Aug 09, 2023
In a Maternity Desert, a New Kind of Home Visitation Program Brings Care to At-Risk Mothers
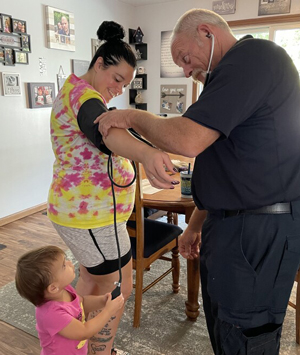
When Darren Forman's "baby phone" rings, he answers.
A young mother calling for help on a Friday evening after a domestic dispute. A pregnant 17-year-old girl stopped by law enforcement after a methamphetamine relapse. A woman in need of a listening ear following a miscarriage. Through the baby phone, expectant and new mothers can reach Forman at all hours of the day and night with questions, crises, medical needs, or just to talk.
Over the past five years, Forman and his team at the Crawfordsville Fire Department have provided education, support, and medical care to more than 200 women in Crawfordsville, Indiana, through Project Swaddle, a home visitation program in which a community paramedic brings wrap-around care to pregnant and postpartum patients. By bringing resources and support to women experiencing at-risk pregnancies or other social or environmental challenges, the program aims to keep patients from falling through the cracks in a maternity care desert.
"There were a lot of pregnant patients that were not showing up to their appointments and that were kind of falling off the healthcare radar," said Scott Sinnott, MD, an obstetrician based in neighboring Tippecanoe County who sees patients in Crawfordsville and the surrounding area. Under Project Swaddle, those patients "get better care, get much more attention, they feel better understood, and I think it inspires them to take care of themselves, too."
"We Have a Problem"
In Crawfordsville, a city of 16,000 and the county seat of Montgomery County, access to obstetric care became more limited after the local hospital, Franciscan Health Crawfordsville, closed its birthing unit in 2011.
Like "everybody else" in Crawfordsville, Mayor Todd Barton was "upset" about the closure, he said. But Barton, who was working at the time as a firefighter and paramedic with the Crawfordsville Fire Department, also recognized the grave implications for women's healthcare in Montgomery County: "It's no longer a situation where we're 10 minutes from a hospital," he said. "Now, we're 45 minutes to an hour from a hospital where you can get those kinds of services."
Five years later, Barton was saddened but not shocked when a community needs assessment revealed a gap in care and resources for mothers and babies in Montgomery County. But the severity of the issue came as a wake-up call for many community members and leaders, including first responders.
A lot of moms were missing appointments and nobody had really stopped to ask why.
At that point, "We realized, 'Oh boy, we have a problem,'" Forman said. "A lot of moms were missing appointments and nobody had really stopped to ask why."
Barton and other city and county leaders leapt to action to find solutions. Before long, they turned to the Crawfordsville Fire Department, which had already begun to launch a home visitation program focused on chronic disease management. With that foundation laid, the department decided to pivot to try something new: shifting the focus of the home visitation program to moms and babies instead.
With a partnership with Franciscan Health Crawfordsville established, an early version of Project Swaddle was formed, centered on connecting mothers to obstetric care, transportation, and social services as needed. But conversations with Sinnott, who had paired up with the fire department to oversee the program while providing care to patients during visits to Crawfordsville, made Forman realize that the program could be doing more to help high-risk mothers manage their care. From there, Project Swaddle expanded to offer in-home care to at-risk mothers, with Forman able to administer medications and IVs, perform tests, and monitor conditions such as gestational diabetes during visits.
Since then, Project Swaddle has expanded into a mobile integrated healthcare program offering wrap-around services to pregnant and postpartum women, with a holistic approach that requires coordination between paramedics, physicians, nurses, social workers, and other service providers in the community. Patients can enroll in Project Swaddle as early as the first trimester of their pregnancy and receive care up to 90 days postpartum; the program is in the process of expanding to serve mothers up to one year postpartum.
"We like to say the program is physician-led but patient-centered," said Samantha Swearingen, Project Manager for the Crawfordsville Fire Department.
The "Why"
As Project Swaddle came to life, the "why" of all those missed obstetrics appointments became clearer to Forman. For some patients, unpredictable work shifts led to timing issues. In families with one shared car, some mothers had no way to drive to their appointments while their partner was at work. Others were unable to afford gas money for regular trips to the doctor.
Some patients didn't face physical barriers to care, but reported feeling intimidated or unheard during appointments, especially when meeting with busy practitioners who might not have time to sit and answer all of a patient's questions.
"We heard a lot of, 'Why was I even there?'" Forman said. "'They come in and ask me how I'm doing, maybe measure my belly, and tell me to come back in two weeks. Why did I bother?'"
Over time, Forman learned that education — and someone willing to sit down and answer all of a patient's questions, patiently and without judgment — was something many Project Swaddle participants were craving. Those who attended birthing classes "were coming back with more questions than answers," Forman said.
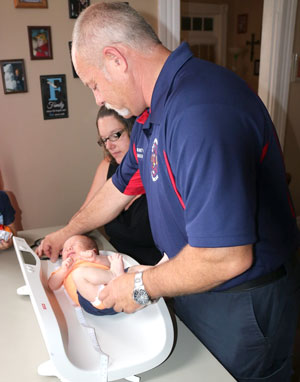
In some instances, these one-on-one conversations between Forman and his patients have saved lives: Forman gives the example of one patient who was able to recognize when she began experiencing preeclampsia symptoms and get herself to the hospital quickly after discussions preparing her for the possibility. Other educational conversations might revolve around infant safety topics, such as safe sleep practices and car seat usage, how to choose a bottle, or what to expect during delivery.
At any given time, Forman estimates that he is working with 15 to 20 mothers on average, making five one-hour-long visits on a typical day. Home visits usually occur every two weeks until the 36th week of pregnancy, at which point they increase in frequency to once a week, although this timeline varies from patient to patient. Visits also tend to look different from patient to patient; a visit might include any combination of a medical check-up, testing, medication administration, a general wellness check, and education on prenatal and postpartum care.
With Forman monitoring his "baby phone" during all waking hours, patients can also have their questions answered with near immediacy outside of designated visit times, whenever symptoms or concerns may arise.
"If you call your doctor's office, you talk to a machine or a nurse, and hopefully somebody gets back to you later in the day," Forman said. "If you're an at-risk mom and you feel something or your friend told you a scary story, you're anxious and you're waiting on a phone call that may or may not come back. They can call us, or they can text us, and we'll give them some real-time answers."
From Sinnott's perspective as a physician, patient feedback from the program has been "overwhelmingly good," he said. "They feel like they have an inside voice, or an inside track, to get information and care. For them, it's as easy as sending a text to Darren and him responding right away, and then him calling me if it's something that he feels like they need to be seen for."
And for Forman and his patients, the baby phone works both ways: If a patient doesn't show up for an appointment at the doctor's office, he calls them to check in and offer a ride. Sinnott recalls Forman following up with one mother in particular who hadn't shown up to an appointment: a woman who was homeless at the time. Forman tracked the patient to an encampment under a highway overpass and brought her to her appointment.
"The Right People"
As a male firefighter in his fifties, Forman may not be the first person who comes to mind as a guide and confidante for new mothers.
"Initially, that was one of my fears — could he do this job and connect with patients?" said Paul Miller, EMS Division Chief for the Crawfordsville Fire Department. "And, resoundingly, he has knocked it out of the park. He's been able to connect with all our obstetrics staff, our physicians and providers, and, most importantly, the patients.
"At this point, he's almost regarded as an icon in the community," Miller added. "I'm surprised I haven't seen T-shirts with his face on them."
To gain the trust of patients, Forman and his colleagues take an approach that emphasizes transparency and a "non-judgmental" attitude. Using motivational interviewing techniques and with social determinants of health in mind, the Project Swaddle team helps patients map out their goals and priorities, then works with them to achieve those goals.
We help them decide where they want to be. Once we line this path out, then it's just a matter of helping them walk along it.
"We help them decide where they want to be," Forman said. "Once we line this path out, then it's just a matter of helping them walk along it."
For some Project Swaddle patients, "Darren is the first person who has really been an advocate for them and shown up for them," said Sarah Frier, a nurse with the Franciscan Health Network who works with Project Swaddle patients in Crawfordsville and nearby Lafayette.
"Darren makes sure they have diapers and formula and medicine and supplies and housing, and he does things for them that we wouldn't be able to because we don't have enough time in the day," Frier said. "A lot of these patients have never had anyone do things like that for them."
Having "the right people" involved is crucial to the success of a program like Project Swaddle, Miller said: "When you meet with anyone involved in this program, you can see the passion they have for this kind of community outreach." He and Forman both attribute the program's success in large part to Forman's twenty-plus-year career as a paramedic and his years of experience working as an emergency care technician in the emergency room, both of which helped him build trust and establish relationships in the Crawfordsville community.
"It's not something that's going to be for everybody," Forman said. "You're going to run up against roadblocks.But just having the passion to answer the phone when you need to, and to go out even if your day was scheduled to end at four o'clock and somebody calls you at 4:30 on a Friday afternoon — you do what you need to do."
The Bigger Picture
To help other communities who want to start a similar program, Project Swaddle organizers have created a how-to guide with best practices. Swearingen notes that the Crawfordsville Fire Department was fortunate to have already had a relationship with the Franciscan Health Network after partnering with the local hospital for previous programs, making it easier to establish a partnership for Project Swaddle. Having "passionate, dedicated practitioners" has also "been huge for us," Swearingen said. Still, funding has been an ongoing challenge for the program, organizers say. After initial funding through a one-year grant from the Montgomery County Community Foundation and the Indiana Department of Health, the program is primarily funded today by the Franciscan Health Network and the city of Crawfordsville.
"It absolutely requires a community to come together, and you have to break down walls and silos — that's the secret to something like this being successful," Barton said. "You have to break down those barriers and get people to understand that this is about the bigger picture."
Patience has also been key to Project Swaddle's success, program organizers say. Miller encourages other communities to "start small, with achievable goals," and to set metrics that will be achievable, "because success breeds success."
With more than 200 patients served by Project Swaddle since its launch in 2018, the program has been able to recognize patterns in its patient outcomes while tracking metrics such as breastfeeding rates and pre-term delivery. A nearly-identical program — Project Bundle — that uses nurses rather than paramedics to reach patients outside of the Franciscan Health Network has also been established through partnerships with other providers in the region.
"There's definitely success in the data we've collected so far," said Swearingen, noting that a number of Project Swaddle's metrics appear to align with, and in some cases surpass, similar programming at a national level. Swearingen and other program organizers are in the process of digging more deeply into this data and pulling other metrics, such as emergency department visits.
For Forman, the program's impact can be measured in "big old bear hugs" at the grocery store and texts on Father's Day. Many of his stories end in healthy deliveries: The mother who called for urgent help dealing with law enforcement on a Friday evening after a domestic dispute went on to deliver a "beautiful, healthy baby boy." The teenager who asked police to call Forman after she was pulled over with methamphetamine in her car recently gave birth to a "bouncing baby boy," and calls Forman regularly "about all kinds of stuff." And the mother who Forman visited weekly after her miscarriage, so that she had someone to "bounce things off of," called him nine months later to share that she was pregnant with her daughter.
This is something where you can really see the difference that it's made in people's lives.
"This is something where you can really see the difference that it's made in people's lives," Barton said. "The real impact is really something that we can't measure. Because the cost of an NICU stay, yeah, we can put a dollar on that. But the lifelong implications of a healthy birth are profound."

