Nov 30, 2022
Aiming For 'Real and Accessible': EMS Simulations Give Rural Providers Hands-On Experience
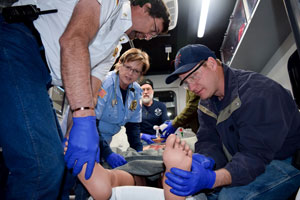
Rural EMS providers tend to have fewer opportunities to practice their skills on the job than non-rural providers, recent research has found — and the difference may impact the quality of care that patients receive.
A study published earlier this year by the University of Washington's WWAMI Rural Health Research Center (RHRC) confirmed what many rural EMS professionals had already known: When it comes to gaining firsthand exposure to relatively rare medical events, rurality can be a disadvantage — and the more experience you have with a certain procedure, the more comfortable you'll likely be performing it.
The good news, EMS leaders and experts say, is that simulation tools to provide rural agencies with the next-best alternative to on-the-job experience are growing and evolving, giving rural providers more opportunities to practice their skills in a hands-on, real-time context. While not a direct replacement for working on living, breathing patients — and not without their own challenges — tools such as high-fidelity mannequins and virtual reality technology can help rural EMS providers become more comfortable in high-stress situations.
How do we make them as real as possible and as accessible as possible?
"These simulations are what we've got," said Brad Blackwell, EMS Division Chief for the Telluride Fire Protection District in southwestern Colorado. "How do we make them as real as possible and as accessible as possible?"
Overcoming 'Reality Shock'
The WWAMI RHRC study found that the more accumulated time the lead EMS professional on a given call had spent on 911 responses, the more likely the patient was to receive evidence-based care for conditions including seizure and trauma.

"Even if you've been well-trained, if you're not using a skill often enough, it will get rusty over time," said Davis Patterson, PhD, Director of the WWAMI Rural Health Research Center and co-author of the study. The research found a "clear trend away from providing evidence-based care with increasing rurality," Patterson said.
In comparing urban and rural agencies, the research found that rural EMS professionals tended to respond to fewer daily calls on average and that rural agencies were generally less likely to provide evidence-based care than non-rural agencies.
"We designed the study to try to identify whether those things were actually true, because they're often discussed — but just at the agency level or the community level," said study co-author Nick Nudell, a Colorado-based paramedic scientist and president of the American Paramedic Association. "This now gives us a launching point to be able to move forward with addressing those gaps."
This now gives us a launching point to be able to move forward with addressing those gaps.
The fact that rural EMS providers often find themselves traveling longer distances likely contributes to these disparities in accumulated experience, Patterson said — and, as the report noted, makes it all the more important that rural providers feel comfortable handling all kinds of patients for extended periods of time.
Training with high-fidelity mannequins can help keep muscle memory sharp for performing a particular procedure, Nudell said. Practicing for the less predictable elements of a call — such as interacting with a distraught family member — can be trickier.
"Reality shock can set in when you're dealing with the sights and sounds and smells and sensations of an actual call," Nudell said. "So we try to make training as realistic as possible, so providers will be more comfortable when the time comes and won't be distracted or triggered by elements of the real world."
Simulations on the Move

One of the largest and best-known EMS simulation programs in the U.S., Simulation in Motion (SIM) has grown to establish presences in Iowa, Montana, North and South Dakota, and Nebraska.
In Nebraska, where nearly 9 in 10 EMS agencies serve rural or frontier areas, the program primarily delivers training to rural parts of the state, said Simulation in Motion—Nebraska (SIM-NE) Program Manager Douglas Dekker. Using four mobile simulation labs, SIM-NE has the ability to bring more than 60 simulation scenarios to rural agencies using computerized mannequins that can talk, breathe, display a range of symptoms, and respond to treatments using a built-in algorithm.

With trainings conducted in towns as small as 60 people, SIM-NE offers its services at no cost to participating EMS agencies to keep the program affordable for rural departments; funding from the program thus far has come primarily from philanthropic support. SIM-NE has held roughly 700 trainings across the state since the program launched in 2017, with more than 150 agencies hosting multiple training sessions over the years.
They're hungry for something different than death by PowerPoint.
"People are hungry for the training," Dekker said. "They're hungry for something different than death by PowerPoint."
While the SIM-NE program is housed in the University of Nebraska Medical Center in Omaha, the paramedics and nurses who make up the SIM-NE training staff are based around the state, with staff members living and working in their designated region: Staff based in the western part of the state, for example, are from that part of the state.
"We really work hard to make sure that our staff connects to the area they are providing training in," Dekker said. "They relate to the language, the geography, the values. There's an understanding of nuances of very rural areas of the state, the often-long EMS transports to hospitals, and the lack of reliable cell phone service that creates an inability to communicate with their medical control doctors during transport."
The Ten Percent
With child patients accounting for roughly 10% of EMS calls — and just 10% of those calls involving critically ill or injured children — some simulation programs take a specialized approach, focusing solely on pediatrics.
Because pediatric calls are relatively uncommon, many EMS providers find them particularly stressful, said Blackwell, the EMS Division Chief in Telluride.
"We don't do them much, but when we do them, they can be scary," Blackwell said.
"From the moment that EMS professionals are called to respond to a child, their anxiety and stress levels are already elevated," said Nicolena Mitchell, Program Manager for EMS for Children (EMSC) Colorado, a statewide program operating a mobile pediatric simulation lab. "And when you don't have opportunities to practice your skills and become repetitive and increase that competency, there is an increased level of anxiety."
Dr. Kathleen Adelgais, a professor of pediatrics at the University of Colorado's School of Medicine and Project Director for EMSC Colorado, estimates that 60-70% of the agencies served by the mobile simulation lab are rural: "The large majority of agencies are rural," she said, "because most urban agencies actually have the resources to do some of their own trainings."
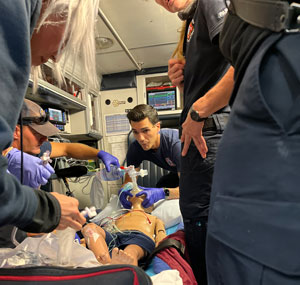
After a period of tamping down travel due to the COVID-19 pandemic, the program has begun to increase the frequency of its trainings again, Mitchell said; a new simulation ambulance that fares better in the snow than EMSC Colorado's previous truck and trailer also allows the program to more easily travel year-round.
"I think if we had enough staff and enough time, we would be on the road every week of the year at the rate in which requests are coming in," Mitchell said.
While some agencies take advantage of the vehicle's built-in simulation lab, others prefer to conduct trainings with EMSC Colorado's high-fidelity mannequins inside their own ambulances.
"It's like working in your office — that's where you're most comfortable," Mitchell said. "I think the benefit of this program is that we are able to be really nimble. We can bring what is needed to that agency at that time."
EMSC Colorado's mobile simulation lab program was initially grant-funded but now charges a small distance-based fee to cover ongoing costs such as oil changes, vehicle maintenance, and insurance. The program is currently in the process of reevaluating this model, Adelgais said.
"We recognized that there was going to need to be a small business model to keep the lab on the road, but I think it does disadvantage the rural communities that have to pay a little bit more," Adelgais said. "We're re-looking at that right now to make sure that our way of doing this continues to be sustainable."
'Striving To Be Better'
The Telluride Fire Protection District has participated in EMSC Colorado's mobile simulation lab training twice; Blackwell, the EMS chief, said he hopes to make the training an annual event.
For small departments like Telluride's, "simulation is generally the mode of education," Blackwell said. "The goal is to try to stress our providers in the same way they'd be stressed in a real-life environment. It's impossible to match it 100%, but we're always striving to be better."
One aspect of a real-life call that can be difficult to replicate using high-fidelity mannequins is human emotion, especially on tense pediatric calls.

"What mannequins can't do is replace walking into a real call where there's a child screaming," Blackwell said. "And it's hard to simulate a freaked-out parent."
One strategy for simulating real human emotion: using real humans. SIM-NE is currently piloting the use of standardized patients — actors given a script — to play, for instance, the spouse or parents of a patient during simulation trainings.
"Having a standardized patient in there brings it to another level," Dekker said. "The whole program has been very well received, but the standardized patients have been very, very well received when we bring them in."
The limited availability of human actors makes it unlikely that standardized patients will ever be incorporated into every SIM-NE training, Dekker said. But he hopes that, eventually, the program will be able to use them more frequently.
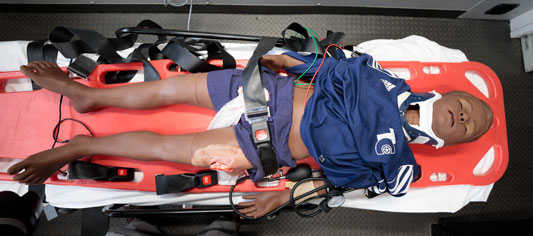
Other aspects of the job that can be difficult to replicate exactly, according to Blackwell, are the timeframe of calls, particularly for rural agencies that need to travel a long distance to reach patients or the nearest hospital, and environments that are particularly tricky to handle and move patients around in.
For many rural agencies, accessing state-of-the-art simulation tools is a challenge in itself.
"There's a lot of access to equipment and education and facilities in urban areas," Blackwell said. For rural communities farther removed from the amenities of Colorado's metro areas, high-fidelity mannequins and other simulation tools are likely too pricey for most individual departments to purchase — but Blackwell sees a future in small, rural agencies pooling their resources to establish regional simulation training centers.
"I think that's the route we really need to go to try to continue this work," he said.
A Virtual Approach
In Maine, EMS providers have begun to use a different kind of simulation tool: virtual reality.

Maine EMS, the state EMS bureau, had looked into buying high-fidelity mannequins to help agencies across Maine practice for pediatric calls — but the price of the mannequins and the thought of hauling a mobile simulation lab cross-state in New England winters made the idea feel impractical.
With grant funding from the Health Resources and Services Administration (HRSA), the Maine EMS for Children program instead purchased five virtual reality (VR) headsets that simulate the experience of responding to pediatric calls. The headsets' compact size makes them easier to transport than mannequins and offers the flexibility to mail, rather than drive, them to far-flung agencies when necessary.
Mannequin simulations and VR simulations aren't exactly comparable, as the two tools target different aspects of the first responder experience: High-fidelity mannequins "help with anxiety around the skill itself and handling different devices," said Marc Minkler, Program Director for Maine EMS for Children. The type of VR simulation used in Maine, in which EMS professionals don't actually touch the patient, deals "more with the human side of it and less the technical side of things" — assessing symptoms and determining the best course of action, all while interacting with distressed patients and upset family members.
More traditional EMS assessment training models, in which the trainer might play the part of the patient, can be difficult to apply to pediatric training, especially for calls involving very young children, Minkler noted.
I can't look at a two-year-old and say, 'Okay, pretend you're hurt.'
"If you're in my EMT class, I can simulate that I'm having a heart attack by telling you that I have chest pain and clutching my chest, or I can present as a person who's confused and disoriented," he said. "You can't do that with a baby. I can't look at a two-year-old and say, 'Okay, pretend you're hurt.'"
The patients in the VR simulation are all under five years old and unable to articulate their symptoms as an older patient could; in some of the scenarios, the child screams throughout, adding to the stress of the situation.
"It's not going to teach you how to intubate a patient," Minkler said. "But it teaches you what is sick and what is not sick, what is critical and what is not critical, and it gives you a litany of patients in a very short time that shows a breadth of conditions in a way I've never seen before."
Four communities in Maine — a mix of urban and rural — were served by the initial pilot program; the headsets have since been made available to any EMS agency in Maine. Maine EMS has also begun to expand its virtual reality programming beyond pediatrics.
Safety and Comfort
While the headsets' portability makes them well-suited for reaching remote rural areas, they require a reliable wireless internet connection to work — a condition some rural agencies may struggle with. VR training may not be a good fit for every individual, either: One trainee in Maine experienced vertigo after putting on the headset, and the fully immersive experience of being in a virtual environment designed to be stressful has the potential to trigger post-traumatic stress or other anxiety disorders in trainees, Minkler noted.
"There has to be some measure of safety and comfort," Minkler said. "I tell service leaders, 'You can't require this.'"
There has to be some measure of safety and comfort.
Even for those who are well-suited for VR training, the experience will likely be a little bit uncomfortable — but that discomfort is the point. One trainee was initially hesitant to put on the headset, Minkler recalls, after having been on some particularly stressful pediatric calls in real life. The simulation produced a similar wave of anxiety as the real calls had, the trainee told Minkler, but by the time they finished the training they'd seen more child patients in the span of a half-hour than they had in the previous two years.
A few days later, Minkler received a call from the same trainee. They had received a real pediatric call that day, the trainee told him — a bad one. But the call had been remarkably similar to one of the simulated scenarios they had experienced in training earlier that week.
"I thought, I've already done this call," Minkler recalls the trainee telling him over the phone. "I was able to assess the kid and their needs, and I didn't have the anxiety. I walked away going, I did good. I did it."

