Jan 22, 2020
Physician Burnout: Definition(s), Cause(s), Impact(s), Solution(s)
This is the first in a two-part series on rural physician and provider behavioral health. Read part two – Healthcare Professionals' Mental Health Needs: Where Can They Go?.
 "We see these elevated risks in
suicide in all the caring professions, whether it be
dentists, human medicine, or animal medicine," Dr. Chris
Bundy, psychiatrist and president-elect of the Federation of State Physician
Health Programs (FSPHP) said, providing a perspective
on physician suicide and burnout. "We can debate each
study's outcomes, odds ratios, methods, and time
intervals. We can express our concerns about how suicide
is a stigmatized cause of death that impacts death
certificate accuracy. But no one can argue this: any
number in any of these professions is just too high."
"We see these elevated risks in
suicide in all the caring professions, whether it be
dentists, human medicine, or animal medicine," Dr. Chris
Bundy, psychiatrist and president-elect of the Federation of State Physician
Health Programs (FSPHP) said, providing a perspective
on physician suicide and burnout. "We can debate each
study's outcomes, odds ratios, methods, and time
intervals. We can express our concerns about how suicide
is a stigmatized cause of death that impacts death
certificate accuracy. But no one can argue this: any
number in any of these professions is just too high."
Bundy noted the Centers for Disease Control and Prevention's 2019 report on veterinarian suicide and also said there would be benefit to having a similar, more robust look into physician suicide and related data in a very structured fashion.
"We don't have a very good estimate of current physician suicide mortality data," he said. "I think there is a lot of speculation that there might be a link between physician burnout, distress, and suicide. But there's no hard data to support that conclusion. However, there is data that suicidal ideation is increased in medical students, residents, and for populations struggling with burnout. Furthermore, there's data that higher rates of depression exist in individuals experiencing burnout. Given that data, we do seem to be in an epidemic of physician burnout, distress, disillusionment — whatever the label being used in the discussion, or all of those things — and that must have attention."
Burnout: The Definition(s)
Some experts suggested that an indicator of the gravity of what's happening with physician burnout might be judged by the number of words and phrases used to describe the issue. For example, phrases like physician wellness, provider well-being, work-life integration, and work-life balance — a frequent phrase that researchers point out is actually without a well-constructed framework — give a positive frame to the issue. Other phrases, like moral injury, provide a different tone. Words like "distressed" are also found in front of "physician," "healthcare provider," or "clinician."
The World Health Organization's (WHO) description seems to be the standard: burnout is "phenomena in the occupational context and should not be applied to describe experiences in other areas of life." WHO emphasizes that it is not a medical condition. Experts writing in a 2015 paper with respect to creating public health policies for burnout offer that the "current state of science suggests that burnout is a form of depression rather than a differentiated type of pathology." Other experts provide a more fine-tuned definition: Burnout is a job-related stress syndrome resulting in emotional exhaustion, depersonalization, and reduced personal accomplishment.
Burnout Solution(s): Approaches for Medical Students, Women Physicians, and Employed Physicians
Experts said that although it's taken time for physician burnout to reach a critical threshold, many now describe it as an "epidemic." The past few years have seen organizations stepping up to help their workforce cope with the physical and emotional demands since research suggests the demands associated with the current models of healthcare delivery in the United States are an important contributor to burnout. Several rural examples illustrate what can be done for rural healthcare workforce trainees and individual practitioners and at an organizational level.
Rural's Future Doctors: Medical Students
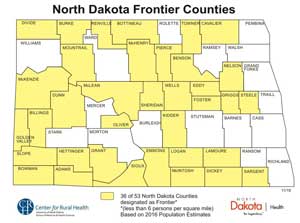
Building on the concept that practicing physicians can be healthier when their own physical and mental health needs have been integrated into medical training from day one of entering the profession, the University of North Dakota School of Medicine and Health Sciences (UNDSMHS) supports medical student and resident wellness with a program implemented in 2016. Michelle Montgomery, a Licensed Clinical Social Worker with the school's Psychiatry and Behavioral Science Department, is the Wellness Coordinator for the school's medical students. She talked about her role in a state medical school that has a purpose statement to "educate physicians and other health professionals and to enhance the quality of life in North Dakota," a state with nearly half its population located in rural areas and 36 of its 53 counties considered to be frontier.

"Students accepted into medical schools have characteristics that set them apart from their college peers," Montgomery said. "Once they get to medical school, due to the selection process they are now with a peer group where every member is elite. At this point in their careers, they begin to learn not everyone can be at the top. Students begin to make personal adjustments in relation to where they fit in this new peer group. That is also happening at the same time they're having to master a tremendous amount of complex information that's coming at them very quickly. This is hard emotional work. I'm here to assist students with their behavioral health, to talk about anything and everything, and to help them see that their mental health really matters," Montgomery said.
Though also connected with all medical students whether they are on campus or on rotation across or outside the state, Montgomery shared that her on-campus work with first-year medical students starts day one of the academic year. She said the first weeks pass quickly and wrap up with the students' first med school exams.
"These first exams are a sort of milestone when students see results that indicate they may not be as high-performing as they thought," Montgomery added. "It's not uncommon that these experiences trigger a student to even reconsider their career choice."

Montgomery also shared that med students working through their emotions is essentially work that provides an entry point to understanding the importance of self-awareness as part of overall well-being. Montgomery is quick to add that as a more self-aware student continues in their medical training, they eventually become a more self-aware physician.
"I work with students on their patient interviewing skills, especially around mental health questions," she said. "Students are more genuine when they're interviewing patients when they can say to their patients, 'I'm going to ask you some difficult questions. I ask them of all my patients and these are the same questions I have to answer, too' — that just makes a physician more human and less intimidating."
Again, the philosophy is that medical students who have a better understanding of their well-being will become residents who understand the importance of their personal well-being and will further become practicing physicians who not only have insight into their own personal well-being needs but can better discuss and assist their patients with well-being and mental health conditions. In 2003, the American Medical Association (AMA) articulated this hopefulness for the successive medical training tracks — medical school, residency, and eventual unsupervised practice — in their consensus statement on physician depression and suicide.
"Addressing depression and suicidality in physicians more decisively may have a multiplier effect for medical students, residents, and patients," the statement reads. "Treatment of mood disorders can lead to better physician mental health and productivity, fewer suicides, and better physical health. Because physicians' own health habits affect their health and prevention counseling, attention to their depression and suicidality may improve their mentoring and training of young physicians and may improve mental health care of patients."
More about the UNDSMHS Medical Student Well-being Program
Montgomery said that, as the Well-being Advocate for the students, she has both the full support of the medical school's administration and immediate access to the chair of the Department of Psychiatry and Behavioral Science Department for any needs or concerns. Montgomery also links two additional elements of the North Dakota program with its success: her physical presence in the building where the students' coursework happens and making it clear to students that she is their advocate.
"I share with them that there are strict boundaries of confidentiality when they come talk to me and that only changes if there is a concern of self-injury," Montgomery said. "They can tell me anything, nothing will shock me. And if anything needs to be elevated, I will do that anonymously."
How Do They Do It? Work-Life Balance for Women in Rural Family Medicine Practices
Schools like North Dakota, a state where 30% of the primary care physicians completed both medical school and residencies in the state, hope to see their wellness programs contribute to a healthy future physician workforce. As Montgomery pointed out, self-awareness is an important aspect of well-being. Dr. Julie Phillips, a family physician, clinical researcher, and associate professor of Family Medicine at Michigan State University, said she definitely saw an example of medical student self-awareness when a female medical student came to her with questions about practicing in a rural area.
"We have a rural program at Michigan State University where we really try to promote students to consider rural practice," Phillips said. "The student simply asked, 'How do they do it?' She wanted to better understand how women physicians practicing in rural areas are able to have children and yet keep up with the demands of rural medicine. Since I've not practiced in rural areas, my answer was just as frank: 'I don't know. I'll see if I can find out.' After doing a literature search, I found out there wasn't anything. So we decided to look into it."

Phillips said their team's research findings were quite remarkable. The investigators interviewed 25 women physicians from rural areas in 13 states, the majority located west of the Mississippi River and working in various practice structures ranging from the Indian Health Service to solo private practice. Three key strategies emerged: flexible work hours, clear boundaries set between professional and private life, and establishing supportive relationships.
"We didn't focus on physical and mental health of these providers," she said. "Instead, we looked at work-life balance in relationship to well-being. These physicians in those rural areas are passionate about their communities and love their patients and love patient care. They demonstrated the ability to navigate a difficult career and manage their personal life, something that is absolutely foundational to work-life balance and well-being."
Some experts said they see this research as timely given the fact that women comprise 50% of current medical school enrollment rosters. It might also be important if distant-past research findings regarding self-reported depression and suicide for U.S. women and U.S. women physicians were to hold true today.
Avera LIGHT: A Healthcare Organization Grows Its Own Formal Program

When first navigating the multifaceted efforts to build a program addressing physician wellness, Mary Wolf recalls only four other organizations also in the mix: Harvard's Brigham and Women's, Mayo, Stanford, and Vanderbilt. Wolf, program director for Avera Health's provider well-being program, called Avera LIGHT, said those early days of their program found her involved with crisis intervention and helping those who were burned out, distressed, or abusing substances. Now, she said, the program has matured where prevention is a focus for their urban and rural physicians alike: almost half of Avera's 645 physicians and 438 advanced practice professionals (APPs) practice in rural areas in five states, within about a 400-mile radius of the central operations and tertiary care center located in Sioux Falls.
Wolf said that this geography adds challenges since it is imperative that onsite presentations and meetings happen in order for providers to fully understand the offerings of the LIGHT program, to build trust in the program, and to personally meet her in order to see firsthand that she is a safe contact.

"At the core of our well-being program for physicians, nurse practitioners, and physician assistants is making sure they understand that the support is here for them from residency to retirement, for wherever they are on the spectrum of well-being," Wolf said. "We want our providers to enjoy medicine, stay with Avera, and provide great care for all of our patients. In that sense, LIGHT is also a recruitment and retention tool."
"Awareness about the program is growing and what we've recognized is the more we offer, the more physician engagement happens," Wolf said, also identifying Dr. Tad Jacobs, Avera's recently retired chief medical officer, as a major champion of the program-building efforts. "Most of today's successful physician wellness programs are related to the support of leadership at the top like we've had with Dr. Jacobs."

Jacobs, who had a 28-year career practicing full-spectrum family medicine before his executive tenure and then part-time until retirement, said he understands the importance of physician wellness. Because his dedicated clinical career was in rural South Dakota, he also understands firsthand the importance of looking after the well-being of the organization's providers in the more rural locations.
"Our organization said 'yes' to provider wellness early on," Jacobs said. "We've been developing a culture where we say to our providers, 'Look, you are important to us. We're investing in you to ensure that you're the best you can be so that you can be the best you can be for your patients.'"
Jacobs said that any organization that wants to formally address physician burnout will need to be prepared to present a business case for its existence. For Avera Health, physician turnover rate is a powerful data point. He shared how the program's first-year line item budget of about $150,000 was accountable to the financial structure of the organization.
"Our turnover rate is 3% to 4%, which is well below the national average," Jacobs said, noting that experts quote 7% as an average and that turnover has research linking it directly to burnout. "I remember in the third year of our program, I was asked to explain the financial benefits of the program. In the days when healthcare systems had operating margins of 4% to 6%, those turnover costs perhaps weren't seen as so critical. Now with systems looking at profit margins of less than 2%, pulling out the available data showing it can cost a million dollars or so to replace a physician makes the budget for provider wellness something to pay attention to. And any organization that has a rural footprint understands the difficulties associated with provider recruitment and retention, especially with the number of clinicians who feel comfortable in that setting decreasing dramatically."
Jacobs added that the current budget has now increased to around $450,000 and it is the organization's hope to increase program staffing to allow it to also support the organization's nursing, pharmacy, and administrative team members.
Organizational and Individual Strategies to Prevent Burnout
In the last few months, large healthcare systems are beginning to share their successful approaches to burnout in academic reports: for example, The Ohio State University (OSU). A school well known for its aviation program, its healthcare system adapted the aviation industry's Crew Resource Management (CRM) and combined it with Mindfulness in Motion (MIM) training. The researchers reported, "The improvements seen have not only improved patient satisfaction but also reduced patient safety events and improved national reputation for the institution as a whole."
In December 2019, a journal published two papers sharing approaches for dealing with burnout, one at the organizational level and the other at the individual level. Researchers from nine of the nation's largest academic healthcare systems, located from coast to coast, offered organizational-level strategies to "reduce physician burnout and improve professional fulfillment." (Table 1.) At the individual level, researchers from four medical schools provided suggestions for coping with the demands of work that "can result in mental and emotional exhaustion, self-isolation, burnout, depression, suicidal ideation and tragically, completed suicide." (Table 2.)
| Table 1. Organizational Strategies to Address Burnout | |
| Domain | Strategy |
| Culture of wellness |
Leadership development
Teamwork
Appreciation |
| Efficiency of practice |
Improve usability and interoperability of
electronic health record Workplace efficiency |
| Personal resilience |
Support health life-style behaviors
Peer support
|
Source: "Organizational strategies to reduce physician burnout and improve professional fulfillment." Current Problems in Pediatric and Adolescent Health Care. December 2019.
| Table 2. Individual Strategies for Cultivating Well-being and Resilience | |
| Category | Example |
| Occupational | Healthy limits; saying "no" |
| Finding meaning | Celebrating successes |
| Emotional and cognitive approaches | Address grief/disappointment |
| Personal and professional relationships | Appreciate and maintain both personal and professional relationships |
| Spirituality/Religion | If important, prioritize |
| Self-care | Emphasize participating in what brings personal joy |
Source: "Cultivating a way of being and doing: Individual strategies for physician well-being and resilience." Current Problems in Pediatric and Adolescent Health Care. December 2019.
Wolf and Jacobs also shared some of LIGHT's strategies:
- Program support requiring top-down leadership engagement to promote a well-being culture
- Clinical well-being champions in all five of the health system's regions
- Systemic approaches to promote well-being
- Executive coaching for any provider-requested topic
- For rural clinicians, often provided via Avera's telehealth on desktop or mobile device
- Program focus point examples:
- Provider connectedness
- LIGHT lunches for provider groups and those who practice in the system's service lines: for example, lab, X-ray, and oncology
- Schwartz rounds
- "No-agenda" socials
- "Safe zone" for distressed physicians: tactical approach rather than punitive
- Acknowledging differences between dilemmas and problems
- Mind, body, spirit approach consistent with the Avera mission
- Onboarding: LIGHT information for providers and spouses
- Spouse engagement group
- Well-being survey to pinpoint high-need areas
- Consultation for administrators and human resources professionals regarding challenging behaviors, change, conflict, and resources
- Well-being/LIGHT focus for physician and advanced practice provider leadership development programs
- Critical incident stress management services
- Retreats and CME opportunities
- Provider connectedness
Wolf said she provided 222 executive coaching sessions during the last fiscal year, 75% for physicians. She pointed out that rural physicians' needs are sometimes geared to addressing grief reactions since they become so close with their patients — not just due to geographical isolation, but because of the reasons the provider chose rural medicine in the first place: that potential to form tight-knit patient relationships. That same close connection sometimes also interferes with compartmentalization of their work: keeping their work in the workplace and not public spaces — and learning scripts for addressing patients who want that type of attention at the grocery store or children's sporting events.
Jacobs acknowledged the high number of monthly regional and national presentations and speaking requests Wolf must decline because of the current staffing model for the program.
"It'd be great to have a staff of eight or ten and we'd be on the stage with LIGHT," he said, noting those requests indicate word-of-mouth success of their program but also acknowledging they are still building their program and have more to accomplish. They've only recently hired a manager to allow Wolf to do more.
"Provider word of mouth has proved to be the key to increased engagement with the program," Jacobs said. "Our low turnover is proof it's working. And we're also learning that it's part of our growing footprint when providers come to us and say, 'We want to join you.'"
Resources
Federal Agencies
-
National Institute of Mental
Health
Depression
Suicide in America: Frequently Asked Questions
Suicide Prevention -
Substance Abuse and Mental Health Services
Administration
Physician-specific: DIMENSIONS: Work & Well-Being Toolkit for Physicians
Professional Organizations
-
American Hospital Association
Well-Being Playbook: A Guide for Hospital and Health System Leaders -
American Medical Association
Steps Forward -
Accreditation Council for Graduate Medical
Education
AWARE Well-Being Resources
Clinical Learning Environment Review (CLER) -
American Academy of Family
Physicians
Physician Health First -
American Academy of Physician
Assistants
Getting Ahead of Burnout: Experts Share Tips for Provider Well-being
Provider Burnout and the Risk of Malpractice -
Council of Residency Directors in Emergency
Medicine
National Physician Suicide Awareness Day, Sept 17, 2020 -
National Academy of Medicine
Action Collaborative on Clinician Well-Being and Resilience
Burnout Among Health Care Professionals A Call to Explore and Address This Underrecognized Threat to Safe, High-Quality Care

