Mar 25, 2026
Unapologetically Built Backwards: ONU HealthWise, Pharmacist-Driven Healthcare Access in Rural Ohio
Several years ago, an economic report highlighting market changes in urban and rural pharmacies commented on pharmacies' position within rural healthcare delivery systems:
"When thinking about rural health care services attention tends to be drawn to rural hospitals and perhaps the availability of health care professionals such as doctors and nurses. The services offered by pharmacies, however, tends [sic] to receive less attention despite pharmacies being an integral part of the health care service delivery puzzle."
In a 2020 study, researchers found that rural Medicare beneficiaries visited their community pharmacist an average of 14 times per year versus five primary care visits — a number, the researchers said, that positions pharmacists operating at the top of their practice scope to potentially provide additional healthcare access in rural areas with physician shortages. With a 2024 policy report also echoing that previous practice scope theme, another recent study described pharmacists in rural and low-resource areas as "one of the most accessible healthcare providers" due to availability on evenings and weekends.

For the Ohio Northern University (ONU) Raabe College of Pharmacy's faculty and learners, these study results are not just research, they're reality: their university, located in Ada, Ohio, is located in a rural county surrounded by rural counties.
Stuart Beatty, PharmD, the pharmacy college dean, shared that the ONU pharmacy program has a dual focus that meets rural healthcare access challenges. The first focus is comprehensive training to provide doctoral candidates with practice-readiness for future work in any rural or urban setting that allows pharmacists to provide care according to their profession's full scope of practice — especially in states like Ohio, where pharmacists have been granted "provider status."
Beatty went on to describe their second focus.
"Although our pharmacy program originally started to meet an educational need, in recent years we've pushed program work out to meet our rural area communities' needs," he said, explaining those needs emerged as a result of the COVID pandemic and a national pharmacy franchise closure.
"We began to dovetail our educational offering while actively meeting community needs in a very unique way," he said.

Adding to Beatty's description of the school's educational offering, ONU's Michelle Musser, PharmD, professor of Pharmacy Practice, and director of Outreach Programming and ONU's Rural and Underserved Health Scholars Program (RUHSP), described how their school's work in rural communities impacts their learners' perception of their chosen profession.
"I'm from this community and I had clinical experiences in other places with academic medical centers next door," Musser said. "Yes, our students get those experiences. However, look around here. Rural is everywhere. ONU is in a rural county surrounded by other rural counties. Our students are directly involved with addressing rural communities' healthcare needs. This location allows them to discover they're actually an essential healthcare provider."
Definitions: Provider Status and Scope of Practice
Beatty said their program work has been impacted by Ohio pharmacists' recent "provider status" designation. Provider status is a phrase used in the context of describing the reimbursement eligibility of a service provided by a healthcare professional. For pharmacists, some of those services would be linked to their profession's scope of practice — scope of practice being defined as "those health care services a physician or other health care practitioner is authorized to perform by virtue of professional license, registration, or certification. Health care professionals' scopes of practice sometimes overlap reflecting shared competencies." A pharmacist's scope of practice is dictated by state law, but in general includes not just the filling and dispensing of medications, but health screenings, immunization administration, new and chronic medication oversight, and health-related lifestyle advice.
The ONU HealthWise Story: The Early Years

Completing his second decade with the university Michael Rush, PharmD, is an assistant clinical professor of Pharmacy Practice at ONU and director of operations at current day's ONU HealthWise. Like Musser, he's a native of the rural area around the university. He's led many pharmacist-driven innovations, including ONU HealthWise, the name first given to the university's pharmacist-led employee wellness service that included pharmacy services primarily offered to ONU employees and a few community members.
When a review of the 2013 Hardin County's health needs assessment prompted ONU's pharmacy faculty to brainstorm options and "how-tos" of offering needed healthcare services to the county's rural residents lacking access, Rush said he remembers looking out the window at lunchtime, seeing a food truck, and realizing ONU HealthWise might be able to make mobile services work.
The concept resonated and Raabe College of Pharmacy was awarded a 2015-2018 Federal Office of Rural Health Policy (FORHP) Rural Health Care Services Outreach Grant. That grant — along with additional funding from other sources — was used to support hiring a pharmacist and the purchase of a bus that built out ONU HealthWise to become the ONU HealthWise Mobile Health Clinic.
Rush pointed out that the mobile unit provides direct comprehensive services delivered by ONU's student pharmacists and their supervising faculty. The work includes preventive health education, medication reconciliation, medication therapy management, and chronic disease state management. Health screenings are also performed, including onsite measurements of cholesterol, blood glucose, hemoglobin A1C testing, and blood pressure. Immunizations along with additional medical care — including specialty care — are also part of the HealthWise clinical workflow.
Pharmacist care also continues between mobile clinic visits: Managed by the pharmacy telehealth and services center, phone calls are made allowing pharmacists to check in with patients, providing more education and direction when needed. Currently, the team even uses some remote patient monitoring — like wireless technology-enabled blood pressure cuffs and continuous glucose monitors — to remotely monitor and manage patients' chronic disease states.
HealthWise Mobile Clinics: Interprofessional Experiences

In short time also came the realization that these mobile services were not just an opportunity for ONU's pharmacy learners, but of value as interprofessional education (IPE) for other ONU students. While still maintaining the mobile services as a pharmacist-led healthcare access point, collaboration with nearby physician residency programs expands HealthWise services with several primary care residents now working with the mobile unit's pharmacists every month.
"I've often joked that compared to other healthcare access options that usually start with physician medical providers and add pharmacy services later, we've unapologetically built our services backwards with pharmacy services first," Rush said.
Beatty further weighed in on the pharmacist-led IPE experiences.
"As a pharmacist, you sometimes see something in a prescription that necessitates a phone call to the ordering provider," he said. "These calls are just one example that allows the other health profession students to see a pharmacist's side of healthcare delivery. It also gives them a glimpse of where each profession's strengths and opportunities lie and the importance of all professions working together for the patients."
Pharmacists at Work: The Medication Specialist — and More
For many people, interaction with a pharmacist starts with medication pickup at a pharmacy. There they usually first interact with the pharmacy technician. Shortly, the pharmacist might step away from the bench work of filling prescriptions to provide answers and advice to patients about their chronic medications or new prescriptions.
But a closer look at a pharmacist's work reveals a scope of practice that starts with the fact that they are the only health profession granted a doctorate degree as medication specialists. In the nation's pharmacies, clinics, and hospitals — and in their varied roles — they are overseeing literally billions of prescriptions filled each year, numbering about 7 billion in 2024, a number distilled to nearly 20 prescriptions per year for each American.
However, in many states, a pharmacist is not limited to filling, dispensing, and educating about medications. Instead, their scope of practice is more comprehensive and mirrors those services provided by ONU HealthWise Mobile Clinics. With immediate testing results available and in collaboration with a prescribing provider, pharmacists can guide the starting of new medications, adjusting current medications — or even stopping medications no longer helpful or causing problems. ONU's pharmacists also emphasize that, just like other healthcare providers, they must investigate and respond to other health-related patient needs.
The Story Continues: Mobility Fosters Quick Expansion to Meet Not Just Local, but Regional Needs
By the end of FORHP grant funding, Rush said, the mobile pharmacy-led services were operating smoothly in Hardin County and community trust was established. Then came the COVID public health emergency — and their work changed.
Rush shared the scope of their efforts.
"We were initially asked by the governor's office to staff 10 clinics in six counties in 60 days," he said. "However, we ended up reaching K through 12 schools, state sites, rural sites, even urban sites. Final tally? Over 30 unique locations in 14 counties in about a year's time."
Musser described that work.
"We went from rabbit barns to churches," she said. "Because ONU has a full complement of faculty pharmacists and one faculty preceptor can supervise six pharmacists-in-training, with our clinic, we were well-positioned to provide rural outreach for anyone wanting COVID-19 vaccination and testing. For our students, they not only logged mandatory clinical hours, but found themselves leaders in a unique effort providing frontline care during a pandemic."
Then, in mid-2024, came a new challenge: Two pharmacies, run by a national chain, located in Hardin County closed — one in Ada and one in a community about twenty miles away. By reports, the Ada pharmacy that closed was a location filling about 500 to 600 prescriptions a day — with an unknown tally of the many other services those pharmacists provided their customers and prescribers.
Beatty pointed out that pharmacy closures are challenges most pharmacy schools don't navigate. But, in their rural Ohio area, those closures created a serious service gap.
"Our university pharmacy was the only pharmacy in about a 20-mile radius," he said. "Services were needed and it was what we did: We stepped in to fill the needs of the community and our pharmacists stepped up. They put in a lot of work."
The ONU HealthWise pharmacy experienced a tripled prescription volume.
Musser and Rush described the closure's impact on their learners' experiences both in the local pharmacy and the HealthWise Mobile Clinic.
"For our students?" Musser said. "They need those experiences of working in a pharmacy, different from the mobile outreach experiences. This closure allowed them to experience firsthand what a rural pharmacy closure actually does to rural communities."
"However, the closure also resulted in a huge geographical area that needed service and the mobile clinic was now needed as a conduit for medications," Rush added, explaining that HealthWise began expanding mail order prescription services and offering delivery services with the HealthWise Mobile Clinic now going to some areas several times a week.
But there was yet another HealthWise service: Musser shared details of their pharmacy call center's work.
"Our pharmacy call center makes calls and takes calls from patients and providers when our mobile services aren't in the communities," Musser said. "Those follow-up calls include clarifying medication lists, monitoring medication adherence, and reviewing patients' home monitoring values among other things. These activities actually allow us to provide a continuity of care for our mobile clinic patients and our pharmacy users."
But Is Success Sustainable?
In rural areas, even the most successful of services often become financially unsustainable. Beatty said ongoing support for their work is multi-channeled. First, because the outreach work done by the HealthWise team and the ONU student pharmacists generated community trust that allowed the team to provide care in areas other services haven't been able to reach, Beatty said he believes this trust contributed to the $500,000 state legislative support received in 2025.
That award allowed HealthWise Mobile Clinics to become a plural, supporting the addition of a second van that will increase rural outreach. Other funding sources include Ohio's Charitable Health Network membership, various grant awards — with application work completed by ONU pharmacy faculty themselves — and because Ohio pharmacists have "provider status," some billable pharmacist services.

National Numbers: Rural Pharmacists and Pharmacies
ONU, with its dual focus, is impacting both rural pharmacy services and pharmacist numbers: the former with their mobile clinics and the latter with their unique rural locations for pharmacist training.
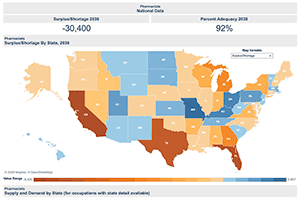
However, what's the nationwide view? Are the nation's pharmacy schools graduating enough pharmacists to be practice-ready for working in rural pharmacies?
While there are additional pharmacy programs providing rural-focused training, perhaps a comprehensive answer starts with reviewing federal workforce projections for the year 2038 that indicate the nation's pharmacist supply will be 92% adequate.
But rural pharmacist numbers aren't counted. Instead, a surrogate number often used is rural pharmacy numbers. Research reveals that there are both urban and rural areas where community residents have low or no access to nearby pharmacy services. Specific to rural, one report using data from the 48 mainland states found that a total of around 4 million people — nearly 20% of the nation's rural residents — were living in pockets of rural areas that were served by a single pharmacy.
Types of pharmacies also differ in rural America. Rural health policy researchers found that national franchises were less common in rural areas, with most communities served by regional franchises and local pharmacy businesses. Additionally, that report also suggested that regional chains have lower turnover rates perhaps because pharmacists at these sites often consider themselves an essential part of local healthcare and are involved in the community.
Rural Readiness: A Pharmacist's Track to Licensure and Independent Practice
Like physicians, there's a many-years path to
independent practice. Musser details their pharmacist
pathway to independent practice.
"Although ONU is unique in that we are one of a few colleges offering a '0-6 program' — meaning many of our students start pharmacy school out of high school and complete the degree in 6 years — the usual path is someone taking two to four years of college-level pre-requisite courses, the latter usually coming with a college degree," she said. "When pre-requisites are completed, next comes four years in a professional pharmacy program with a doctorate degree at graduation. At that point, graduates must pass a national standardized exam for licensure."
Later, she said, a pharmacist might also spend one or two years in a residency or fellowship where they gain even more expertise. Accredited pharmacy training programs must follow standards set by the Accreditation Council for Pharmacy Education. Examples of training themes include communication, person-centered care, and leadership skills.

Emily Eddy, PharmD, an ONU associate professor of Pharmacy Practice and a 2026 National Rural Health Association Rural Health Fellow, said she understands the importance of incorporating those themes into their program. She's the co-director, along with Musser, of RUHSP, the ONU program offered not just to pharmacy doctoral candidates, but nursing students, with all participants in the final years of their professional programs. The RUHSP curriculum includes rural practice experiences and seminar courses that include leadership development training.
Noting leadership skills as especially strategic for rural practice readiness, Eddy said those skills, in particular, are needed for their program's mandatory community-based project, done in collaboration with local agencies. She explained the program's focus: identifying a healthcare need and then both designing and implementing a solution, followed by a programmatic evaluation of the solution.
"We want our graduates to be problem solvers," Eddy said. "To do so, we're providing them with actual experiences in solving the unmet needs and problems they're sure to encounter in rural areas, rather than just waiting to be asked to sit at a table or be invited to participate in similar processes. We want them to have confidence that, as pharmacists, they can lead and accomplish innovation."
The program, which offers a certificate, is now in its sixth cohort. Eddy went on to share more about the mandatory projects.
"Not all projects achieve their intended outcome," she said, emphasizing that those outcomes are as important for the faculty advisors as for the students. "Every participant learns, reflects, takes something away from their project. I've been so impressed — and sometimes actually moved to tears — that even when not meeting success, learner idealism doesn't fade. These participants still want to go out and make a difference, taking with them the answers to their questions, 'What have I learned? What would I do differently?' They seem to develop something I'd describe as 'experienced idealism.'"
The PharmD Graduate Perspective

Katie Prater Kirby is an ONU PharmD graduate, a previous RUHSP participant and now a PGY1 (post-graduate year one) resident in ONU's rural residency with the ONU HealthWise Mobile Clinics. She said she's also from a rural community near ONU. In choosing ONU with its rural presence and a pharmacy program, she said she believed she'd be able to accomplish her career goal of providing healthcare to her rural community. She described how that's exactly what's happened during her education experiences — including her early work as a student "swabber," the job description of those doing nasal swabs for COVID testing, during HealthWise's pandemic outreach work.
Now in her advanced training, she said she believes she's continuing to gain even more firsthand appreciation for what an Ohio rural pharmacist with provider status can actually bring to a rural community.
"As a pharmacist, we are more than medication specialists," she said. "We have a whole-patient approach. Sometimes in those interactions, I've found I'm the one who's become aware of a patient's health need not uncovered by or shared with any other provider. We've been trained in this program that it's a pharmacist's responsibility as much as anyone else's responsibility to provide assistance for that need. And sometimes? The pharmacist is actually the best-positioned professional to help."

