (MUA) where one in five residents live in poverty, widespread "serious issues" with health literacy have contributed to this pattern, Duncan said.
Most people, when they think of an ambulance, they think of red lights and sirens swooping in to save the day… The reality is, for many people, we are primary care."
"Most people, when they think of an ambulance, they think of red lights and sirens swooping in to save the day," Duncan said. "Very little of that actually happens. The reality is, for many people, we are primary care."
The MIHN program began as a pilot project focused solely on care and education for diabetic patients — but as the model proved successful, the leadership team expanded the initiative's reach to include high-risk patients with other conditions as well. The program has also expanded to offer COVID-19 testing, vaccinations, and infusions, and has since partnered with the St. Louis Food Bank to deliver food to MIHN patients once a month.
The barriers to accessing primary care that some patients face in Washington County aren't unique to the area — nor are the concepts of Mobile Integrated Healthcare or community paramedicine.

But the partnership between Great Mines Health Center and the local ambulance district — and the broader collaborative nature of the program — make the Washington County initiative stand out as a new kind of MIH model that could be replicated in other rural communities, said Katherine Lloyd, a public health analyst with the Federal Office of Rural Health Policy who serves as the project officer for the program. The Washington County initiative is one of 16 programs nationally to have received four years of funding from the Federal Office of Rural Health Policy's Healthy Rural Hometown Initiative, a new funding track under the Rural Health Care Services Outreach grant program.
Across Missouri, a handful of other rural communities have begun to develop and implement their own versions of the MIHN program, with the Washington County team providing guidance and assistance as needed. As each community looks to address its own unique challenges with the resources it has at hand, some are finding that variations on the model — such as building their program around a partnership between a hospital and hospital-based EMS service — better fit their area's needs.
"That's the strength of this model: it's not just germane to FQHCs and EMS," said Greg Roeback, chief executive officer of Great Mines Health Center. "It's whatever works best for that community."
Non-Medical and Medical Care
As a community paramedic with the MIHN, Buckley sees an average of four to five patients a day, with each visit tailored to that patient's individual needs.
Determining what exactly those needs are requires first establishing a relationship with each patient, Buckley said.
"I sit and I talk with them, because one of the biggest things is building trust," Buckley said. "I don't talk over people and I don't talk down to people — I talk to them and connect with them on a real level. And once you have that trust, they start letting you know what's going on, and then you can start connecting them with resources to improve their lives."
Patients eligible for the program include those who were recently in the hospital for COVID-19 or other ongoing illnesses and require medical follow-up, new and longtime patients with diabetes who have difficulty managing their condition, patients with heart conditions or high blood pressure, and anyone else whose healthcare provider refers them to the MIHN.
Services begin with a home assessment, in which MIHN staff examine and analyze the patient's living quarters for basic amenities, cleanliness, social environment, and potential safety hazards. If any easily fixable issues are identified in the assessment, MIHN staff can address those issues on the spot. In the case of one patient who repeatedly called 911 for falls after having a stroke, Buckley found through a home assessment that the hand railing on the man's stairs was on the side of his body weakened by the stroke — and was able to install a hand railing on the man's stronger side instead.
The non-medical care is just as important as the medical care.
"The non-medical care is just as important as the medical care," said Rebekah Jones, chief operating officer for Great Mines Health Center. "If we can address those barriers to prevent medical issues, then not only are we offering better quality care, but there is a huge cost avoidance to our system."
MIHN workers also conduct a medication reconciliation with patients at home to compare medications prescribed to them by different providers and ensure that they're taking an appropriate dosage of each. Through this process, it was discovered that one patient had been taking five prescriptions from five different doctors — all for the same medication.

Community paramedics with the MIHN can perform basic procedures such as conducting physical assessments, taking vital signs, conducting in-home lab draws and point-of-care lab testing, wound care, starting and managing IVs, performing electrocardiograms and ultrasounds, and other forms of preventive and post-discharge care. They can also serve as liaisons for telehealth visits with providers at Great Mines Health Center, allowing patients to see physicians from the comfort of home.
After telehealth visits, it's not uncommon for patients to have questions, Buckley said.
"The typical question I get asked is, 'Okay, what did they say?'" Buckley said. "And then I'm able to put it in layman's terms and help them understand why it's important to them. That's when I've seen some of my patients start to take charge of their healthcare."
To offer the same level of telehealth care to patients living in more remote parts of the county with weak or no internet access, the program added a mobile hotspot to its toolbox. The hotspot travels in the MIHN vehicle, along with refrigerators to transport blood and urine samples for testing and other equipment.
"The mobile unit was crucial for us," Jones said. "It allowed us to not have to take all the equipment into the patient's home, and it allowed us to have a clean storage area for transportation."

Building a Homegrown Workforce
All community paramedics and EMTs working with the MIHN are also certified as Community Health Workers (CHWs); a new program at Mineral Area College (MAC) in nearby Park Hills, Missouri, allows students to earn both their paramedic certification and their CHW certification at the same time. To make the MIHN model more easily replicable across Missouri, Duncan and the rest of the leadership team are working with the state health department to develop and formalize a streamlined dual-certification curriculum statewide.
As part of their training, students in the EMS education programs at MAC work with the MIHN and other EMS providers in the region to conduct vaccine clinics and gain other hands-on experience with patients. Through a six-year partnership agreement signed in 2019, the Washington County Ambulance District helped to lead the development of the community paramedic and CHW programs at MAC, and it continues to partner with the college to grow and operate its EMS programming.

In this way, the local community is essentially "creating its own community health worker and community paramedic workforce," said Doris Boeckman, who serves as project director for the MIHN.
"They're growing their own by doing the training themselves, then placing the trainees for that hands-on experience, then employing them," Boeckman said.
With grant support, MAC is able to offer the community paramedic program at no cost to students. Thirty students have graduated from the community paramedic program so far; another dozen will begin classes this month, with a waiting list for the following semester. While students in the first two cohorts primarily came from Washington County and the surrounding region, the incoming class hails from a range of rural communities across the state that are working to implement their own MIH and community paramedicine programs.
"We get to help be a part of building the workforce pipeline," Duncan said. "And what the program has proven is that we have people lined up who want jobs. If we just pay for a little workforce development, they'll show up."
Finding Better Outcomes
In its first year, the MIHN program served 21 patients — and saw a 100% decrease in emergency transports across all participants.
"Our goal was to really hone in on patients who were utilizing the emergency department for primary care," Jones said. "These were patients who were calling EMS on a regular basis and weren't really seeing better outcomes — just outcomes that met their emergency need at that moment."

One patient, a man with limited mobility and multiple chronic conditions including diabetes, hypertension, and chronic obstructive pulmonary disease, had canceled 10 clinic appointments in a year before enrolling in the MIHN program, due in part to anxiety around visiting the doctor's office.
The house-call model "takes a lot of anxiety out of having to do doctor appointments," the patient wrote in a letter to MIHN staff, adding: "Getting in a car…to get to destinations is a very hard task. I commend the professional treatment I get from the EMTs."
Another patient, a man with numerous chronic conditions including atherosclerotic heart disease and a history of strokes, hadn't received any medical care since 2013 due to a lack of insurance and an inability to pay for care out of pocket. With the help of MIHN staff, he was able to enroll in Medicaid and receive the specialized care he required.
The MIHN team points to the broader financial impact of the model and its potential to save the healthcare system money, using the example of the patient who was transported to the hospital in an ambulance at least 44 times over the course of two years. In 2020, prior to enrolling in the MIHN program, that particular patient's healthcare costs for the year totaled upwards of $118,000. After enrolling in the MIHN program last year, her total year-to-date medical costs for 2022 are just shy of $5,000.
Replicating that patient's situation — "which is not an outlier" — by hundreds or even thousands of patients across the state could lead to significant cost savings over time, Jones noted.
Still, funding the MIHN program itself remains a challenge. While telehealth services are reimbursable under Medicaid in Missouri, community paramedic and community health worker services are not — leaving the remainder of the program grant-funded and the financial sustainability of the current model uncertain.

A Statewide Model
Among other rural Missouri communities implementing their own versions of the MIHN, no two iterations of the model look the same: while Adair County in northern Missouri has designed a program that's similarly based on a partnership between an FQHC and the local ambulance district, Polk County in southwestern Missouri is developing its own version through a partnership between an acute care hospital and hospital-based EMS service.
"They are all a little bit different," Boeckman said.
The MIHN has already expanded within southeastern Missouri's Lead Belt region; the program has partnered with the ambulance district in St. Francois County, Washington County's neighbor to the east, to serve patients there using the same community paramedicine model with local paramedics.
For communities interested in developing their own versions of the Washington County model, the leadership team emphasizes the importance of partnerships, collaboration, and finding common ground.
"You have to look at it from the patient's perspective," Jones said. "Come to the table with an open mind, remember that you all want the same success for patients, and sit down together and say, 'How can we share?'"
As project director for the initiative, Boeckman — a partner at Community Asset Builders, a local nonprofit consulting firm — helped to facilitate some of these connections and conversations among relevant organizations in Washington County.
"We all have our different silos we operate out of, and we try our best to not operate with blinders on," Roeback said. "But to have somebody outside of all that who can say, 'Hey, these people are doing something similar. Why don't we all get together?' That's been vital."
Locally, the Washington County team's vision for the future of the MIHN includes expanding the program to reach more high-risk and chronically ill patients across the county. But they also hope to see the model spread statewide, particularly in rural communities that have been impacted by EMS and hospital closures.
"We have to change things," Boeckman said. "That's kind of our mantra."

